In recent years, the field of biodegradable implants has undergone a transformative shift, thanks to the integration of AI in biomaterials and medical engineering. This evolution has moved us away from traditional trial and error methods toward a more precise, efficient, and intelligent process. Advanced algorithms now accelerate every stage from design and manufacturing to post implant monitoring. As artificial intelligence continues to influence global innovation, it’s crucial to dive deeper into this revolutionary fusion and understand its impact on the future of medicine. Let’s explore!
What Are Biodegradable Implants?
According to leading global medical institutions, biodegradable implants are medical devices designed to support or replace damaged tissues or bones inside the body. Over time, these implants naturally degrade into harmless components that are either absorbed or expelled by the body. This innovation presents a safer and more adaptable alternative to traditional permanent implants such as metal or plastic which often require additional surgeries for removal after healing.
The degradation rate of these implants depends on the type and structural composition of the material, allowing healthcare professionals to customize the duration of biological support based on the patient’s specific needs and the nature of the injury.

The Importance of Biodegradable Implants in Regenerative Medicine
Biodegradable implants play a critical role in the advancement of regenerative medicine. Their ability to support tissue healing without the need for follow-up surgeries significantly enhances patient recovery. These implants gradually dissolve after fulfilling their biological function, minimizing post-operative complications and surgical burdens.
By offering a smart and safe alternative to permanent implants, biodegradable devices improve clinical outcomes, especially for complex injuries or patients with chronic conditions. They also reduce emotional and physical stress, making treatments more efficient and patient friendly.
How AI Is Transforming Biodegradable Implant Design
As medical technology rapidly advances, artificial intelligence (AI) has emerged as a transformative force in the design of biodegradable implants. Traditional biomedical engineering standards are now being redefined, with AI in biomaterials enabling researchers to achieve unprecedented levels of precision and innovation. Let’s explore how this cutting-edge synergy is reshaping implant development.
1) Microscopic Structural Design with Machine Learning
- Machine learning algorithms play a vital role in analyzing thousands of biological engineering samples to extract the optimal porous structures. These designs aim to strike the perfect balance between mechanical strength and degradation rate.
- Artificial Neural Networks (ANNs) are trained on real-world mechanical data, generating precise implant structures that support fluid flow and nourish bone cells without compromising durability. This level of microstructural control would be nearly impossible without the capabilities of AI.

2) Numerical Simulation and Advanced Modeling Strategies
- The design process of biodegradable implants greatly benefits from finite element methods (FEM), which simulate real-world body forces acting on the implant. These simulations help predict deformation and stress distribution before the manufacturing stage begins.
- By integrating AI in biomaterials, researchers can refine these models further. Continuous training using laboratory and clinical test data allows AI systems to enhance simulation accuracy and bridge the gap between virtual predictions and real-life performance. This dramatically improves both the safety and efficiency of the final implant.
Also get acquainted with: The Role of AI in the Early Detection of Diseases through Medical Imaging
Smart Material Selection and Manufacturing
The success of biodegradable implants relies heavily on the careful selection and advanced manufacturing of smart materials. This phase is crucial for achieving the ideal balance between biocompatibility, durability, and controlled degradation.
1) AI-Powered Evaluation of Chemical Compositions
- Both natural polymeric membranes (such as collagen and gelatin) and synthetic ones (like PLA and PGA) are commonly used in implant procedures. Through AI in biomaterials, thousands of material compositions can be virtually screened to identify the most suitable options based on biological, mechanical, and degradation criteria.
- Molecular interaction modeling techniques—such as pharmacophore modeling—are applied to replace highly inflammatory components with atoms or functional groups that minimize immune responses. This process significantly enhances the safety and biocompatibility of the implant.
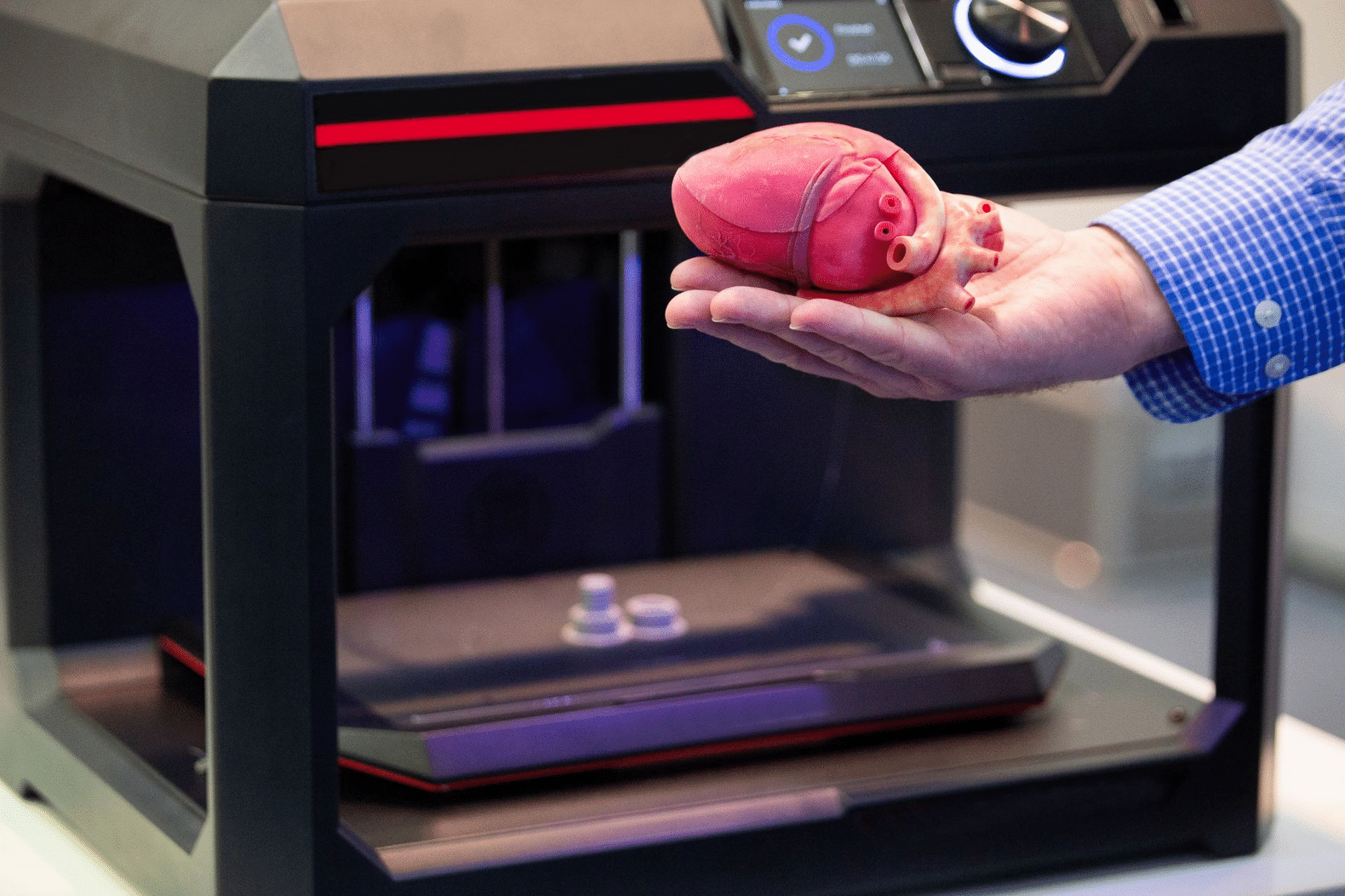
2) Additive Manufacturing and 3D Bioprinting
- 3D bioprinting technology allows for the creation of patient-specific implants using CT and MRI scan data. These customized implants ensure uniform pore distribution, which is essential for effective tissue integration.
- AI-driven control systems optimize the printing path and improve print efficiency, reducing production time, material waste, and overall costs. This not only enhances sustainability but also ensures a more accessible and scalable implant solution.

Intelligent Post-Implant Monitoring and Automation
After implantation, smart monitoring systems play a vital role in tracking the performance of biodegradable implants. These systems enable early interventions and tailored adjustments to improve healing outcomes.
1) Ultrasound and MRI-Based Monitoring
Computer vision algorithms are used to analyze imaging data—such as ultrasound and MRI scans—to monitor implant degradation and bone integration with high precision. These tools alert physicians to any delays in tissue fusion or abnormal implant morphology, allowing for timely medical decisions.
2) IoMT and Real-Time Healing Tracking
Next-generation implants are being equipped with micro-sensors that measure localized temperature, pH levels, and internal bone pressure. This real-time data is processed by AI algorithms to build predictive models of healing progress, offering personalized treatment recommendations for each patient.

Personalized Patient-Centered Care
Deep personalization in medical implant design is revolutionizing recovery experiences and treatment outcomes. With the integration of AI in biomaterials, it is now possible to create biodegradable implants tailored to each patient’s unique physiological profile.
1) Comprehensive Patient Data Analysis
- Advanced AI systems collect and process extensive patient data—including age, weight, bone density, and medical history—to generate a precise digital model of the skeletal structure.
- This model becomes the blueprint for designing a custom biodegradable implant that meets specific strength, flexibility, and degradation rate requirements. This high level of personalization reduces the risk of implant rejection and speeds up healing.
2) Continuous Learning and Smart Drug Delivery
- Some innovative biodegradable implants now include embedded drug-releasing molecules—such as bone growth factors or localized pain relievers—that are gradually released as the implant degrades.
- Using deep learning algorithms, AI in biomaterials dynamically adjusts drug release rates based on the patient’s healing stage and biological feedback, creating a more responsive and effective treatment.

Ethical Challenges and Technical Considerations
As AI in biomaterials continues to evolve, the field faces several ethical, technical, and regulatory hurdles that must be addressed to ensure safety, transparency, and trust.
- Data Availability and Diversity: Machine learning models require vast and diverse datasets, but current clinical implant trials are still limited, particularly for rare or complex cases. This data scarcity can hinder the accuracy and generalization of AI predictions.
- Explainability and Trust: Medical professionals demand transparent AI models that clearly explain how decisions are made. Without interpretability, physicians may hesitate to fully adopt AI-driven implant systems.
- Regulatory Approval and Global Standards: Medical device regulations vary from country to country, often leading to extended approval timelines for AI-based implants. Aligning these frameworks is key to accelerating innovation without compromising safety.
The Future of Biodegradable Implants and AI Integration
Looking ahead, the integration of AI in biomaterials is set to expand beyond orthopedic applications, driving innovation across the broader landscape of regenerative medicine.
- Nano-Tech Integration: Future biodegradable implants are expected to incorporate smart nanomaterials like nanoparticles that deliver antibiotics or growth factors in response to cellular signals enhancing healing and infection prevention.
- Smart Self-Diagnostics: Research is also exploring micro-sensors embedded within implants that detect inflammation markers and autonomously trigger alerts or therapeutic adjustments, improving real time care and patient safety.
- Expanding Beyond Bone: The benefits of biodegradable implants will extend to vascular systems, neural tissues, and soft organ reconstruction, unlocking new potential in personalized, less-invasive healthcare solutions.
In the end, in a world rapidly advancing toward digital transformation and medical innovation, biodegradable implants powered by AI in biomaterials represent a breakthrough in precision, performance, and personalization. At HSI Healthcare Simulation and Innovation Center, we’re proud to be at the forefront of this change. Our comprehensive training programs, led by expert professionals and enriched with hands-on learning and specialized consulting, equip you with the tools to lead the future of medical care. Be part of the transformation.
Source: Application of Artificial Intelligence at All Stages of Bone Tissue Engineering