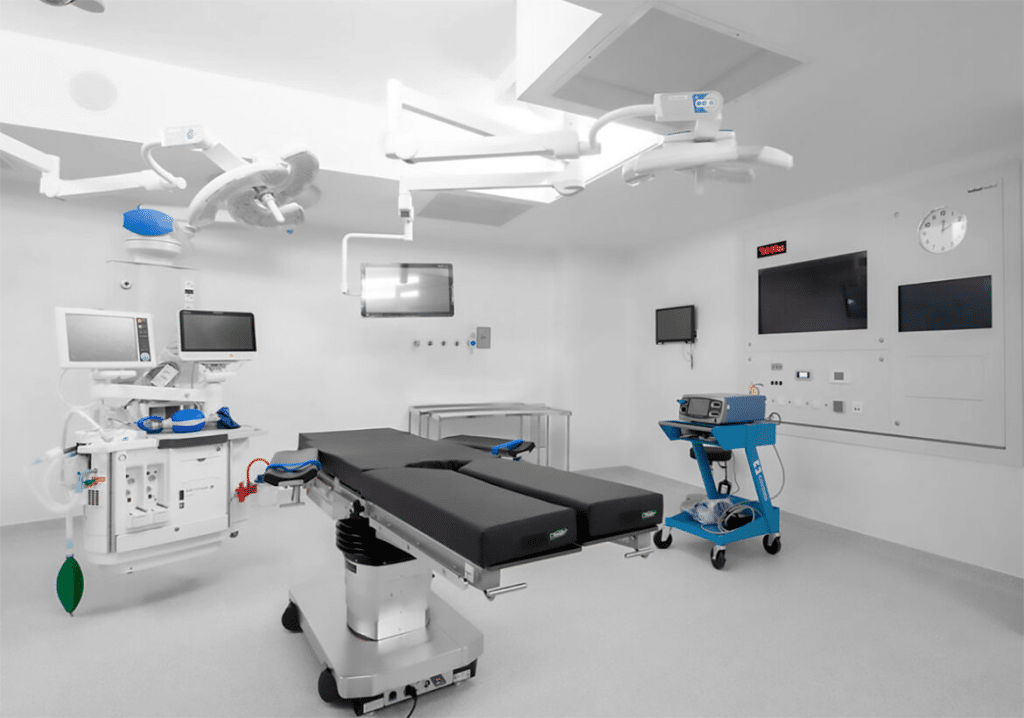
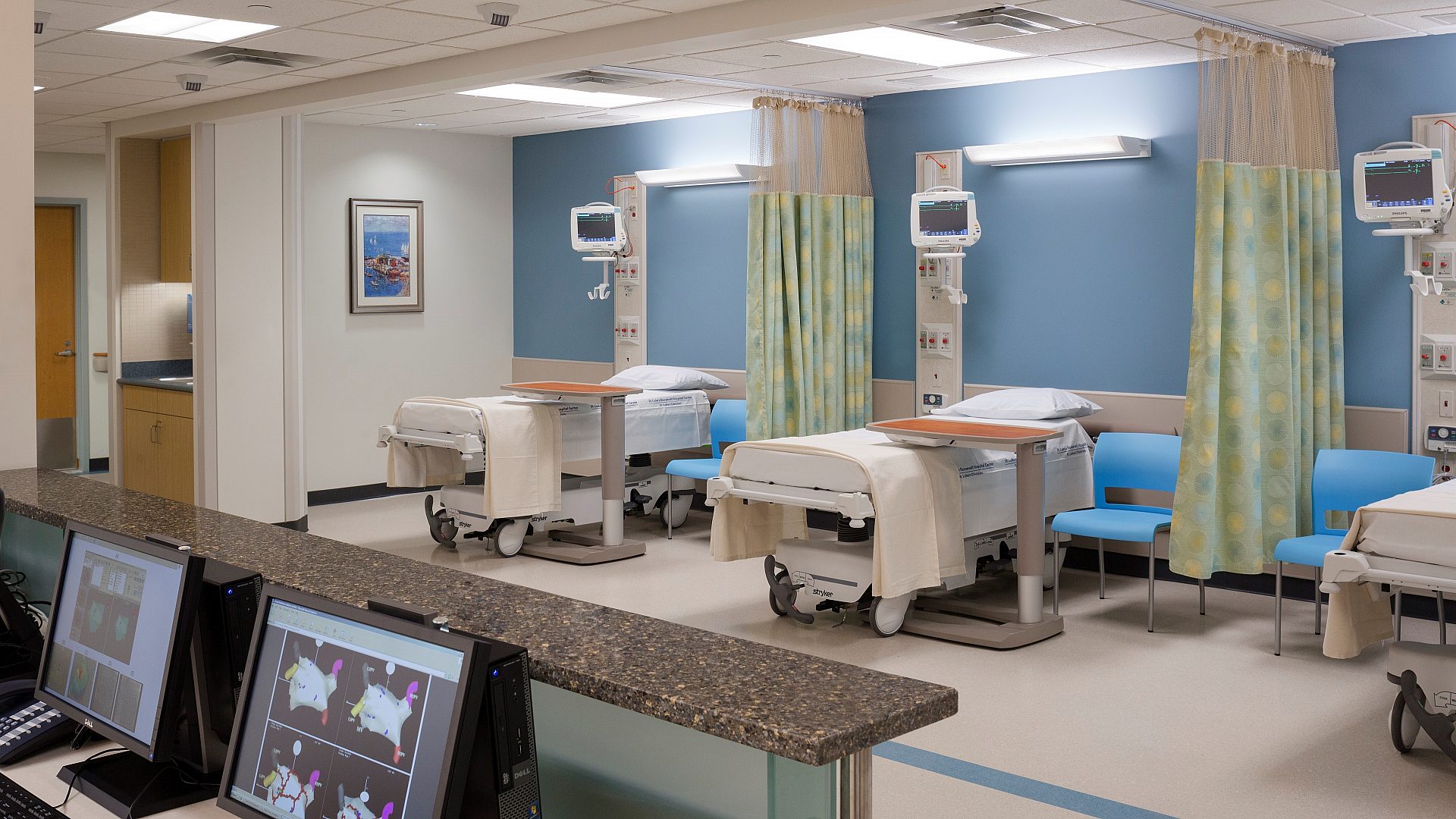
Energy efficiency has always been a persistent challenge in designing healthcare facilities, as hospitals consume up to five times more energy than a luxury hotel. With the catastrophic pressures that the healthcare sector endured in 2020 due to the COVID-19 pandemic that shook the world at that time, healthcare administrators must consider every possible means to achieve economic sustainability. Even if it was not a top priority in the past, designing energy-efficient hospitals has now become a pressing necessity rather than merely an option.
Energy-efficient hospitals play a vital role not only in reducing operating costs but also in protecting the environment and enhancing the comfort of both patients and staff. In this article, we will detail how to design hospitals to transform them into energy-efficient hospitals, relying on the latest studies and research addressing energy efficiency in healthcare facilities, while providing a practical guide for biomedical engineers to apply these principles in design and renovation.
Energy-Efficient Hospitals
The Importance of Energy Efficiency in Hospital Design
Hospitals consume enormous amounts of energy around the clock to operate heating, ventilation, and air conditioning (HVAC) systems, in addition to lighting, medical equipment, and numerous other devices. This excessive energy consumption not only leads to high operating costs but also contributes to increased greenhouse gas emissions, negatively impacting the environment. Therefore, designing energy-efficient hospitals is a critical necessity to achieve both financial and environmental sustainability.

The Role of Biomedical Engineers in the Design Process
Biomedical engineers play a crucial role in designing energy-efficient hospitals. They are responsible for integrating and managing the medical technologies that consume a significant portion of a hospital’s energy. Through their deep understanding of the energy requirements of medical equipment, they can:
Select Energy-Efficient Equipment: Evaluate the energy efficiency of various medical devices and choose those that consume less energy without compromising performance or quality.
Optimize Equipment Usage: Develop protocols and procedures to ensure efficient use of medical equipment, such as turning off devices when not in use and scheduling regular maintenance to maintain optimal performance.
Design Integrated Systems: Collaborate with architects, mechanical, and electrical engineers to integrate medical equipment into the building design in a way that minimizes energy consumption. For example, they can help design efficient cooling and ventilation systems for laboratories and operating rooms.
Monitor and Analyze Energy Consumption: Utilize energy management systems to monitor and analyze the energy consumption of medical equipment and identify areas for improvement.

Strategies for Designing Energy-Efficient Hospitals
Biomedical engineers and designers hold a pivotal role in radically transforming energy consumption in hospitals by adopting a variety of innovative strategies. Among these strategies, improving HVAC systems stands out, as they are one of the largest energy consumers in healthcare facilities. This can be achieved by using high-efficiency HVAC systems and implementing heat recovery systems that recycle wasted energy, in addition to activating demand-controlled ventilation to ensure that unoccupied spaces are not unnecessarily ventilated. Furthermore, enhancing the design of air ducts and using high-quality insulation materials to reduce energy loss are also key factors.
In addition to HVAC systems, lighting represents another critical element that can be developed to reduce energy consumption. This is primarily achieved by replacing traditional bulbs with LED lights, which are known for their high efficiency and long lifespan. Maximizing the use of natural light through smart architectural design plays a significant role in reducing reliance on artificial lighting during daylight hours. Moreover, installing motion sensors and lighting control devices ensures that lights are turned off in unoccupied areas, effectively contributing to energy conservation.
Efforts to save energy do not stop at the basic building systems; they also extend to the medical equipment itself. It is crucial to acquire high-energy-efficiency medical devices and establish regular maintenance programs to ensure they operate at maximum capacity while consuming the least amount of energy. Additionally, implementing clear protocols to turn off equipment when it is not needed is a simple yet effective step in reducing overall energy consumption.
Looking further ahead, embracing sustainable design principles for buildings—including the use of insulated building materials, energy-efficient windows, designs that maximize natural light, the integration of renewable energy sources such as solar panels and geothermal energy, and the implementation of smart energy management systems to monitor and analyze consumption—are all integrated steps toward achieving hospitals that use energy more efficiently and are sustainable in the long term.
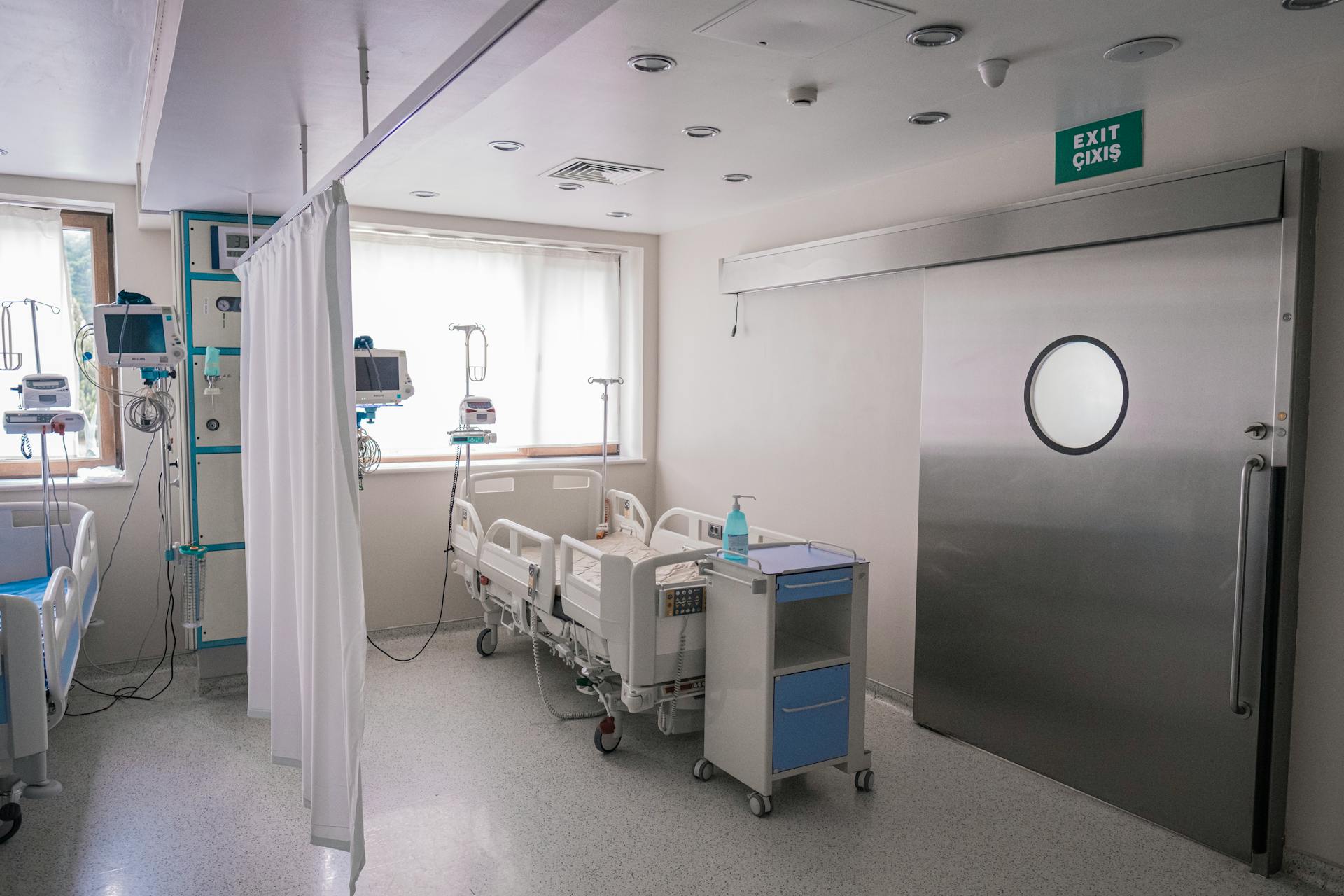
Practical Steps for Designing Energy-Efficient Hospitals
There are several crucial steps to take when starting a project to design or renovate hospitals with energy savings in mind:
1- Assess the Current Situation:
Before beginning any renovation or new design project, engineers should conduct a comprehensive assessment of the hospital’s current infrastructure. This includes reviewing heating and cooling systems, thermal insulation, lighting, and electrical equipment. This assessment is the first step toward identifying weaknesses and strengths that can be improved to achieve better efficiency.
2- Apply Dynamic Energy Modeling:
Using simulation software and dynamic energy modeling can help visualize multiple scenarios for energy saving. By studying the effects of different modifications, designers can choose the best solutions that achieve energy savings without compromising patient comfort or operational efficiency.
3- Adopt Machine Learning Techniques:
Employing machine learning models is an innovative step to predict and analyze energy consumption. These models can identify patterns and the most influential factors, allowing adjustments to systems based on different operating conditions and achieving enhanced energy performance. This approach represents the future of designing energy-efficient hospitals, as models can be regularly updated with changing environmental and operational conditions.
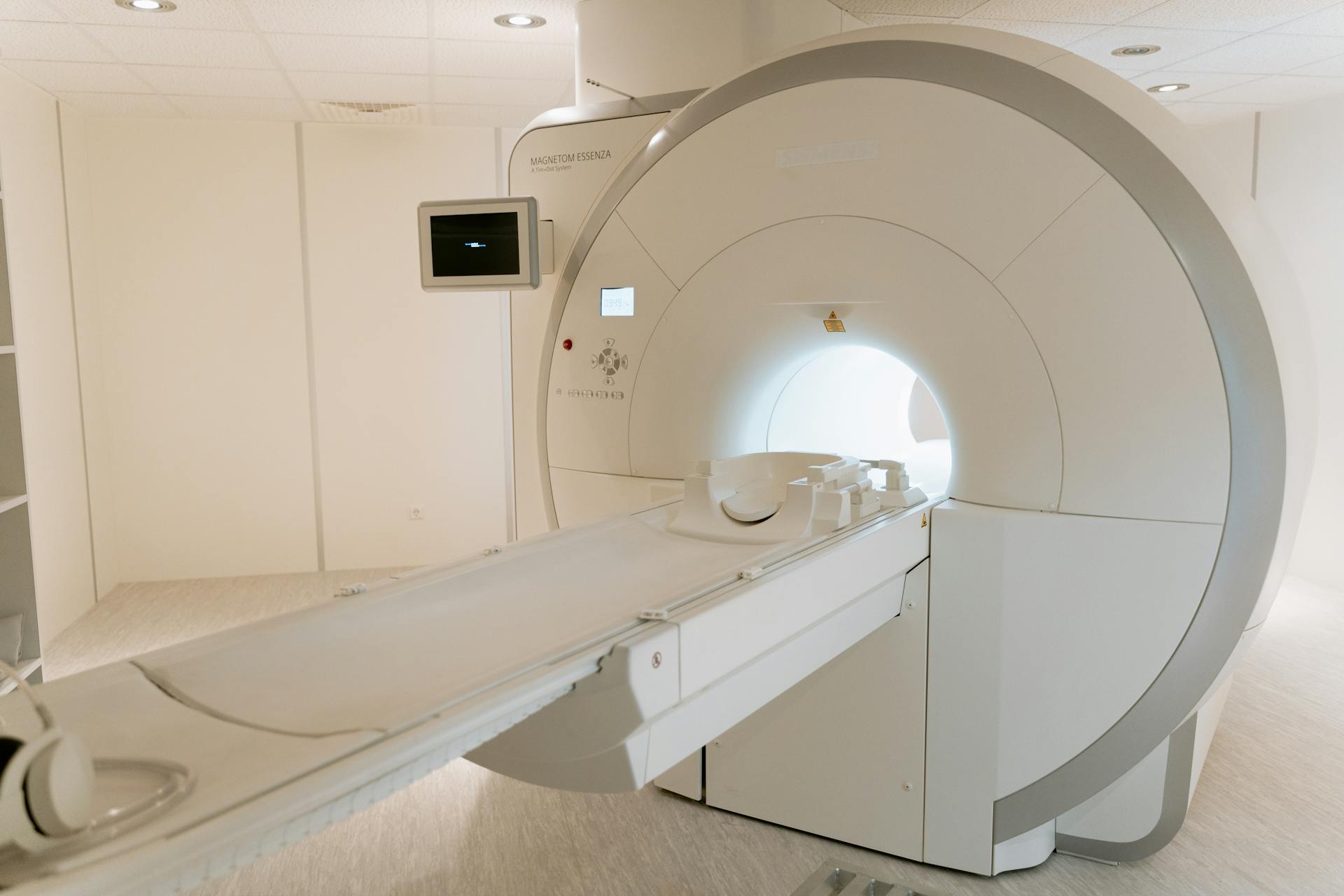
4- Improve Insulation and Windows:
As many studies have shown, improving glazing and window technologies plays a central role in designing energy-efficient hospitals. Adopting double-glazed windows and choosing types of glass that reduce thermal loss allow the hospital to benefit from natural light without adversely affecting the heating and cooling systems.
5- Use Advanced Lighting and Electrical Systems:
Implementing modern lighting technologies, such as LED lighting, is one of the effective means of reducing energy consumption. Additionally, integrating smart control systems that adjust lighting and air conditioning levels according to the building’s needs and different times of the day can further optimize energy use.
Designing energy-efficient hospitals requires a comprehensive approach that combines innovative architectural design, advanced technology, and effective energy management. Biomedical engineers play a pivotal role in this effort by ensuring the efficient integration and use of medical equipment. By adopting sustainable design strategies and best practices, we can create hospitals that not only reduce energy consumption and operating costs but also enhance patient comfort and safety, contributing to a more sustainable future. If you want to elevate your status as a biomedical engineer to reach a high level, all you need to do is contact us through the HSI website and explore our services and training courses.