The field of medical technology is witnessing continuous and rapid advancements, with new and improved equipment being introduced regularly. Therefore, medical equipment planning must keep pace with this dynamic landscape while adhering to strict regulatory standards and managing significant financial investments. This process requires a deep understanding of the hospital’s clinical, technical, and financial needs.
This article aims to provide a detailed overview of the essential steps hospitals need to take to effectively plan for their medical equipment needs in the modern era. By reviewing these steps, hospitals can enhance their ability to deliver exceptional healthcare and achieve long-term sustainability.
Medical Equipment Planning
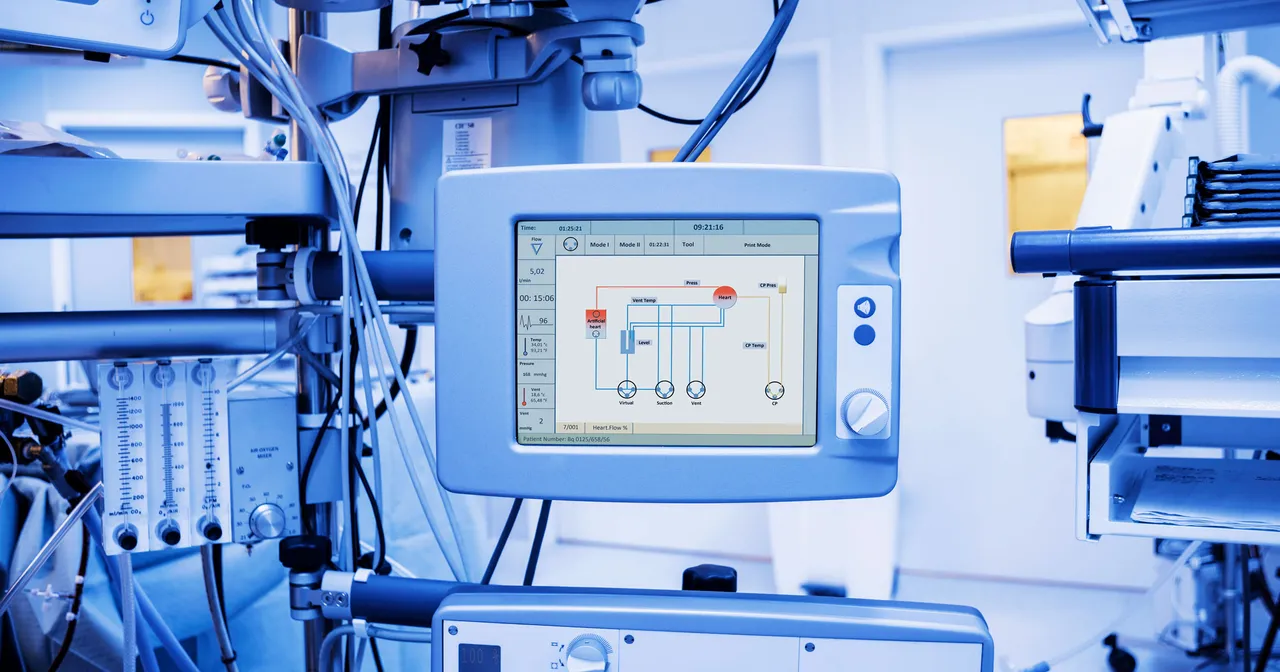
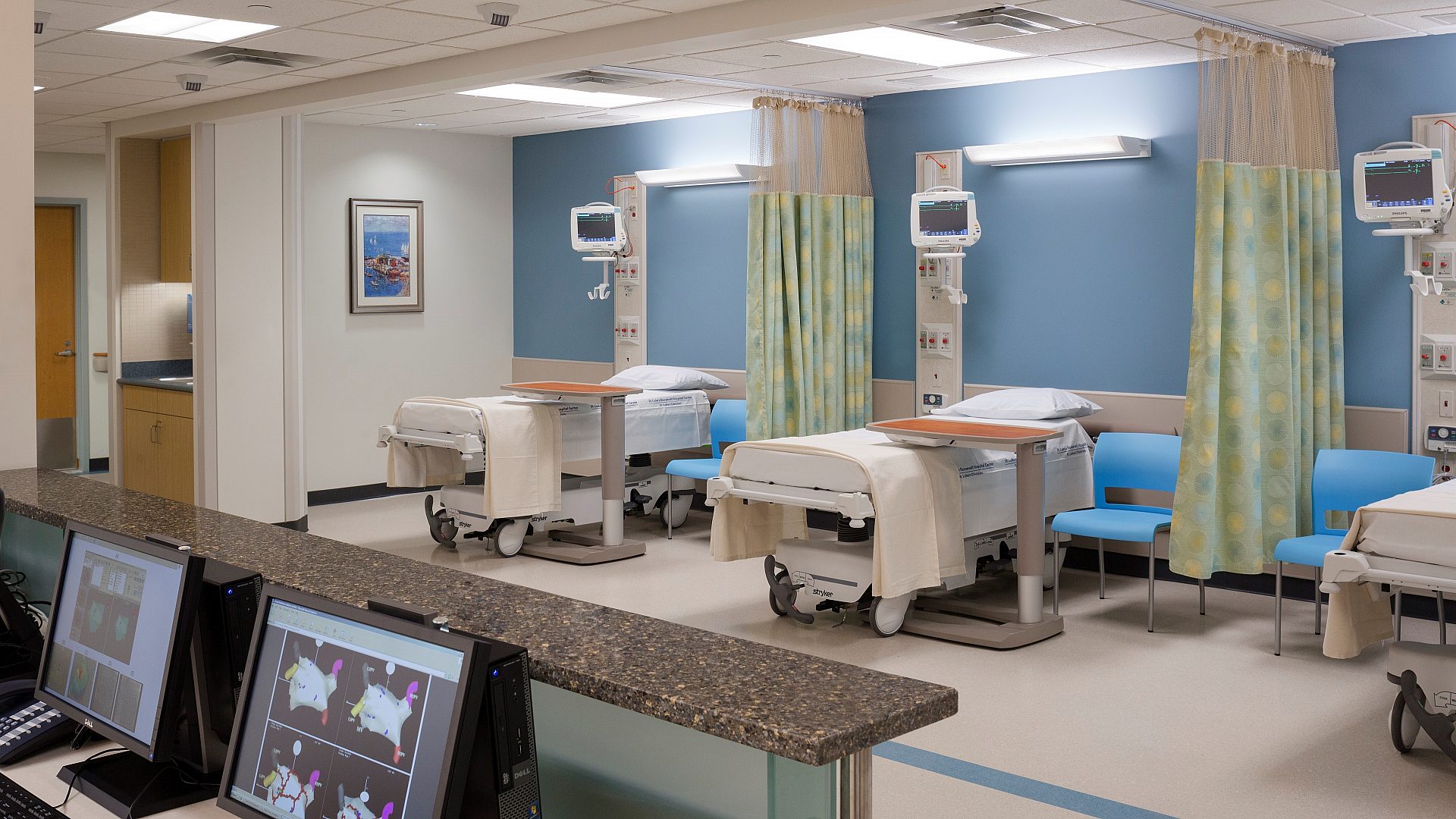
There is no doubt that modern medical equipment plays a pivotal role in delivering high-quality healthcare and improving patient outcomes. Contemporary hospitals heavily rely on a wide range of advanced devices for diagnosis, treatment, monitoring, and rehabilitation. The efficiency and proper availability of these devices directly impact the quality of healthcare services provided and the effectiveness of clinical operations.
Moreover, medical equipment is highly complex, and its technology is constantly evolving. As a result, it requires a high level of knowledge regarding precise installation procedures, design standards, and environmental conditions to ensure optimal performance. These requirements present numerous design challenges while also considering intricate logistics and reducing overall costs.
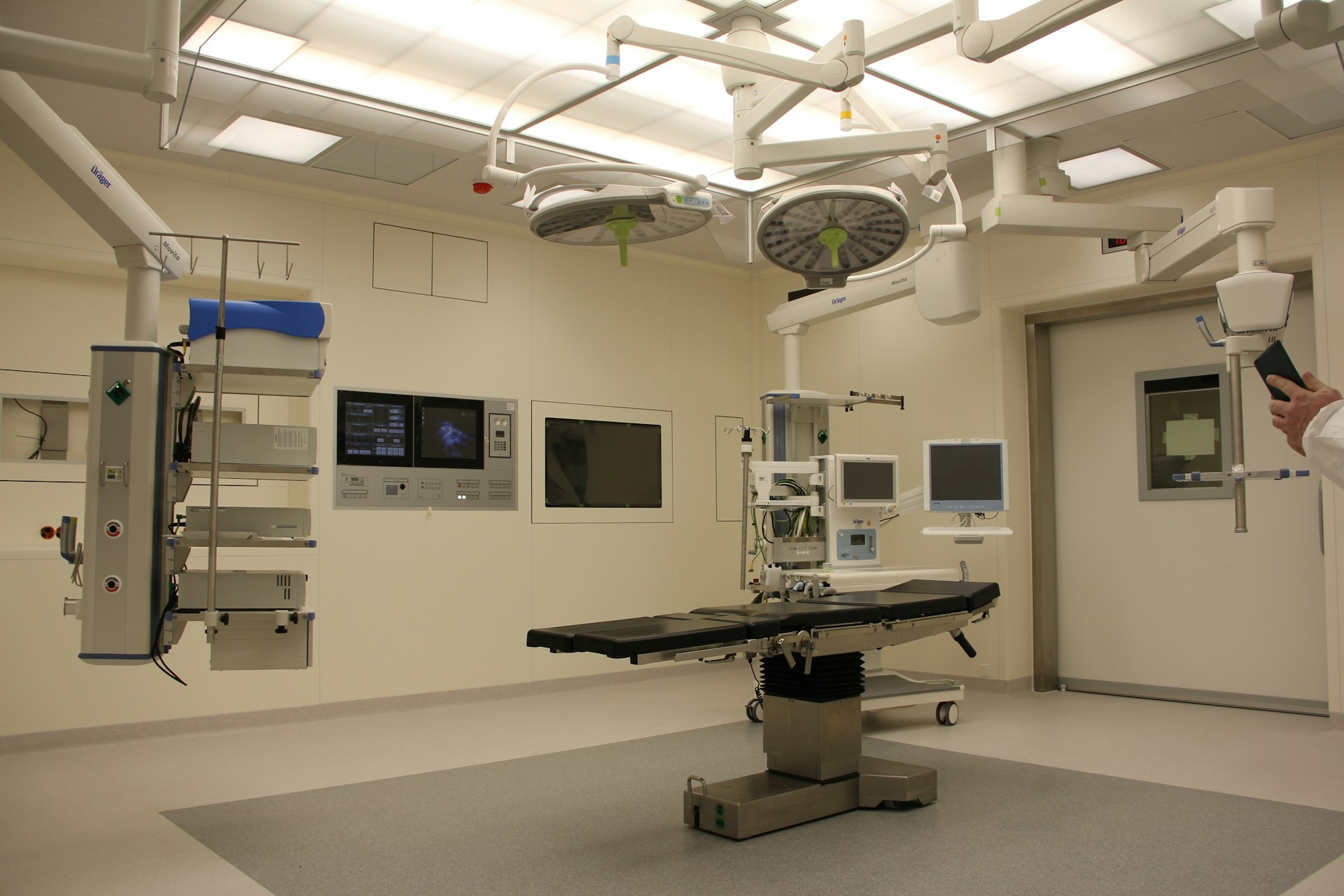
Essential Steps for Medical Equipment Planning in Modern Hospitals
Medical equipment planning is not merely a logistical task; it is a strategic necessity for modern hospitals. This planning involves adopting a comprehensive approach to ensure that hospitals acquire the right equipment, in the right place, at the right time, and within the available budget. This strategic perspective is essential for optimizing resource allocation and achieving the hospital’s organizational goals.
1- Understanding the Hospital’s Needs
The fundamental step in planning medical equipment is a comprehensive understanding of the patient population served by the hospital. This includes analyzing demographics, prevailing health conditions, and social and economic factors to predict the types and volumes of medical services required. For instance, the needs of a hospital in an area with a large elderly population will differ from those of a hospital serving a younger demographic.
It is also crucial to clearly define the specialized departments and services offered by the hospital. These specific departments and services directly determine the hospital’s equipment requirements. For example, the cardiology department will require different equipment from the orthopedic surgery department, and a pediatric hospital’s needs will differ from those of a facility focused on elderly care. Therefore, a clear understanding of the hospital’s specialization and service portfolio is essential for effective medical equipment planning.
Before planning for new equipment, it is necessary to evaluate the current inventory of medical devices. This includes documenting the specifications, age, condition, and functions of existing equipment to determine whether upgrades or replacements are needed. This assessment helps avoid unnecessary purchases and ensures that the hospital’s equipment aligns with its present and future needs.
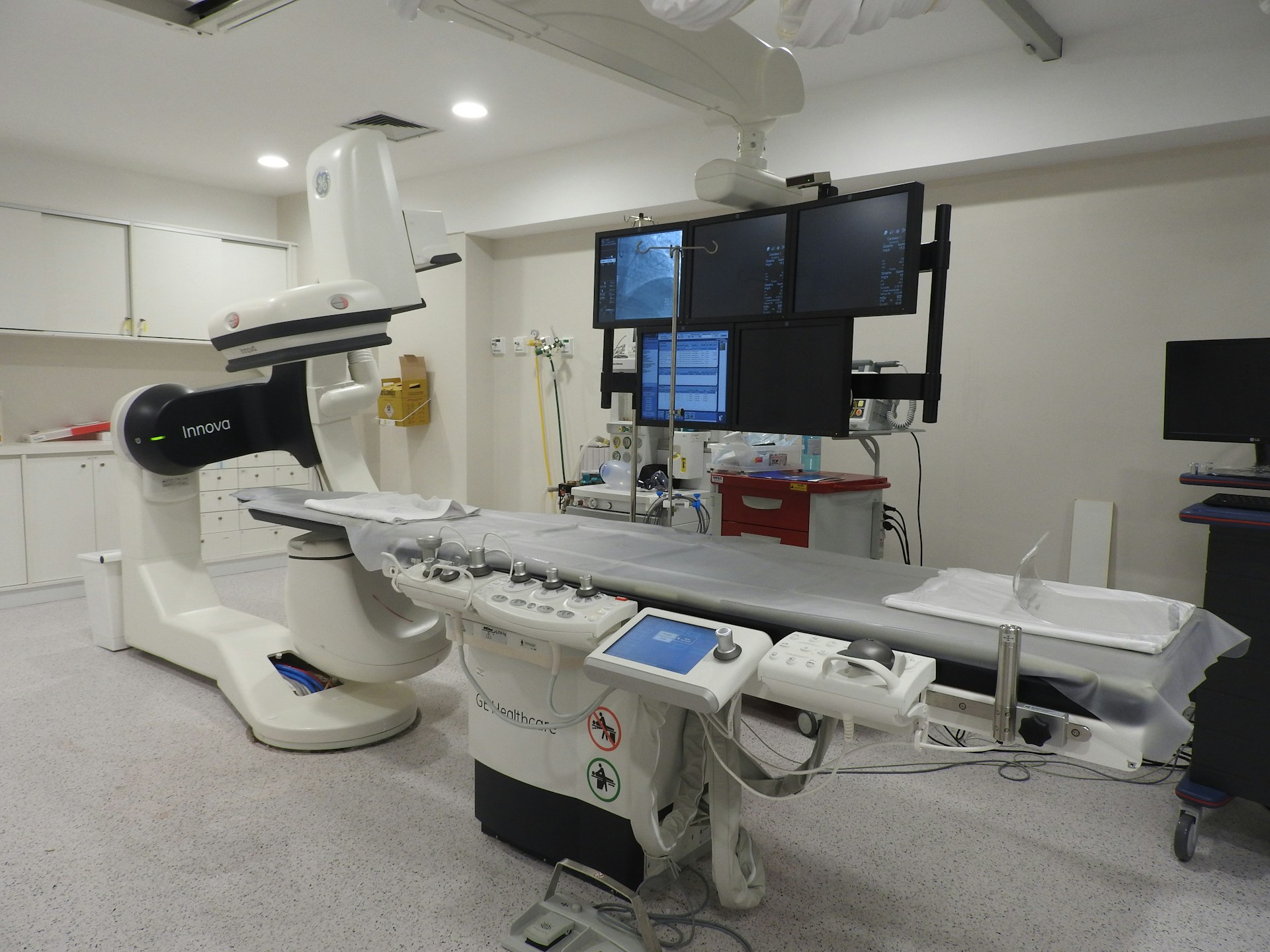
A comprehensive needs assessment forms the basis of effective medical equipment planning, ensuring that the procurement of equipment aligns with the hospital’s mission and patient needs. Without a clear understanding of whom the hospital serves and what services it offers, any effort to plan for medical equipment will be misplaced. Analyzing patient demographics helps predict the types and volumes of medical services required, which in turn determines the necessary equipment. Similarly, knowing the current inventory prevents over-purchasing and highlights areas that need updating.
2- Planning for Functionality and Efficiency
Medical equipment planning should focus on seamlessly integrating technology with the existing hardware and IT systems in the hospital while considering future technological developments. Modern medical devices often need to integrate with the hospital’s existing IT systems, such as electronic health records and other medical devices. The planning must account for the compatibility and interoperability of new equipment to ensure smooth data exchange and efficient workflows. Moreover, anticipating future technological advancements is critical to avoid purchasing equipment that may quickly become obsolete.
Prioritizing the selection of user-friendly equipment is essential to reduce the training time required for staff and enhance efficiency among healthcare professionals. User-friendly devices with intuitive interfaces can significantly decrease the time needed for staff training and reduce the likelihood of errors, ultimately leading to increased efficiency and improved patient care.
Medical equipment planning should also include developing comprehensive maintenance and service plans to ensure continuous equipment availability and prolong its lifespan. Regular maintenance is vital for ensuring that medical devices remain operational and perform optimally. Detailed maintenance schedules and service agreements should be developed as part of the planning process to extend equipment life and minimize downtime.
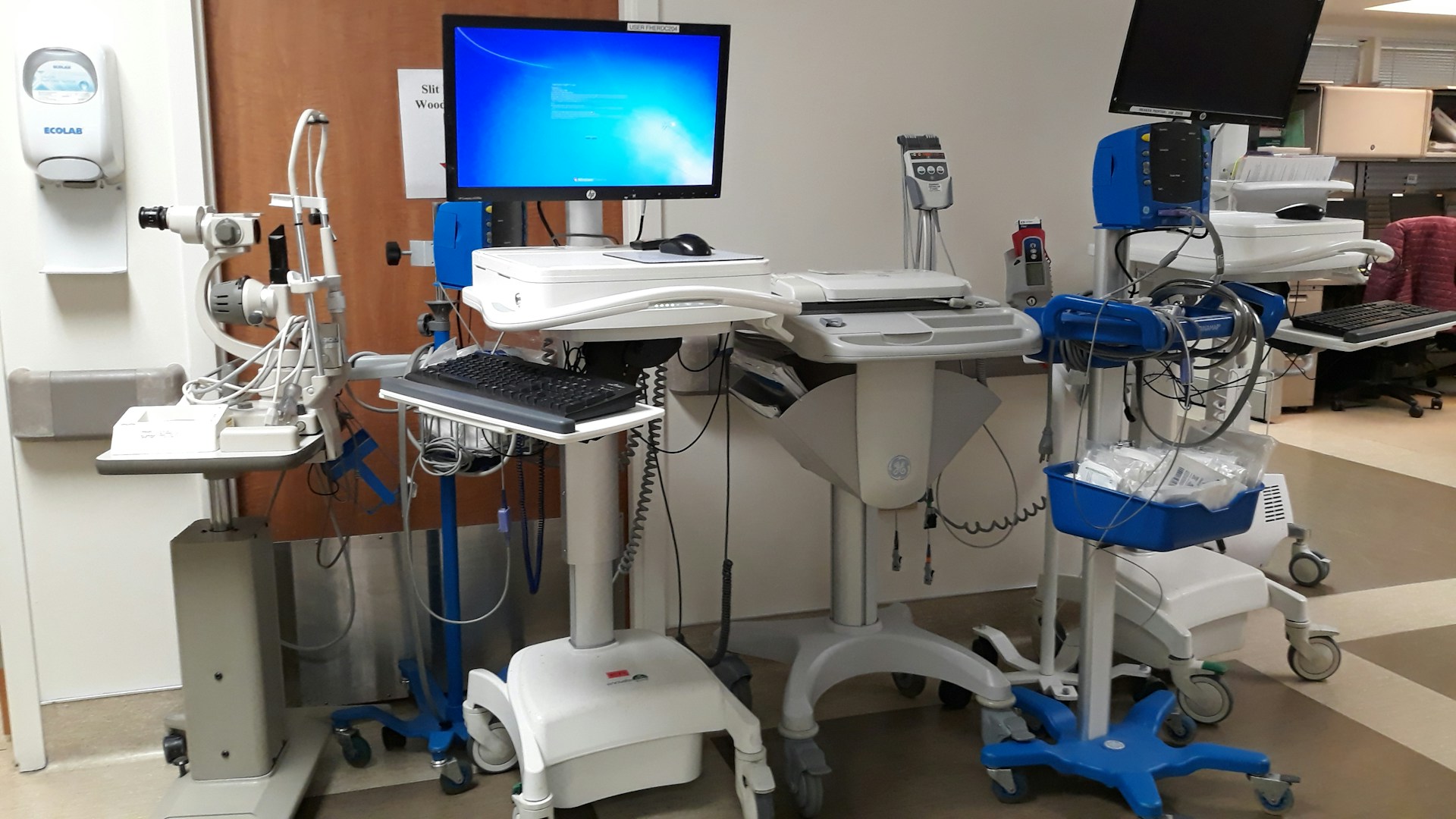
Effective workflow design around dedicated medical equipment is essential to enhance patient outcomes and staff productivity. Careful planning of the placement and utilization of medical equipment improves workflow, boosts patient throughput, and enhances staff productivity. This involves considering the physical layout of departments and the sequence of steps involved in patient care.
Planning for functionality and efficiency goes beyond mere equipment acquisition—it includes ensuring that equipment is effectively used and maintained within the hospital’s operational context. Modern hospitals are complex ecosystems where different technologies must interact seamlessly. Medical equipment planning must consider this interoperability to avoid compatibility issues that could hinder workflows and compromise patient care. Similarly, user-friendly designs reduce the learning curve for staff, leading to quicker adoption and fewer errors, while proactive maintenance planning minimizes downtime and ensures that equipment remains in optimal working condition.
3- Financial Considerations and Budgeting
Budgeting is a critical aspect of medical equipment planning, requiring meticulous financial planning to secure the best equipment at a sound investment. This involves considering not only the initial purchase price but also the long-term costs associated with maintenance, supplies, and operations to determine the total cost of ownership.
Hospitals invest in new equipment to enhance patient care, operational efficiency, diagnostic accuracy, and treatment outcomes. Evaluating the potential return on investment (ROI) helps justify the expenditure by demonstrating the expected benefits over time. Various financing options are available for acquiring medical equipment, including capital expenditure budgets, government grants, and leasing agreements. Medical equipment planning should explore these options and understand their respective advantages and disadvantages to make informed financial decisions.
Financial planning is a crucial aspect of medical equipment planning and requires a comprehensive understanding of the total cost of ownership and potential funding sources. The decision to acquire medical equipment involves a significant financial commitment that must extend beyond the initial purchase price to include long-term costs such as maintenance, supplies, and operational expenses. Evaluating the ROI helps justify the investment by highlighting the potential benefits in terms of improved patient outcomes, increased efficiency, or higher revenues. Exploring various financing options allows hospitals to optimize their financial resources and facilitate the necessary acquisitions.
4- Safety and Regulatory Compliance
Patient and staff safety must be a top priority in medical equipment planning. This involves selecting equipment with robust built-in safety features that minimize the risks associated with its use. Adhering to regulatory standards is one of the most critical steps in medical equipment planning, which includes compliance with local building codes, national legislation, and industry standards, as well as guidelines and regulations set forth by agencies such as the U.S. Food and Drug Administration (FDA).
When planning for new hospital equipment, it is essential to provide proper training for the staff to ensure their safety and the effective operation of the equipment. Additionally, when medical equipment reaches the end of its lifecycle, proper disposal methods that comply with regulatory requirements must be considered as part of the equipment plan.
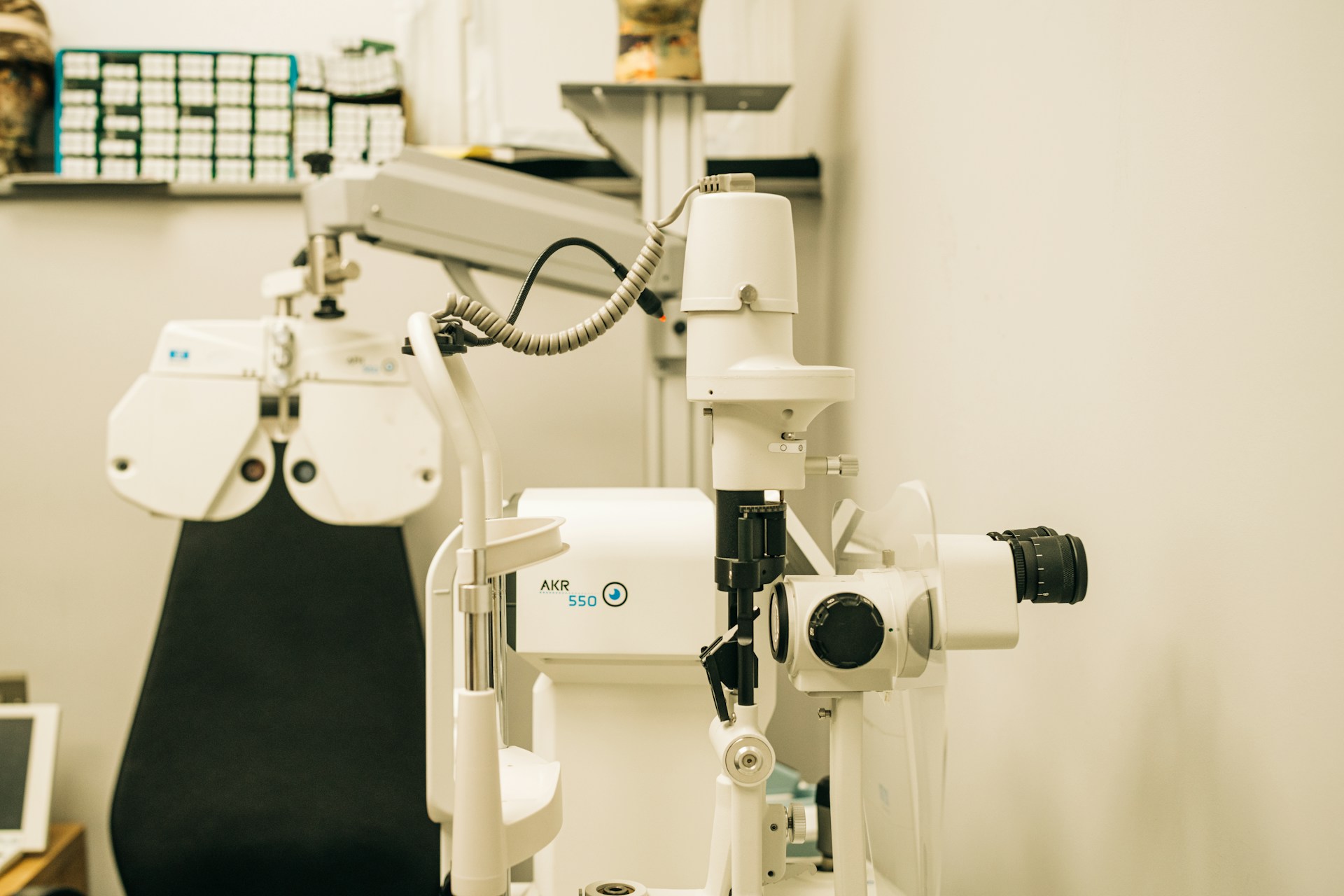
Adhering to safety standards and regulatory compliance is non-negotiable in medical equipment planning, protecting both patients and healthcare professionals. Given the inherent risks associated with medical devices, planning must prioritize safety by selecting equipment with strong safety features and ensuring compliance with all relevant regulations. Adequate training is crucial to minimizing user errors and ensuring safe and effective equipment operation, while responsible disposal of outdated equipment is essential for environmental safety and regulatory compliance.
5- Space Planning and Infrastructure
Medical equipment planners work closely with architects and builders to ensure that there is adequate and appropriate space allocated for each piece of equipment. This includes considering factors such as power requirements, climate control systems, and necessary peripherals, and ensuring the seamless integration of equipment within the healthcare facility. The physical size and weight of the machines must also be taken into account.
Coordinating systems is an important aspect of hospital design, and medical equipment must be synchronized with other building systems such as lighting, alarms, and ventilation. Hospitals should plan for future growth and ensure that spaces are flexible enough to accommodate new medical equipment as needed. Incorporating flexible designs, such as modular interfaces, can facilitate future equipment changes.
Effective medical equipment planning requires a careful study of the physical environment and infrastructure needed to support the proper performance of medical devices. Medical equipment often has specific spatial and structural requirements, so planning must involve close collaboration with architects and engineers to ensure that the facility can accommodate the size, weight, power, and environmental control needs of the chosen equipment. Proper integration with existing building systems is critical for safety and functionality, and planning for future growth ensures that the hospital can adapt to technological advances without significant disruption.
6- Effective Inventory Management
Effective inventory management is the cornerstone of successful medical equipment planning. Inventory management programs play a vital role in ensuring that the appropriate equipment and supplies are available for healthcare facilities when needed. For successful use of barcode technology in medical equipment, barcodes must be clear and well-made, and staff should be provided with appropriate scanning technology to read them. Although not mentioned as a separate point, maintaining an accurate inventory through regular audits is crucial for effective medical equipment planning.
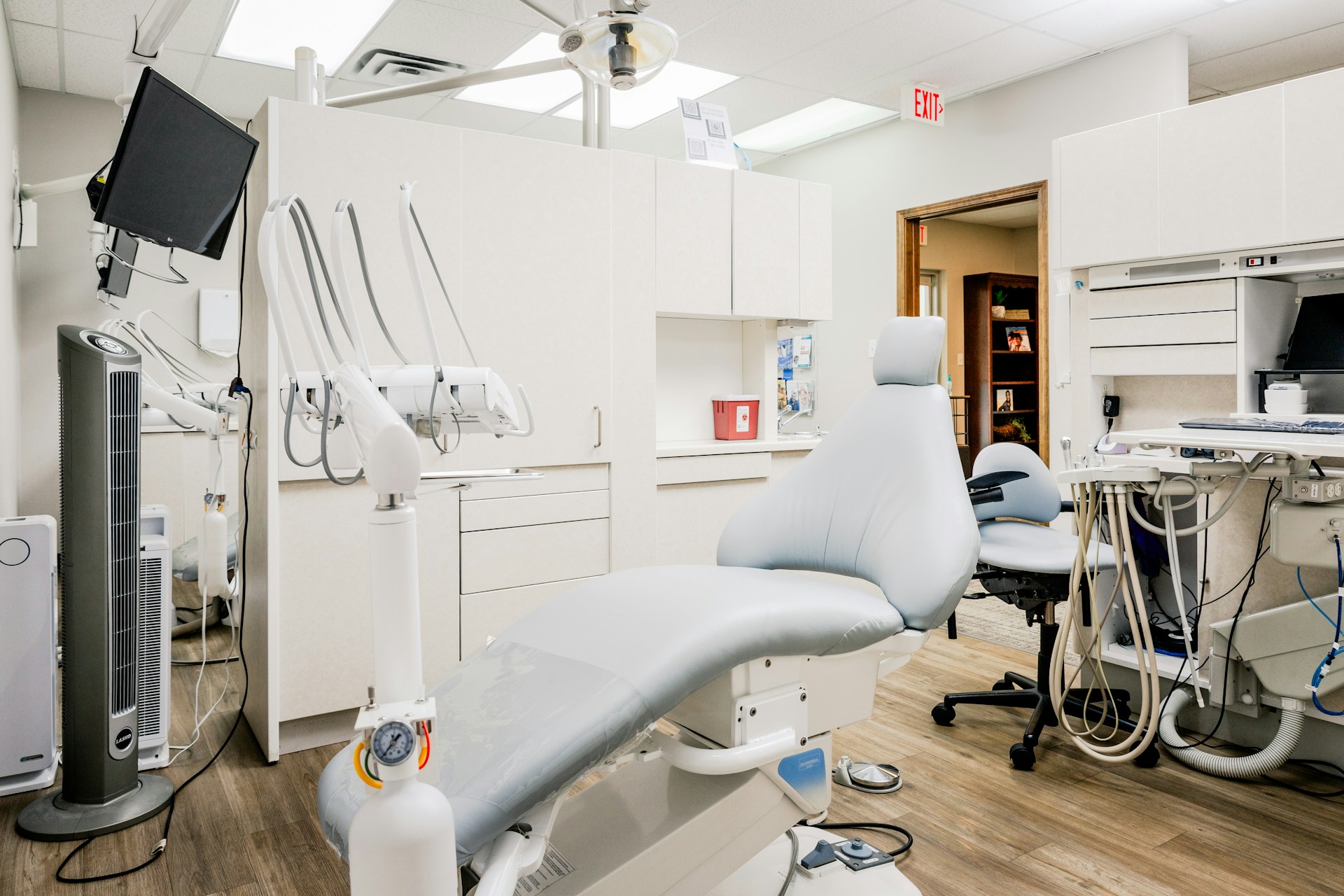
Future Planning for Medical Equipment
Hospitals must look beyond current circumstances and anticipate facility growth over time when planning for medical equipment. Equipment planning should also take into account future technological developments to avoid costly upgrades or replacements.
Future-oriented medical equipment planning involves having a long-term vision for the hospital, ensuring that current investments continue to meet future needs. Hospitals are dynamic entities that may experience growth in patient numbers or an expansion in services over time. Medical equipment planning should not be limited to immediate needs but should also forecast future requirements. Selecting scalable equipment and designing flexible spaces allow hospitals to adapt to these changes without incurring significant future costs or disruptions.
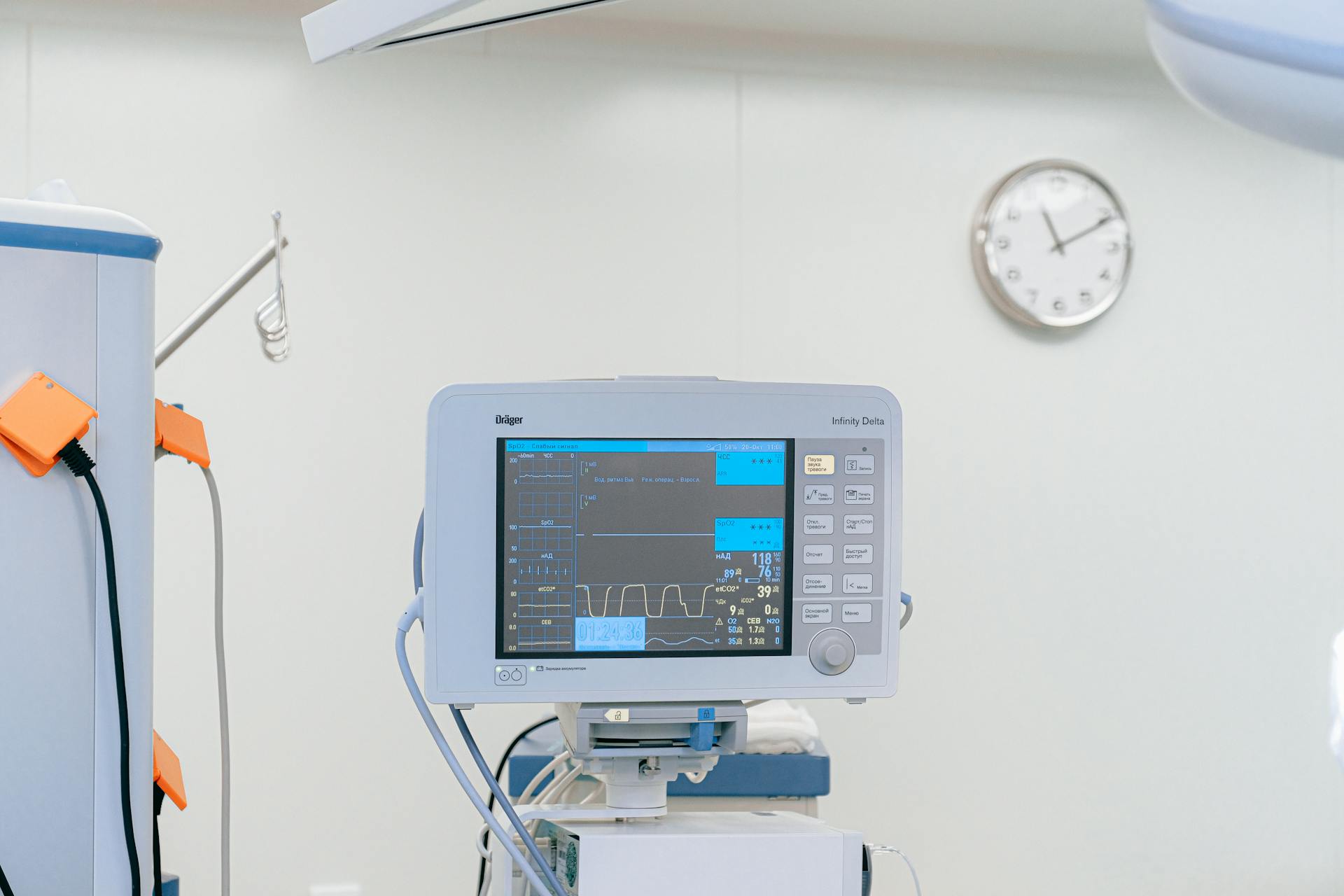
Thorough quality assurance and performance verification are essential steps in medical equipment planning to ensure that the acquired devices meet the required standards and perform as expected. Before putting medical equipment into service, it is crucial to verify that it operates correctly and safely. Comprehensive inspection and testing procedures conducted by qualified biomedical engineers can identify potential issues or defects before they impact patient care. Establishing performance metrics and monitoring equipment effectiveness post-implementation allows for continuous evaluation and ensures that the investment yields the intended benefits.
The Role of Technology in Medical Equipment Planning
The technology used in medical equipment is constantly evolving, which requires a high level of expertise for proper performance. Medical equipment planning must consider future technological developments to avoid costly upgrades or replacements. Specialized computer programs are used for collaborative building design, tracking equipment specifications, generating progress reports, and cost estimates.
Technology plays a dual role in medical equipment planning: as a subject of the planning process and as a tool to facilitate it. The rapid technological advancements in medicine mean that medical equipment planning must be forward-looking and anticipate future innovations. Additionally, technology itself provides valuable tools to manage the complexities of equipment planning—from collaborative design platforms to inventory management systems. The expertise of technology managers is crucial in navigating this evolving landscape and ensuring that technology investments align with the hospital’s strategic objectives.
The Importance of Engaging Medical Equipment Planning Experts
Medical equipment planners possess the knowledge and experience to determine specifications, overall cost, and more. Vendors can ensure that everything is classified correctly and that equipment is shipped to the right location on the right date and time. Experienced professionals can assist organizations in identifying any hospital equipment that their laboratory or facility may require.
Engaging external experts in medical equipment planning can provide valuable insights and ensure a more efficient and effective planning process, especially for complex projects. Medical equipment planning is a specialized field that requires an in-depth understanding of medical technologies, regulatory requirements, and best practices in project management. Involving experienced consultants enables hospitals to access this expertise, helping them make informed decisions, avoid costly errors, and ensure a smooth and successful equipment acquisition process.
Effective medical equipment planning is essential for delivering high-quality patient care and ensuring the long-term success of modern hospitals. By following these fundamental steps, hospitals can enhance their ability to meet the needs of their patients, staff, and the community as a whole.
Are you looking to advance your career in biomedical engineering? HSI Center is your ideal choice for achieving your ambitions. With our specialized and diverse training programs, we equip you with the necessary skills and knowledge to be at the forefront of the continuous evolution in the healthcare industry. Let us accompany you on a journey to build an exceptional professional future through expert guidance and innovative consulting services. Join us now and become one of the pioneers making a real difference in improving the lives of others.
Source: Comprehensive Guide to Medical Equipment Planning, Budgeting, and Procurement