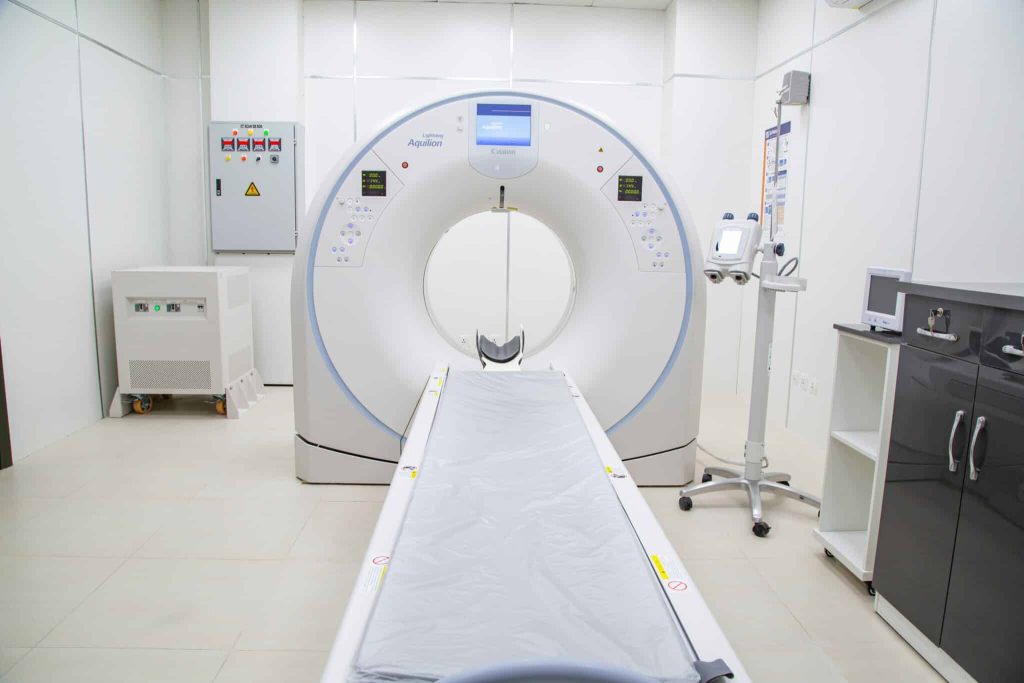
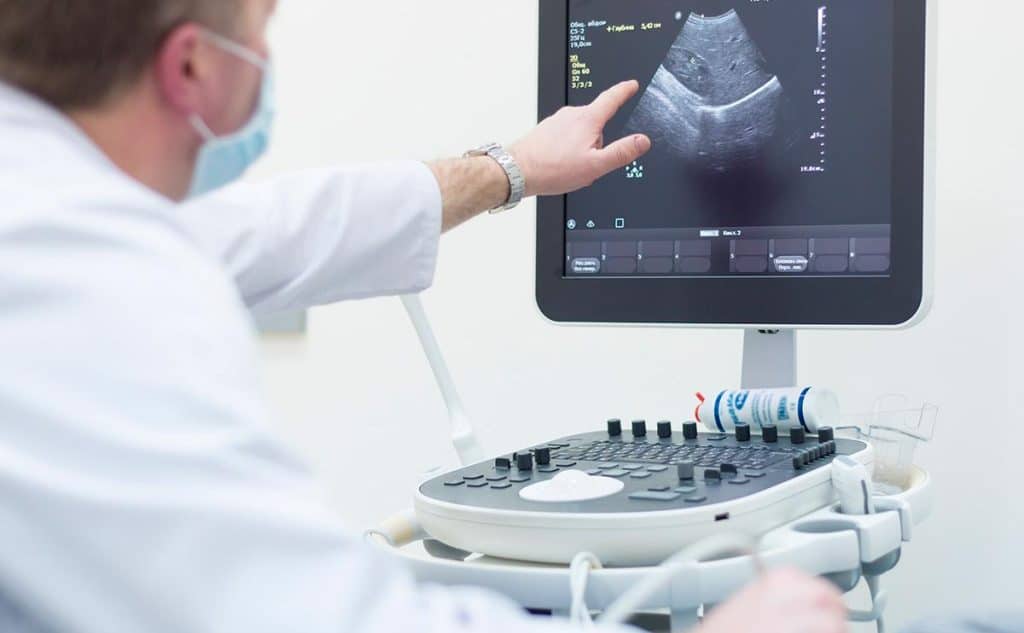
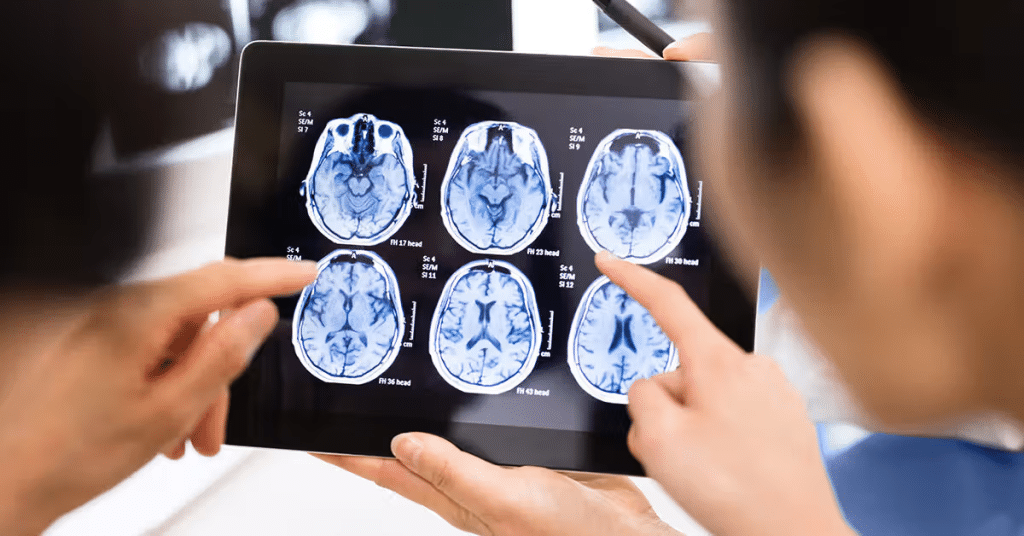
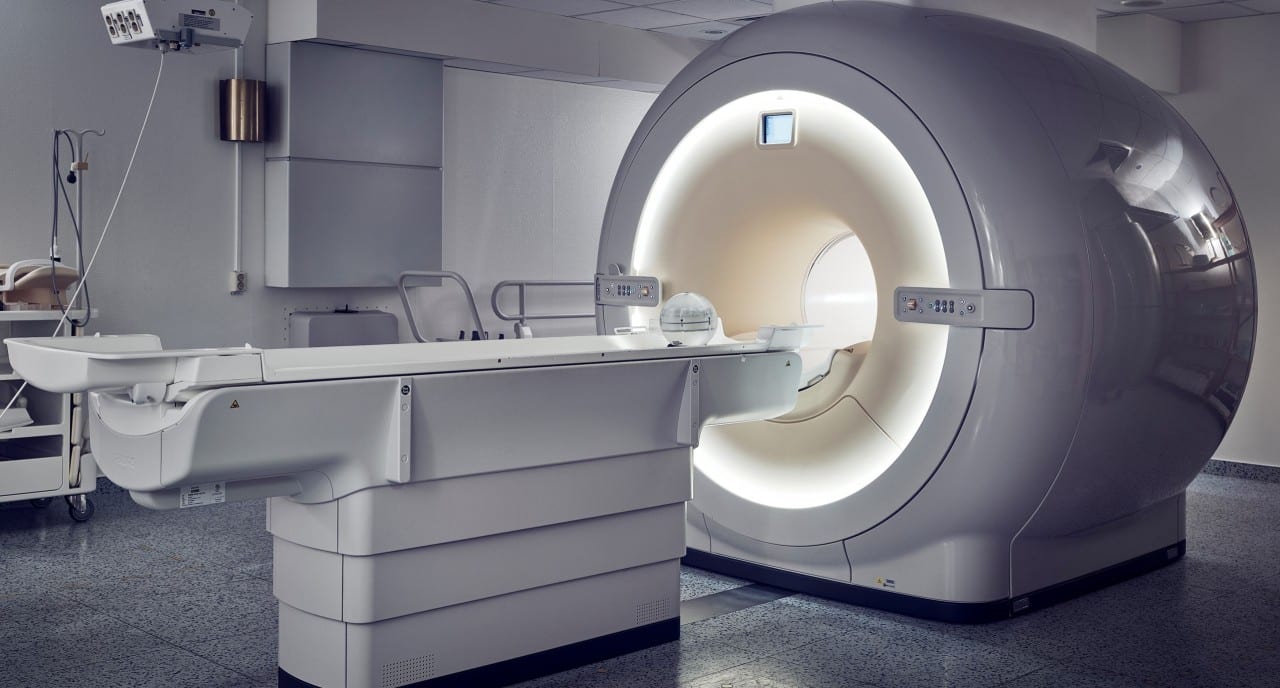
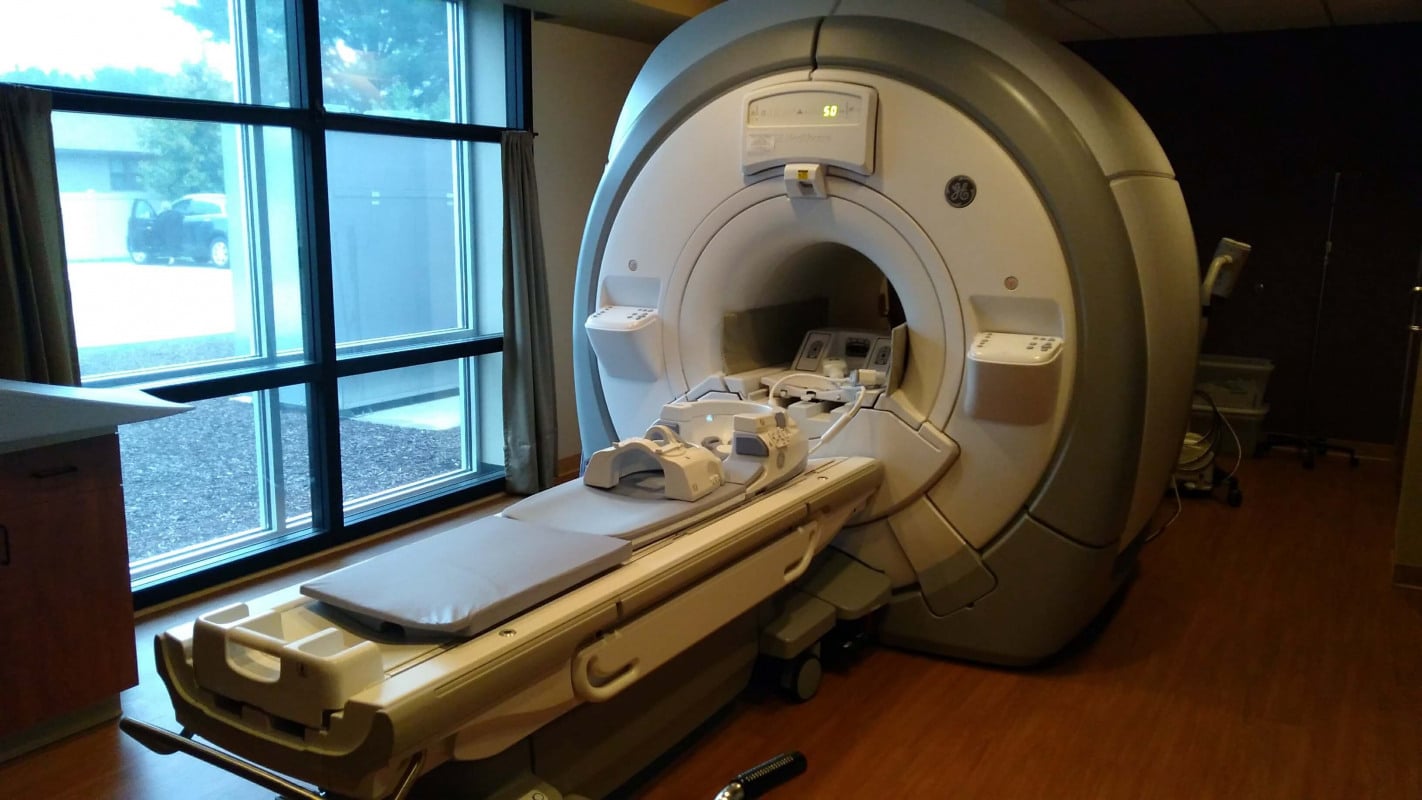
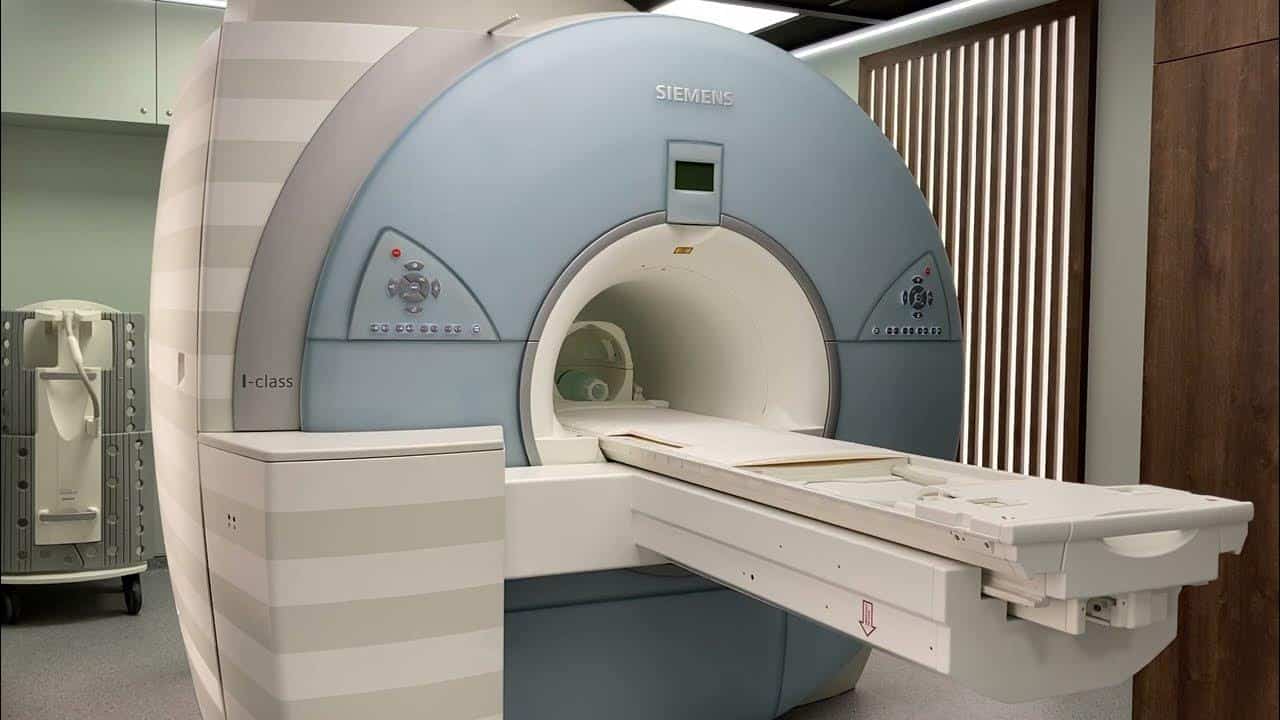
Amid the rapid technological advances in the fields of medicine and biomedical engineering, hybrid imaging has emerged as a revolutionary technique that has transformed the concepts of medical diagnosis like never before. This approach relies on combining multiple imaging modalities such as magnetic resonance imaging (MRI), computed tomography (CT), and nuclear medical imaging, which enables the acquisition of precise and comprehensive images of a pathological condition. Moreover, recent developments in artificial intelligence have contributed to analyzing these images with exceptional precision and speed, making this technology the ideal choice for early diagnosis.
The Remarkable Features of Hybrid Imaging Technology
Hybrid imaging is considered an innovative technique that combines the advantages of each imaging modality to provide both quantitative and qualitative information that assists physicians in accurately evaluating a patient’s condition. This technology is used in the detection of tumors, chronic diseases, and functional disorders of vital organs. In addition, the integration of different techniques delivers detailed anatomical and functional data, while artificial intelligence enhances the process of analyzing and interpreting this data in a scientifically reliable manner.
The Importance of Hybrid Imaging in Medical Diagnosis
Hybrid imaging plays a vital role in the early and accurate diagnosis of numerous diseases, especially cancerous tumors and cardiovascular and neurological disorders. It provides valuable information that helps doctors in:
- Detecting cancerous tumors at early stages: Hybrid imaging can identify small tumors that are difficult to detect using conventional imaging techniques.
- Determining the extent of cancer spread: It helps in assessing whether the cancer has metastasized to other organs in the body.
- Evaluating tumor response to treatment: Hybrid imaging can be used to monitor the effectiveness of treatments and determine whether a tumor is responding to therapy.
- Diagnosing heart diseases: It aids in assessing cardiac functions and identifying areas with insufficient blood supply.
- Diagnosing neurological diseases: This technology can be used in the diagnosis of conditions
- such as Alzheimer’s, Parkinson’s, and multiple sclerosis.
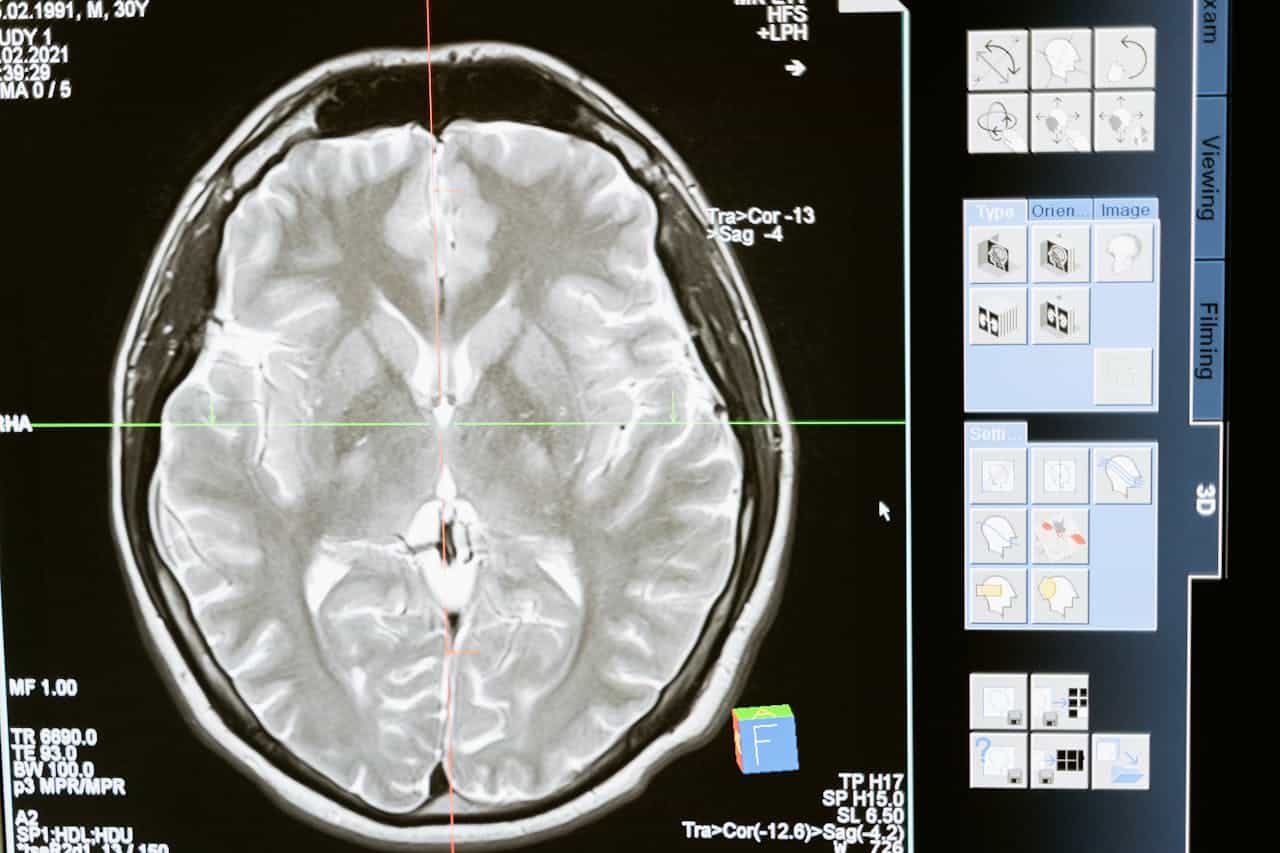
Recent Developments in Imaging Techniques and Artificial Intelligence
With continuous technological progress, hybrid imaging techniques have seen significant advancements in recent years. Modern innovations have enhanced the quality of final images and reduced the time required to obtain results, which has led to an overall improvement in healthcare quality. Artificial intelligence techniques are utilized to process and analyze data in innovative ways, where algorithms are trained on massive datasets of medical images to deliver precise and immediate diagnoses. These applications serve as strong support for traditional techniques and contribute to building an integrated diagnostic system.
The Role of Artificial Intelligence in Enhancing Medical Diagnosis
Artificial intelligence is one of the fundamental pillars in the development of hybrid imaging techniques, relying on advanced algorithms to analyze images and detect fine details that are difficult to observe with the naked eye. These algorithms help in precisely determining the characteristics of tumors and tissues and assist in predicting the stages of disease progression more rapidly. By integrating artificial intelligence with hybrid imaging, physicians can achieve early and effective diagnosis, which contributes to improved treatment outcomes and a reduction in potential complications.
Modern hybrid imaging technologies are vital tools for the early and effective detection of diseases, as they enable doctors to obtain comprehensive data about the patient’s condition. This approach facilitates precise and prompt therapeutic decision-making, thereby enhancing the chances of treatment success. Artificial intelligence plays a pivotal role in analyzing this data and extracting critical biomarkers that may be overlooked by conventional methods, which in turn increases the accuracy and reliability of diagnostic results.
Challenges and Future Development Prospects
Despite the significant achievements of hybrid imaging in the field of medical diagnosis, challenges still remain for researchers and clinicians in the optimal application of this technology. Among these challenges is the need to develop more advanced artificial intelligence algorithms and to provide extensive training datasets to improve diagnostic performance. Moreover, the integration of various imaging techniques represents a complex task that requires high-level coordination between devices and software. Artificial intelligence remains at the forefront of efforts to address these challenges and to achieve promising future developments in medical diagnosis.
A Future Vision for Hybrid Imaging in Medicine
The future of medicine is moving towards an increased reliance on digital technologies and artificial intelligence, opening up new horizons in the field of hybrid imaging. Artificial intelligence is considered a cornerstone for developing diagnostic methods and analyzing data much faster than before, enabling physicians to offer advanced and personalized treatment services to each patient for quicker and better recovery. These technologies contribute to improving survival rates and reducing healthcare costs, while also providing valuable data that supports well-informed therapeutic decisions. Hybrid imaging, assisted by artificial intelligence, shows tremendous potential in enhancing healthcare quality and elevating the standards of medical diagnosis.

Hybrid imaging represents a true revolution in the field of medical diagnosis, thanks to the integration of various imaging techniques and the rapid advancement of artificial intelligence. These technologies provide precise and comprehensive insights that aid in the early detection of diseases and in determining the most appropriate treatment pathways for each case. The synergy between advanced imaging techniques and artificial intelligence holds great promise for improving healthcare quality and achieving outstanding therapeutic outcomes, making this technology one of the most important future tools in medicine. Continuous research and development in artificial intelligence and hybrid imaging remain the key to achieving further breakthroughs and innovations in the world of medical diagnostics.
In conclusion, after exploring hybrid imaging technologies and in light of the rapid advancements in medical imaging and artificial intelligence, if you aspire to become a part of the biomedical engineering field, connect with HSI Center. Through our specialized training and consulting programs, we empower students and professionals to gain both practical and scientific skills, enabling them to keep pace with the latest innovations and actively contribute to improving the quality of healthcare.
Source: Hybrid imaging is the future of molecular imaging – PMC