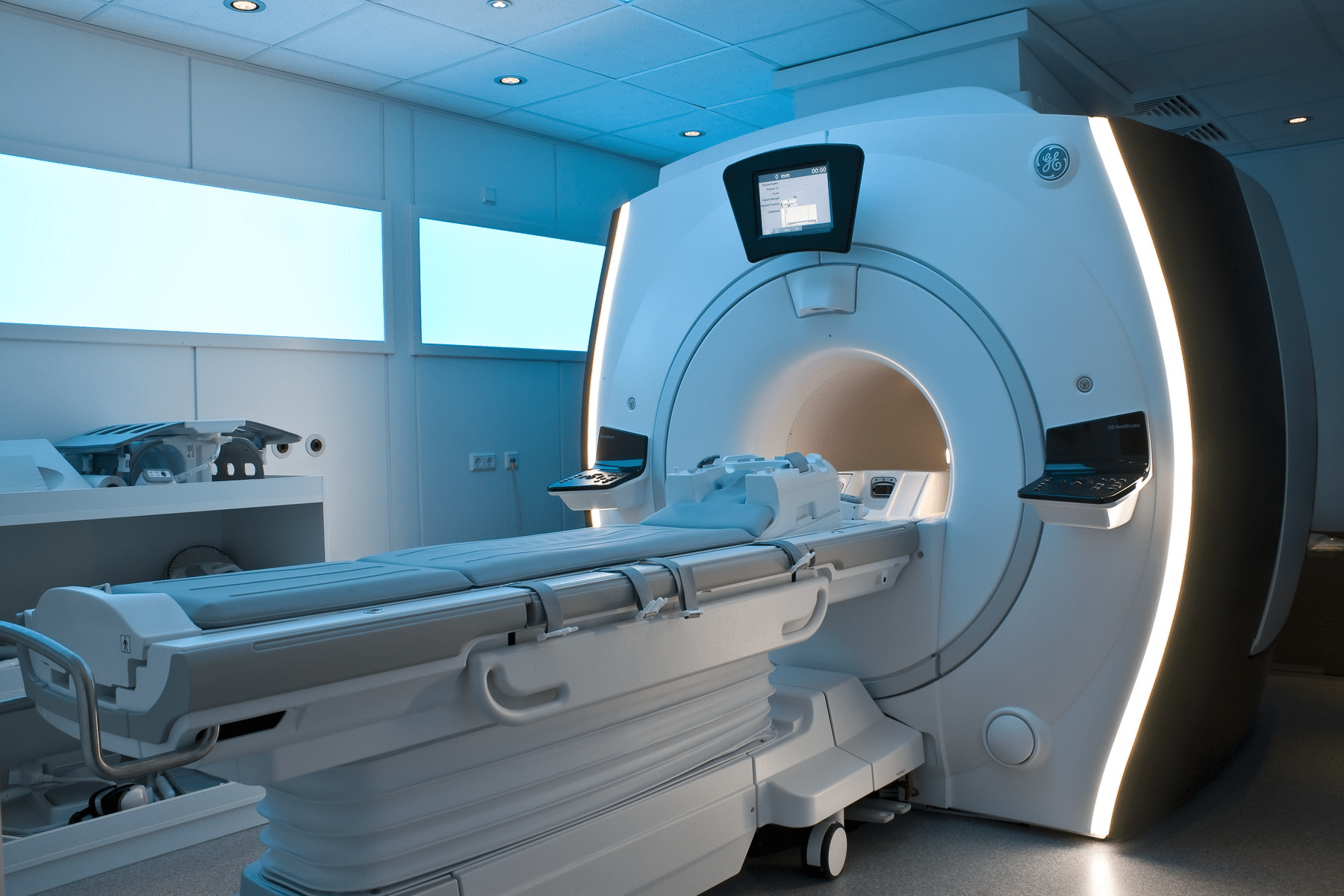
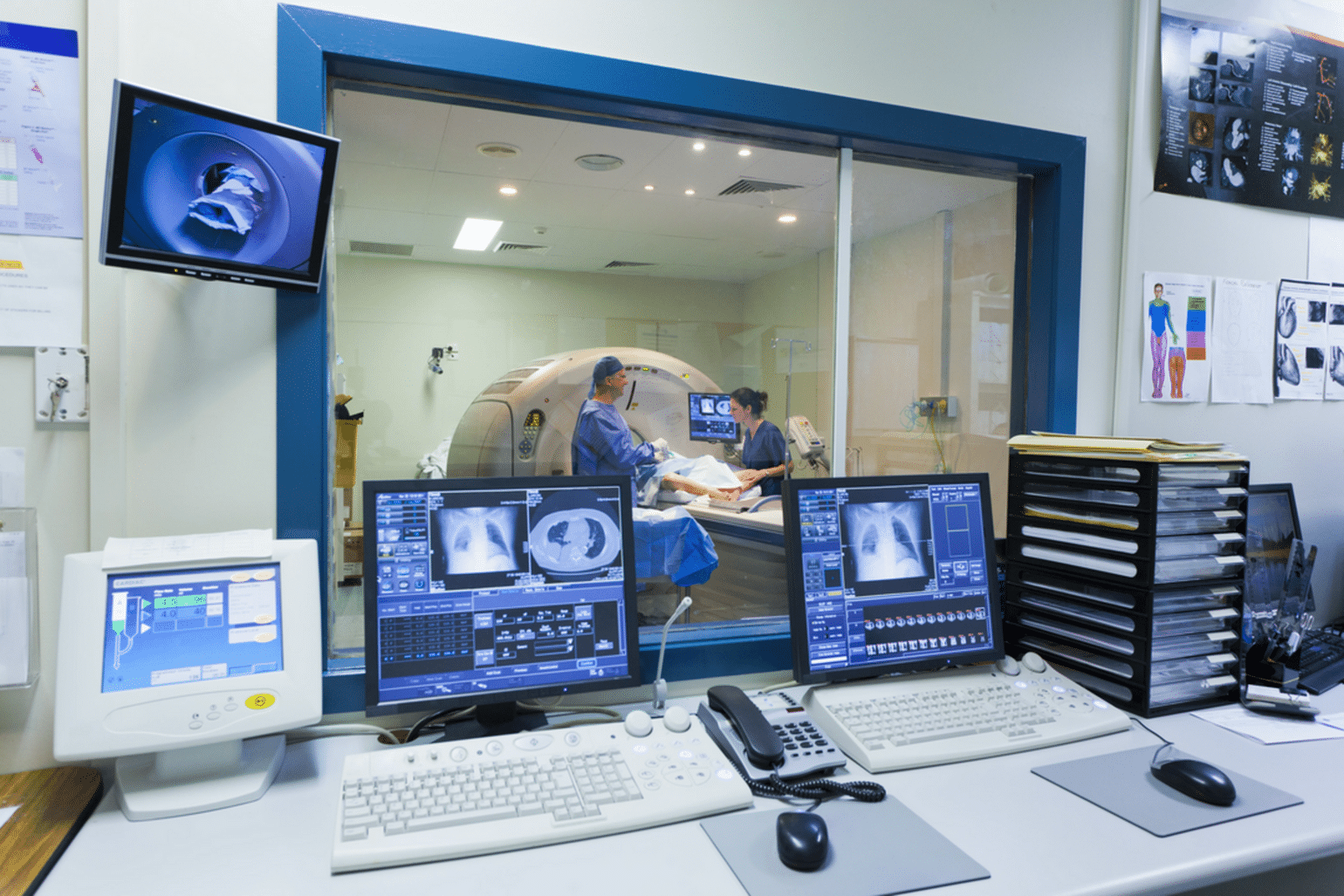
The healthcare industry is undergoing a transformative shift, thanks to AI in medical imaging, which has become a crucial tool for improving diagnostic accuracy and accelerating treatment processes. With rapid technological advancements, AI is no longer just an assistive tool but a strategic partner in medical imaging—particularly in MRI and ultrasound. This guide provides a comprehensive introduction for beginners, highlighting how AI in medical imaging is applied in MRI and ultrasound.
The Integration of AI in Medical Imaging Technologies
AI in medical imaging is one of the most significant innovations enhancing disease diagnosis methods. Through machine learning and deep learning techniques, AI-powered systems can analyze medical images with remarkable precision. This capability enables early disease detection and the development of effective treatment plans. AI’s role extends beyond expediting diagnosis—it enhances overall healthcare quality, minimizes human error, and alleviates the workload on medical professionals.

Specifically, AI plays a vital role in MRI and ultrasound imaging, improving image quality and reducing scan time, ultimately enhancing patient comfort and lowering healthcare costs. AI in medical imaging refers to the use of machine learning and deep learning algorithms to analyze and interpret medical images. These technologies include:
- Machine Learning – Teaching systems to recognize patterns and differences in medical images.
- Deep Learning – Utilizing neural networks to analyze images at multiple levels, enabling accurate insights.
- Computer Vision – Applying AI techniques to digital images for detecting fine details that may be difficult for the human eye to perceive.
By implementing these technologies, AI-driven systems can identify diseases, monitor patient progress, and provide highly accurate diagnostic recommendations. AI in medical imaging represents a revolutionary advancement in medical diagnostics, combining human expertise with computational intelligence to achieve unprecedented levels of accuracy and efficiency.
AI in medical imaging and its application in MRI
AI in medical imaging is revolutionizing MRI and ultrasound diagnostics by enhancing image analysis and improving disease detection accuracy at an unprecedented speed. This article explores the significance of MRI in medical diagnostics and how AI is optimizing this advanced imaging technology.
MRI in Medical Diagnostics
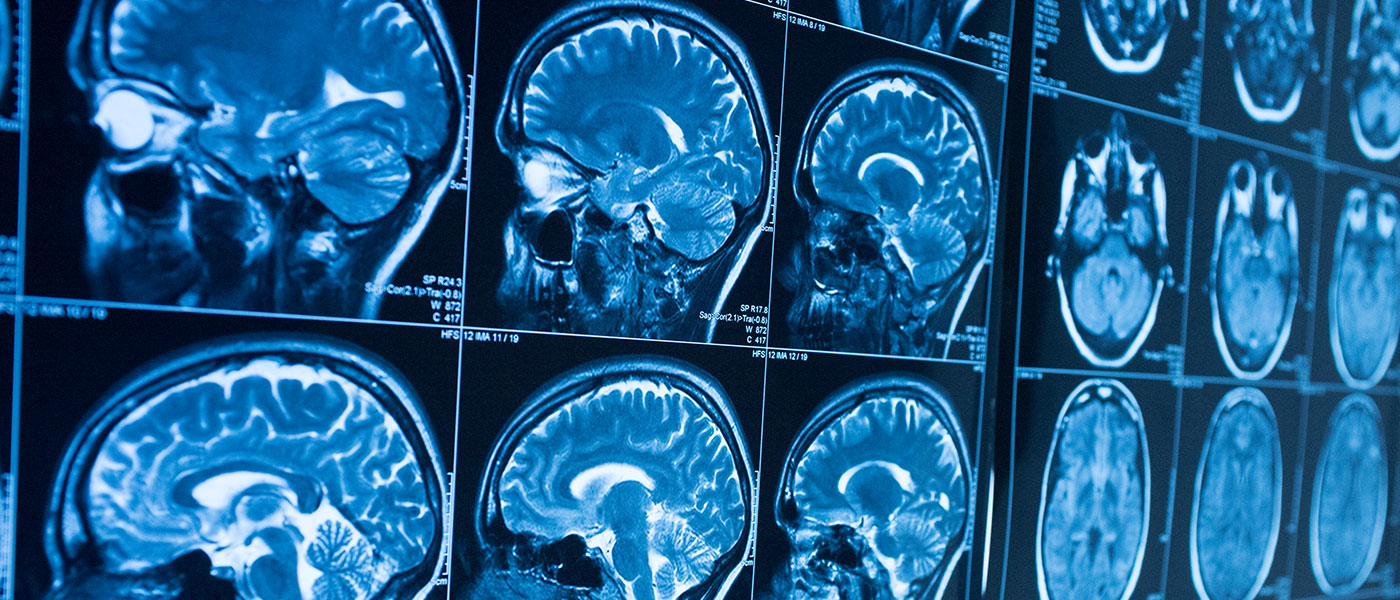
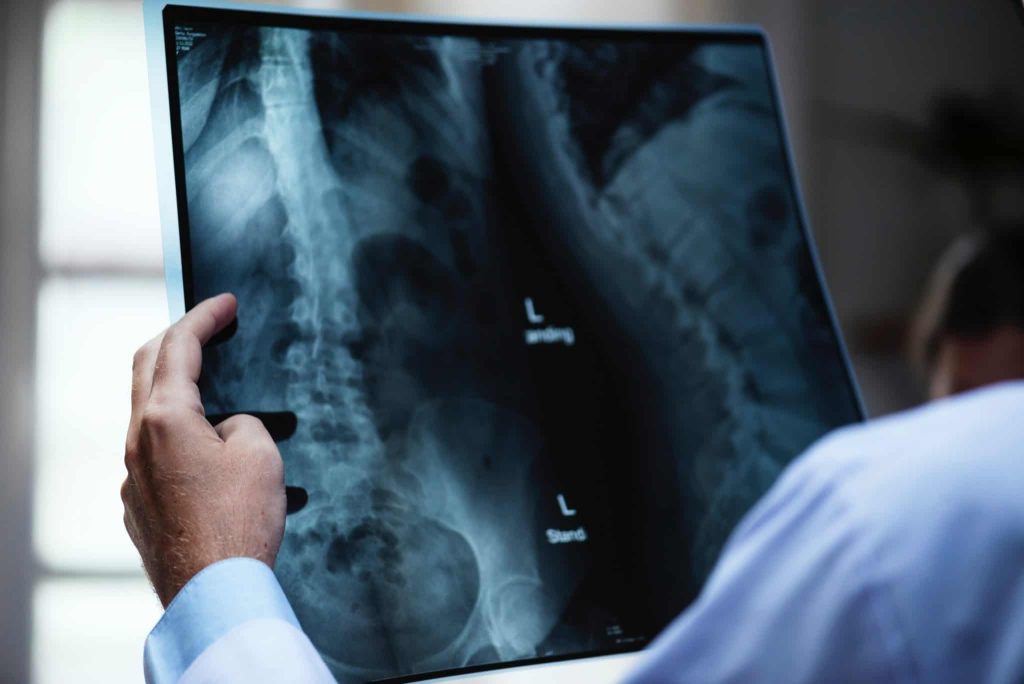
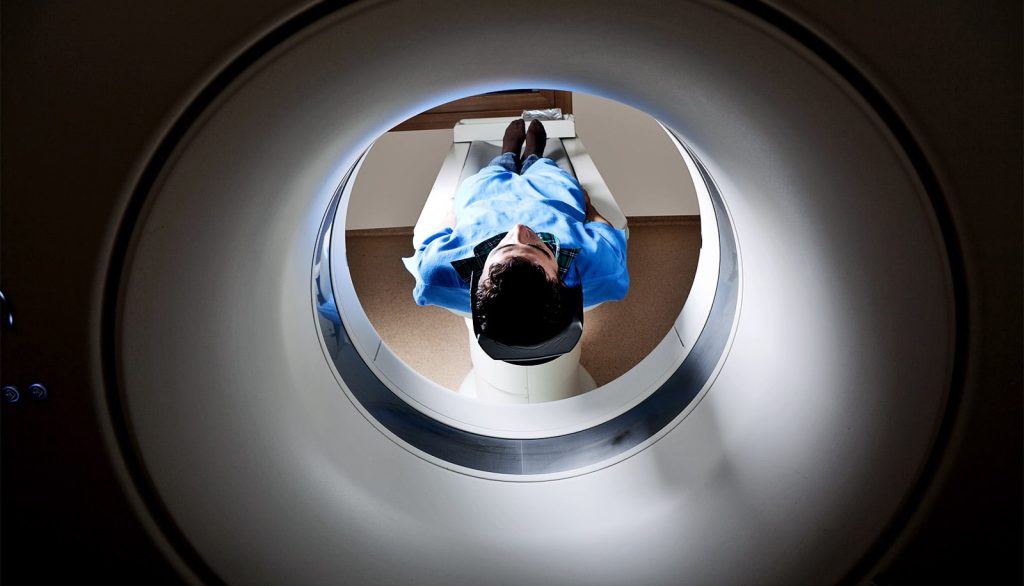
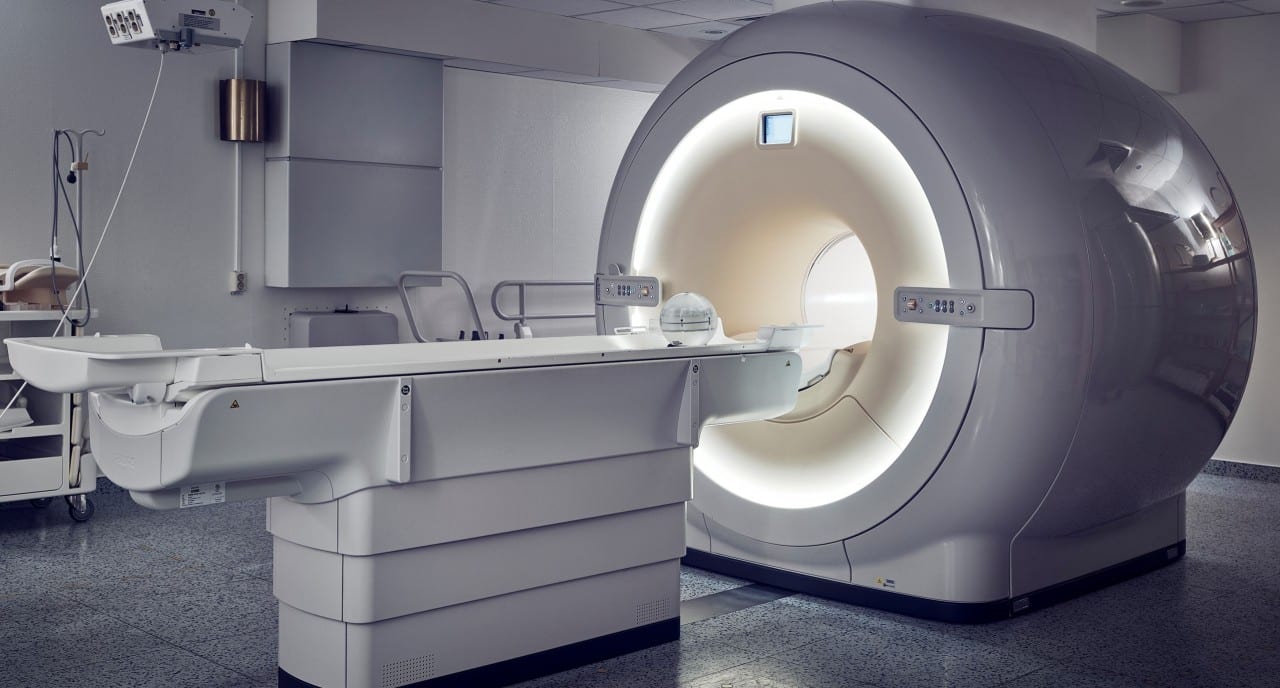
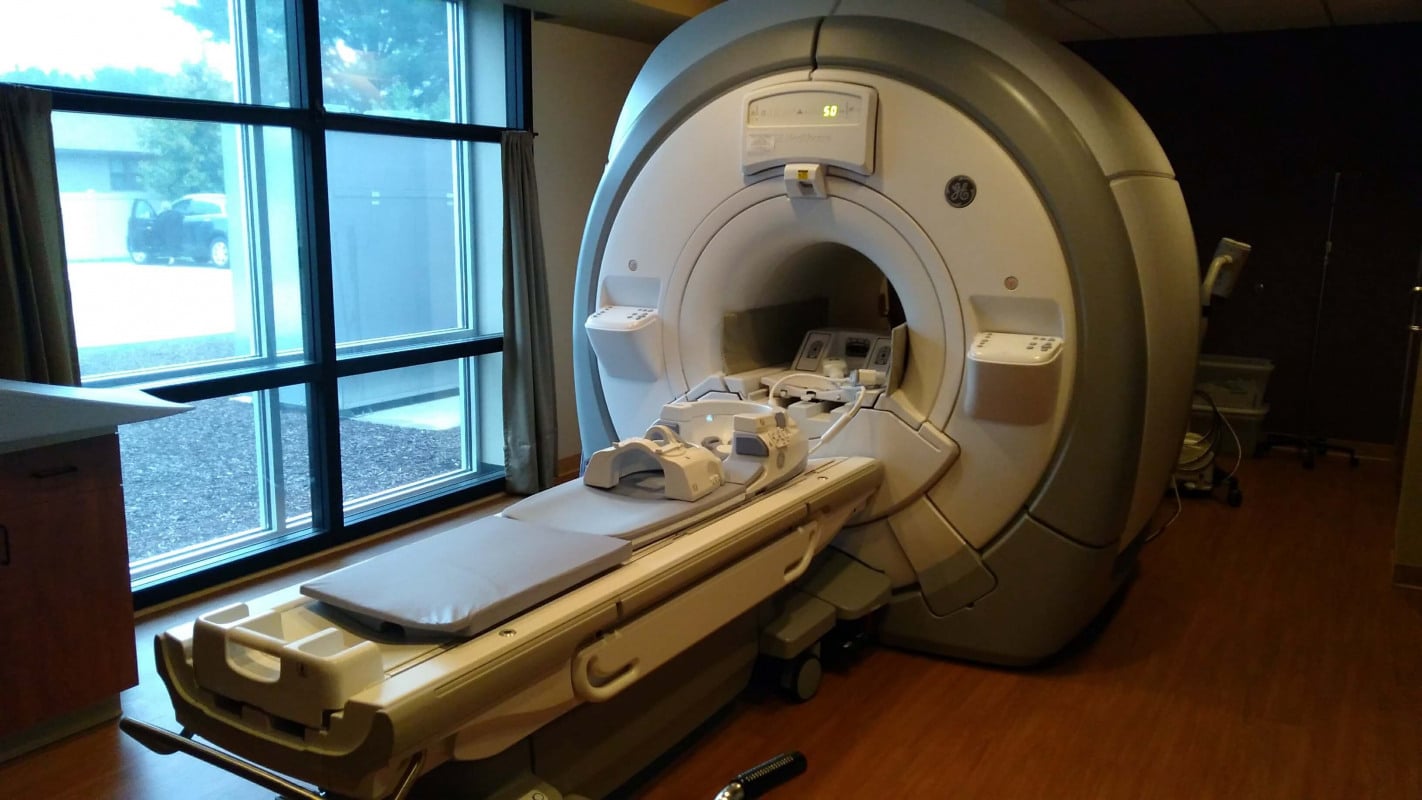
MRI (Magnetic Resonance Imaging) is a non-invasive imaging technique used to obtain detailed images of organs and tissues within the body. It relies on powerful magnetic fields and radio waves to generate high-resolution images that reveal subtle changes in biological structures. MRI plays a critical role in detecting neurological disorders, tumors, and internal injuries, making it an indispensable tool in modern medicine.
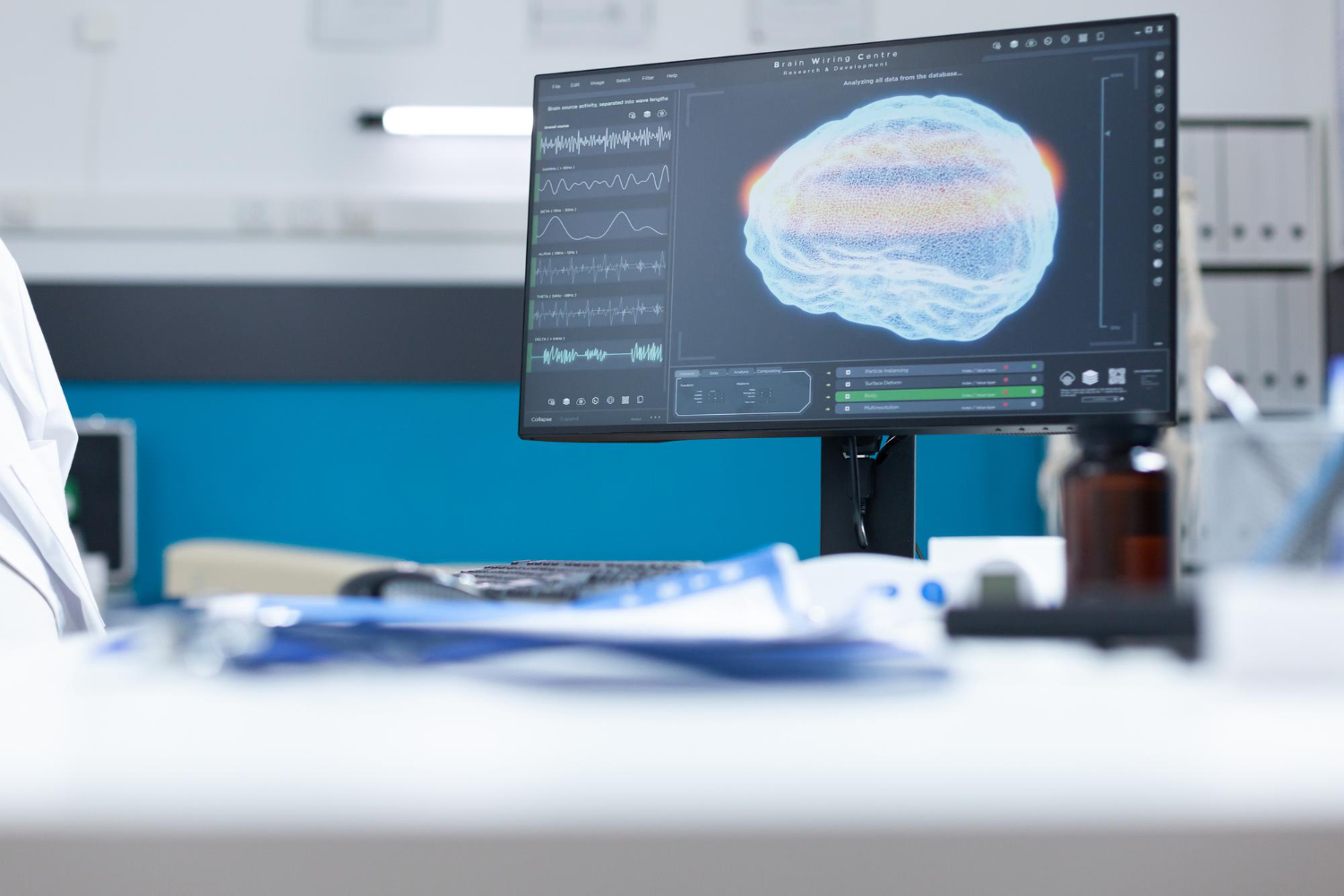
You can check out: Understanding MRI | Principles and Applications
How AI Enhances MRI Imaging
AI in medical imaging significantly improves MRI efficiency through various innovative approaches, including:
- Reducing Scan Time: AI-driven algorithms optimize image reconstruction, cutting scan times by up to 50%.
- Enhancing Image Quality: Deep learning techniques reduce noise and refine image clarity, enabling more accurate diagnoses.
- Early Disease Detection: AI-powered systems analyze MRI scans with high precision, identifying subtle abnormalities indicative of conditions such as tumors and multiple sclerosis.
- Big Data Analysis: AI rapidly processes vast amounts of imaging data, extracting critical diagnostic insights and generating detailed reports.
Through these advancements, AI in medical imaging has become an essential partner in diagnostics, refining MRI quality and boosting early disease detection rates. This transformation in medical imaging improves healthcare efficiency and enhances patient outcomes.
AI in medical imaging and its application in Ultrasound Diagnostics
AI is also revolutionizing ultrasound imaging, refining examination quality, and improving diagnostic precision. The following sections explore the significance of ultrasound in medicine and how AI enhances this widely used imaging technique.
The Importance of Ultrasound in Medicine
Ultrasound is a fundamental diagnostic tool, particularly in obstetrics, gynecology, and internal organ assessment. This imaging method is safe, non-invasive, and uses high-frequency sound waves to produce real-time images of tissues and organs, making it an invaluable tool for monitoring fetal development and diagnosing various medical conditions.

AI Applications in Ultrasound Imaging
AI in medical imaging enhances ultrasound accuracy through:
- Automated Image Analysis: AI algorithms analyze ultrasound images with high precision, reducing operator dependency and minimizing diagnostic errors.
- Anomaly Detection: Machine learning models identify abnormalities, such as fetal deformities and potential tumors, improving early diagnosis rates.
- Guidance in Surgical Procedures: AI assists doctors during interventional procedures, increasing surgical precision and minimizing risks.
- Real-Time Data Processing: AI-driven ultrasound systems analyze images instantly, expediting medical decision-making and treatment planning.
By integrating AI, ultrasound imaging becomes more efficient and accurate, providing high-quality diagnostic images that facilitate early disease detection and improve patient care.
You can also get acquainted with: What are The Basics of Ultrasound Technology?
The Multifaceted Benefits of AI in Medical Imaging
- AI-powered medical imaging systems analyze vast amounts of data with exceptional precision. These smart technologies can detect subtle abnormalities in images that may be overlooked by the human eye, significantly improving the early diagnosis of conditions such as tumors and multiple sclerosis.
- One of the major advantages of AI in medical imaging is the ability to expedite scanning procedures. By utilizing advanced algorithms, AI reduces scan times and enhances image reconstruction, allowing doctors to provide quicker diagnoses and shorten patient wait times.
- Deep learning techniques optimize image clarity by reducing noise and enhancing detail visibility. This improvement results in highly accurate medical images, which are crucial for precise diagnoses and effective treatment planning.
- AI-driven imaging systems generate detailed analytical reports and automatically identify disease indicators, minimizing human errors. By supporting physicians with data-backed insights, AI helps reduce the likelihood of misdiagnosis and enhances overall medical decision-making.
- Support for Medical Decision-Making: With its advanced analytical capabilities, AI provides detailed diagnostic data that aids in making swift and accurate treatment decisions. Doctors can rely on AI-generated insights to tailor treatment plans based on each patient’s unique condition.

AI in MRI Imaging
Several research initiatives and practical applications have begun incorporating AI in medical imaging to enhance MRI efficiency. Notable examples include:
- FastMRI Project: A collaboration between academic institutions and tech companies aimed at reducing scan time while improving image quality, making MRI scans more comfortable for patients.
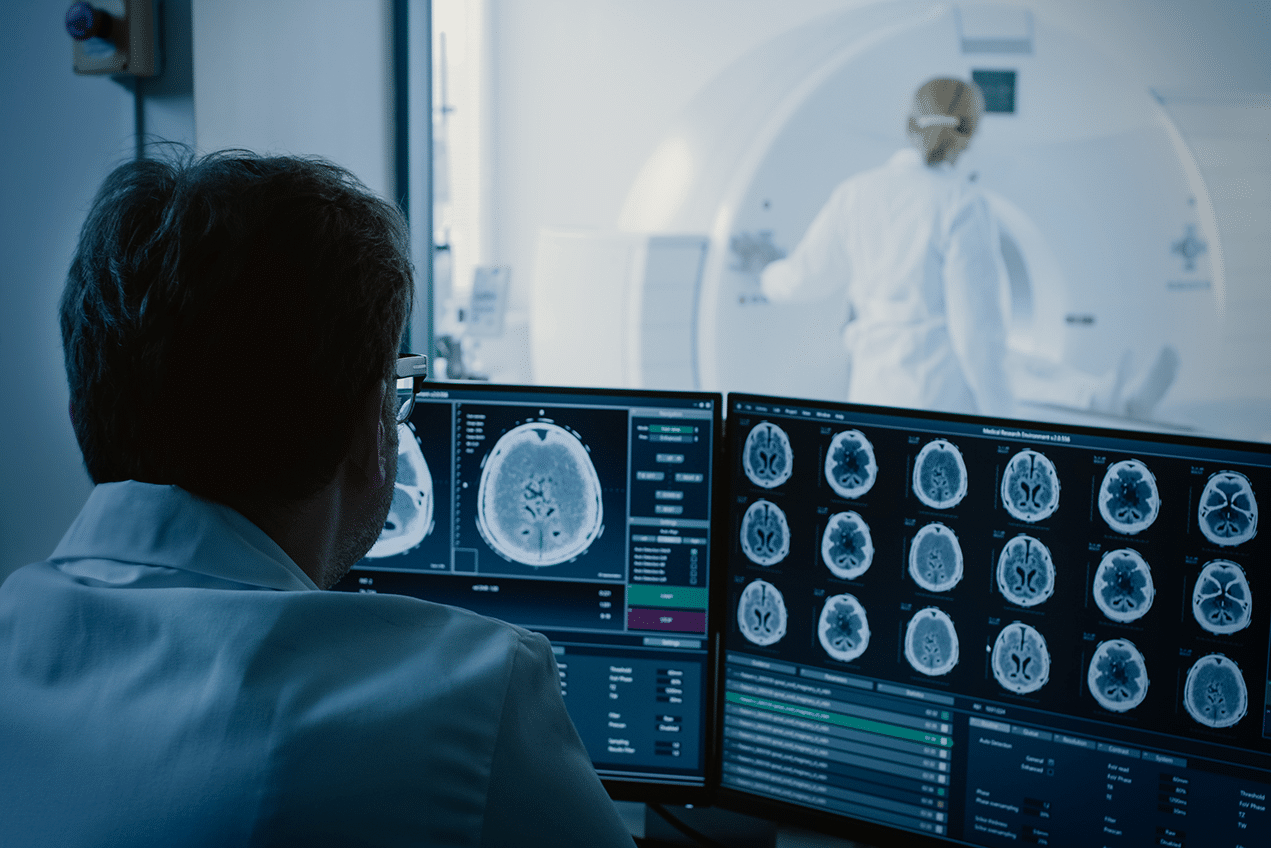
- Neural Image Analysis Systems: These AI-powered tools assist in the early detection of neurological disorders such as multiple sclerosis and brain tumors, offering faster and more precise diagnoses through deep learning algorithms.
AI in Ultrasound Imaging
AI is also making strides in ultrasound imaging, improving the accuracy and efficiency of diagnostic procedures:
- Real-Time Image Analysis: AI-powered systems analyze ultrasound images instantly, enabling doctors to make immediate clinical decisions during examinations.
- Smart Guidance Systems: These AI-driven technologies assist physicians during interventional procedures, enhancing surgical precision and minimizing risks.
- Early Diagnosis in Obstetrics and Gynecology: AI plays a vital role in detecting fetal abnormalities and congenital defects at an early stage, allowing timely medical interventions.
Ultimately, with the rapid advancements in artificial intelligence technologies in medical imaging, it has become essential for professionals in biomedical engineering to keep up with these transformations and seize the opportunities they offer. For this reason, HSI Center provides specialized training programs that equip industry professionals with the knowledge and skills needed to apply the latest technologies, including AI, contributing to skill development and enhancing professional excellence. Get in touch with us today and discover how HSI can be your ideal partner in your career journey.
Source: Revolutionizing Radiology with Artificial Intelligence