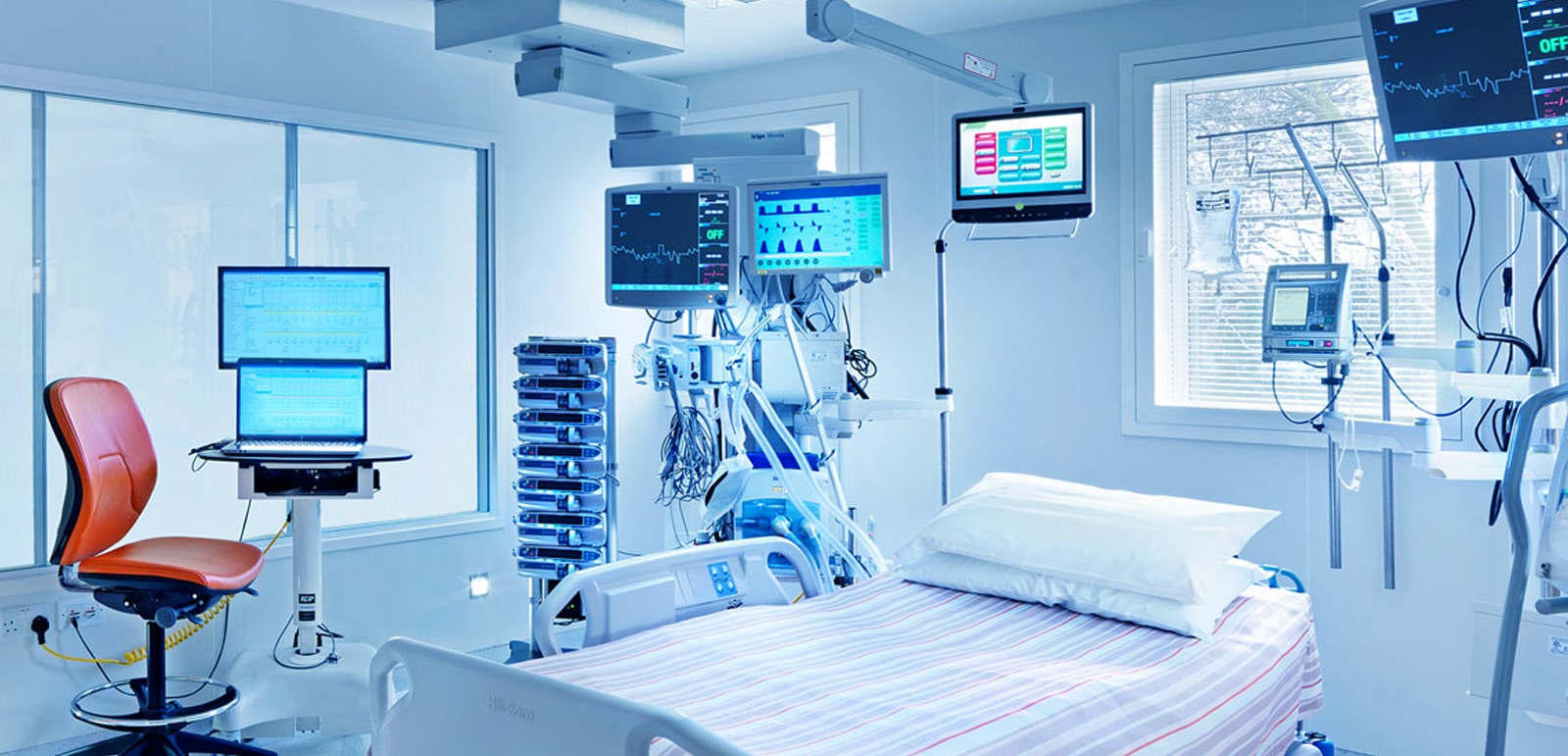
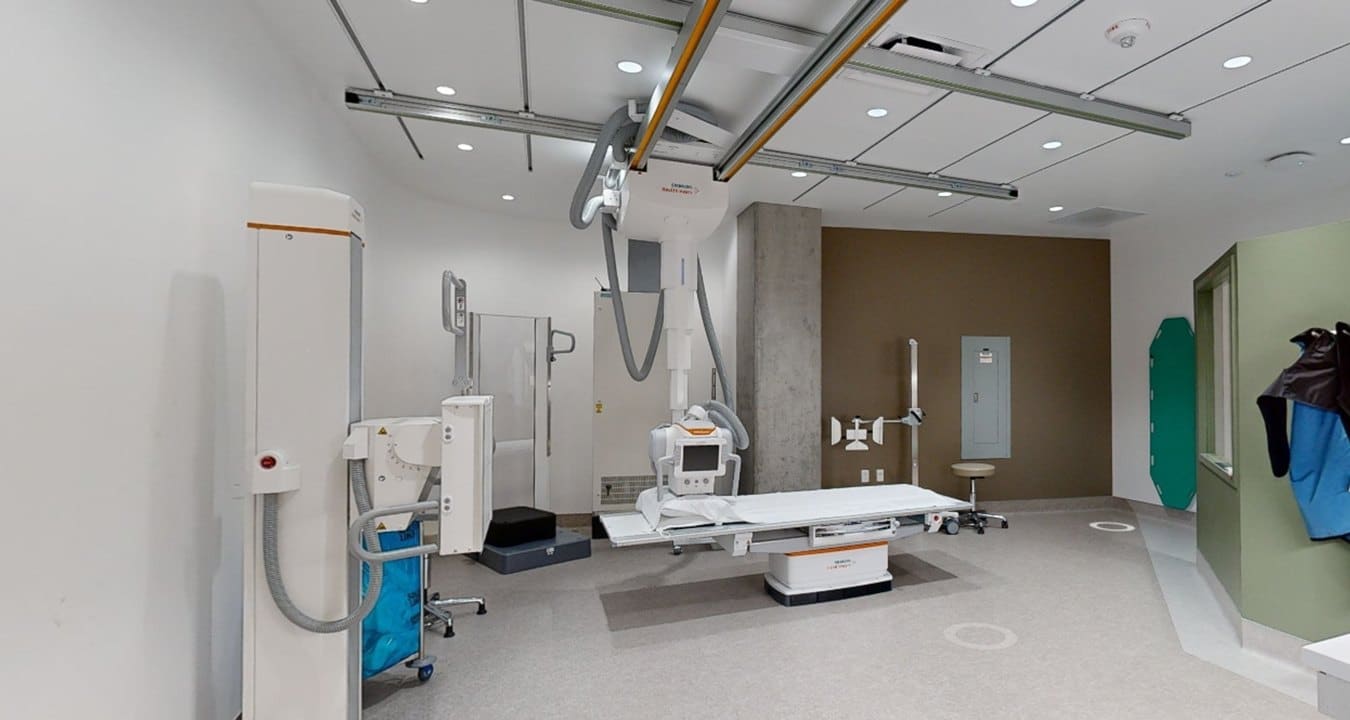
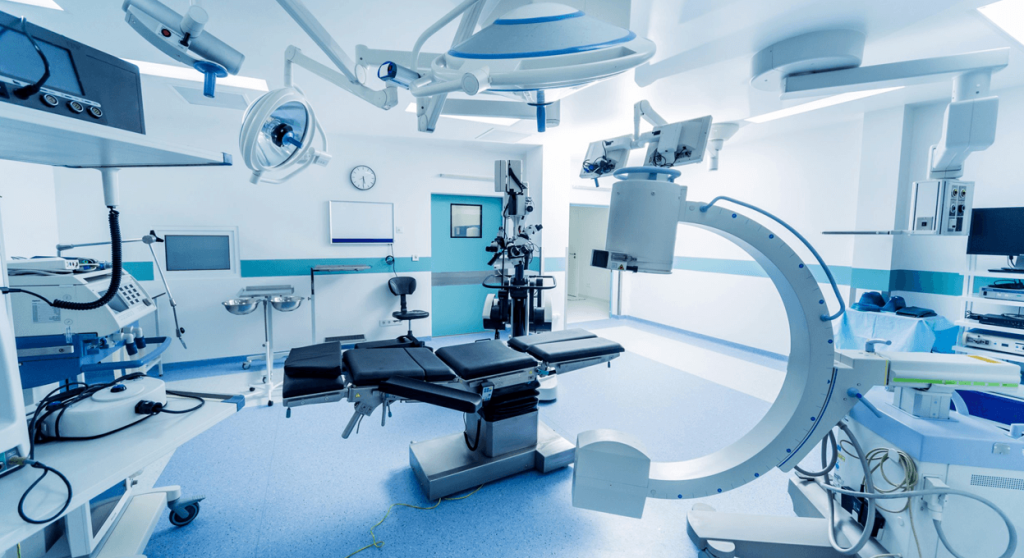
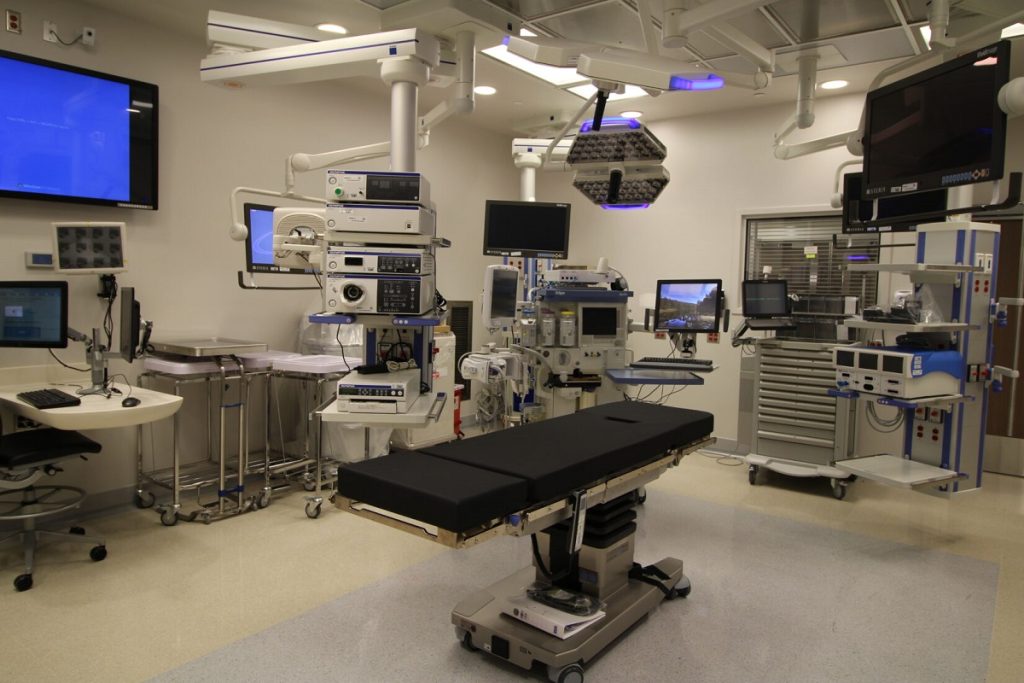
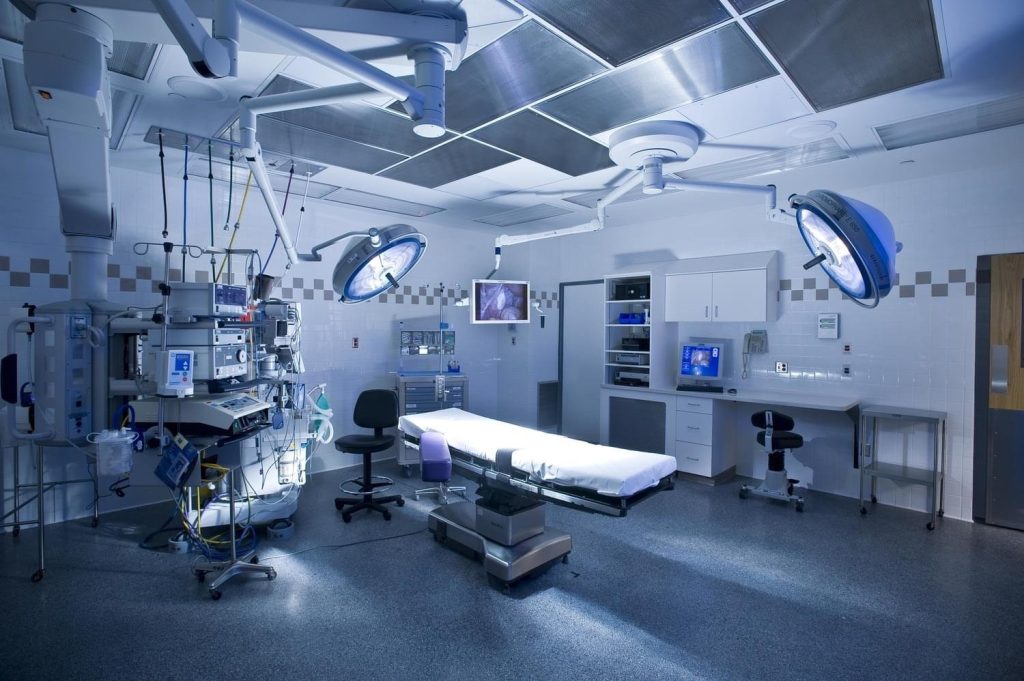
There is no doubt that the Intensive Care Unit (ICU) is one of the most crucial departments within medical facilities. However, the spotlight on the importance of ICU design gained momentum with the COVID-19 pandemic, which highlighted the critical need for such units. Modern ICUs are no longer limited to a single unit handling all critical cases. Facilities with specialized departments, such as surgery, pediatrics, neonatology, and cardiology, often have separate ICUs tailored to each specialty. Let’s explore how ICUs have evolved over time to meet patients’ needs.
Designing an Intensive Care Unit
Establishing an effective ICU requires specialized architectural and structural design to meet the demanding needs of intensive care. Studies indicate that efficient ICU design has a direct impact on patient morbidity and mortality rates, reduces medical errors, shortens patient stays, improves outcomes, and helps lower treatment costs.
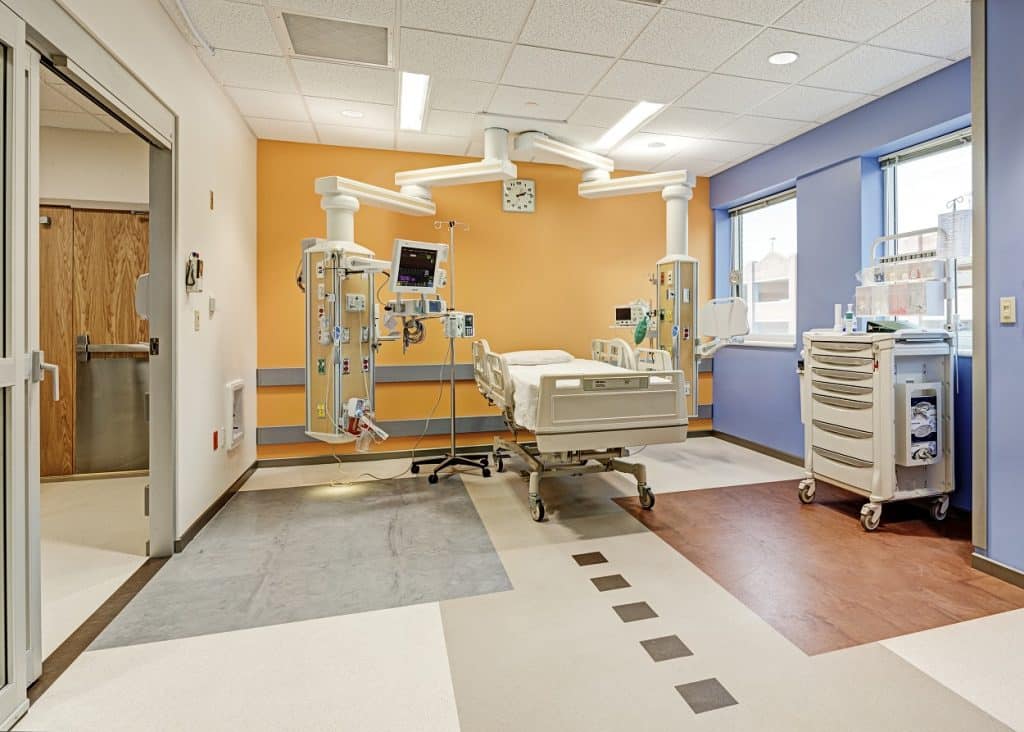
ICU vs. Critical Care Units
What is the difference between an Intensive Care Unit (ICU) and a Critical Care Unit (CCU), also known as a Coronary Care Unit? Both are designed to provide specialized medical care for critically ill patients.
Patients may be admitted to an ICU for various reasons, including planned admission after surgery, unplanned admission due to an accident, or a severe decline in health.
ICU teams consist of highly skilled professionals, such as ICU nurses, doctors, and specialists, trained to provide critical care to patients suffering from diverse medical, surgical, and trauma-related conditions.
Some hospital ICUs specialize in specific medical conditions or injuries, such as major trauma, severe burns, respiratory failure, organ transplants, complex spinal surgeries, and cardiothoracic procedures.
Levels of Critical Care
There are three levels of adult critical care:
- Level 1: Requires basic monitoring or minor interventions after discharge from advanced care.
- Level 2: Focuses on pre-operative optimization or extended post-operative care.
- Level 3: Involves advanced respiratory support or support for at least two organ systems.
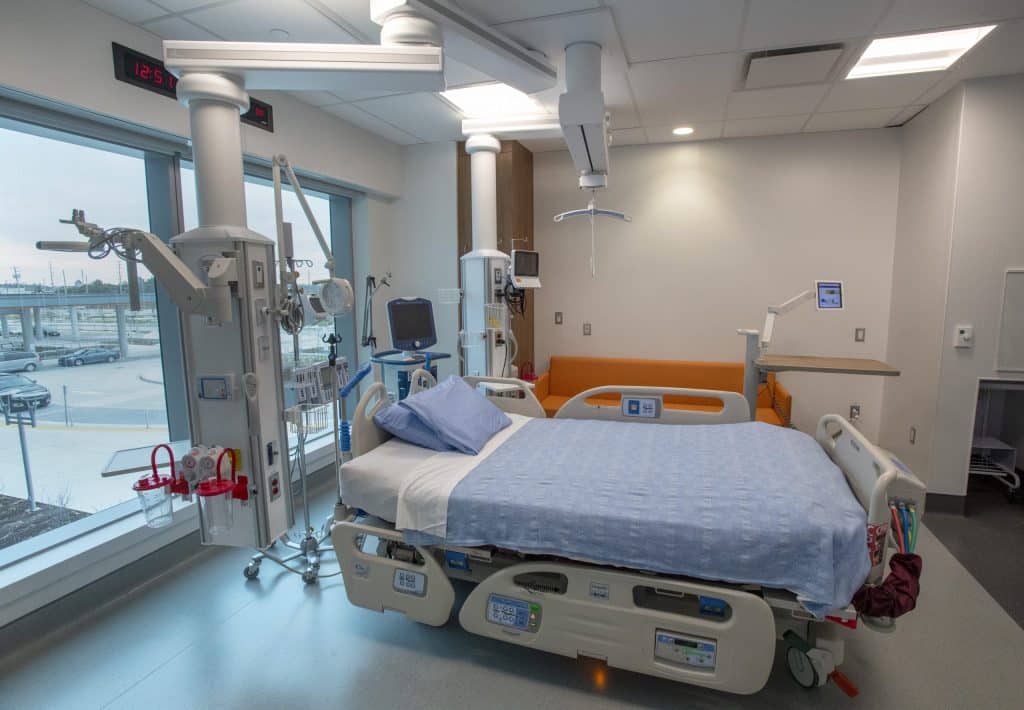
Key Elements in Designing an Intensive Care Unit
Design guidelines for Intensive Care Units (ICUs) have recently gained significant recognition for their ability to create safer and more efficient healthcare environments for both patients and staff. These designs focus on optimizing the layout and functionality of ICU rooms to enhance patient care while supporting the needs of medical teams.
These designs are not based solely on personal preferences or assumptions; they incorporate research findings and scientific evidence to guide decision-making regarding patient care, staff needs, room design, and critical care. The following guidelines emphasize room layout, organization, staff training and expertise, and overall unit design.
1. Reducing Stress Levels
One of the primary benefits of evidence-based ICU design is its ability to reduce stress levels for patients, families, and medical team members in critical care rooms. The design of patient care rooms plays a vital role in influencing the emotional state and overall well-being of both staff and patients.
Evidence-based designs consider factors such as noise reduction in patient care rooms, privacy for critical care patients, exposure to natural light in staff areas, and access to natural views. These elements help create a calming environment that promotes healing and recovery.
2. Enhancing Lighting
Lighting is a critical element in ICU design, as it impacts various aspects of patient care, room functionality, and staff performance. Evidence-based guidelines emphasize the importance of appropriate lighting conditions in critical care rooms to support clinical tasks and ensure patient comfort.
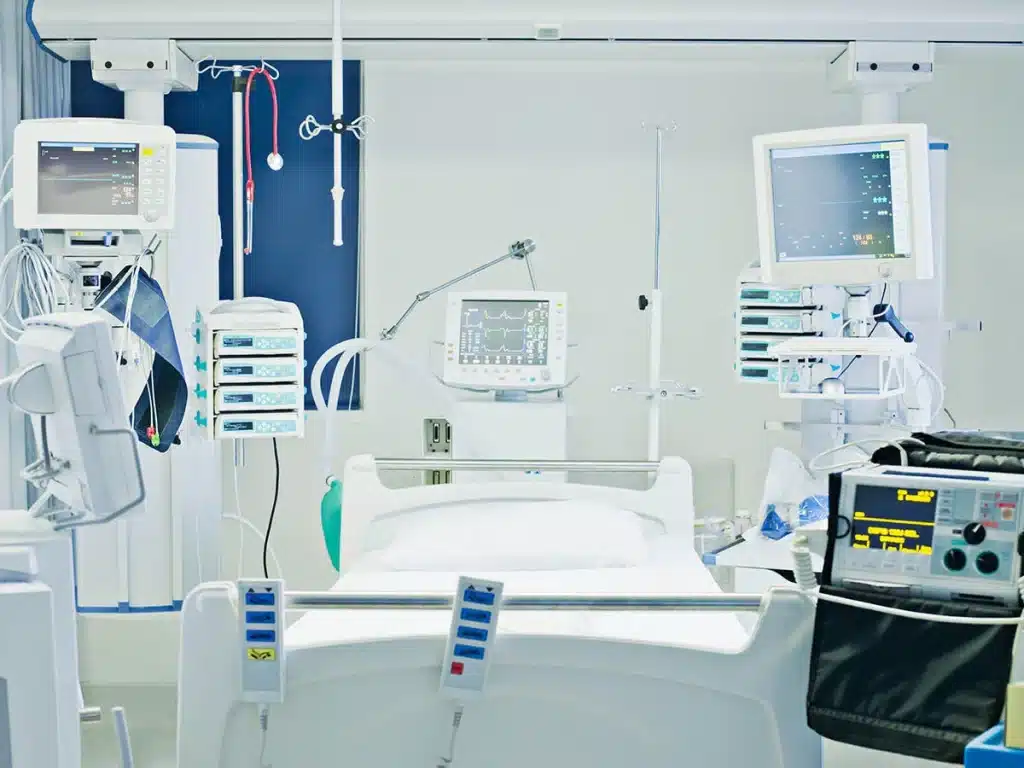
When implementing lighting solutions, staff should consider the room layout. Adequate lighting levels in critical care rooms improve visibility for medical staff while maintaining a warm and comforting atmosphere for patients.
Incorporating natural light in ICU rooms has been proven to reduce depression rates and improve sleep quality for both patients and staff. Effective lighting design is essential for creating a therapeutic environment.
3. Improving Ventilation
Proper ventilation is crucial for maintaining optimal air quality within ICUs, ensuring better patient care and reducing the risk of airborne infections for both patients and staff.
Good air circulation in critical care units minimizes the concentration of pathogens and ensures a consistent supply of fresh air for patients and medical staff. Adequate ventilation also helps regulate temperature within critical care units, creating a comfortable environment conducive to recovery.
4. Soundproofing
External noise is one of the most disruptive factors in healthcare facilities, especially in ICUs where constant monitoring and medical interventions are conducted. This can disturb both patients and staff. However, thoughtful design can minimize noise levels, creating a more peaceful environment for everyone.
ICU rooms design that incorporate sound-absorbing materials, such as acoustic ceiling tiles and soundproof wall panels, help reduce noise levels. This enhances patient comfort and improves communication among healthcare workers.
5. Allocating Sufficient Space for Equipment, Staff, and Patients
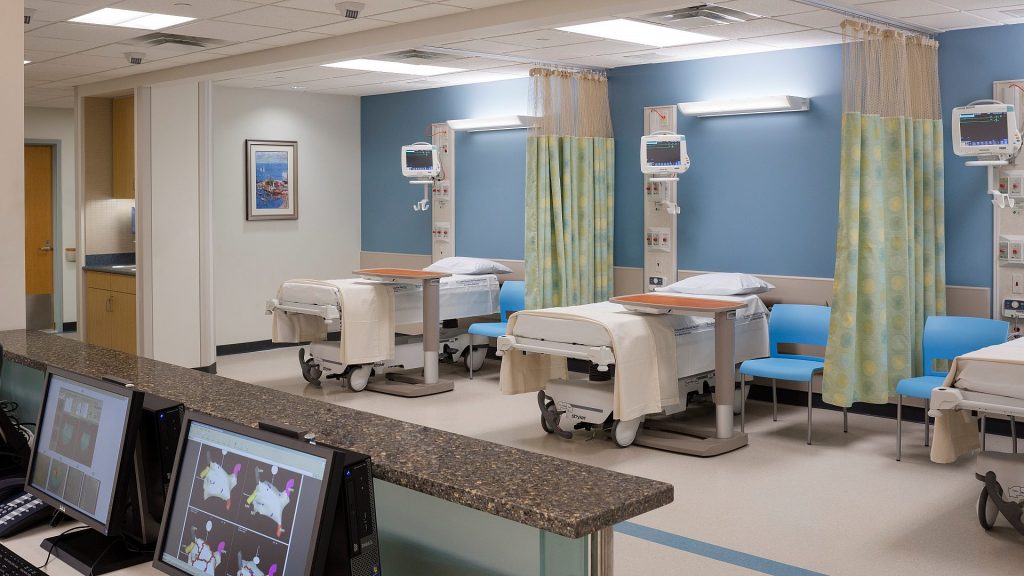
A key consideration in critical care unit design is ensuring sufficient space for patients and staff. This includes enough room to accommodate essential medical equipment, supplies, staff, and patients within the ICU layout. The design should facilitate ease of movement and accessibility for both medical teams and patients without feeling crowded or constrained.
6. Incorporating Infection Control Measures
Infection control is vital in any healthcare setting, especially in ICUs where critically ill patients and post-surgery recovery patients are more susceptible to infections. Design plays a pivotal role in ensuring effective infection control measures are implemented.
Designing ICUs with infection control guidelines in mind helps minimize the spread of diseases within critical care units, ensuring patient safety.
Considerations for ICU and CCU Design
- Key considerations for designing an ICU or a Critical Care Unit (CCU) include creating patient rooms tailored to critical care needs.
- Ensuring adequate space for patient beds, medical equipment, and staff movement is essential for effective healthcare delivery.
- Proper lighting and ventilation in patient rooms create a safe and comfortable environment, following guidelines for equipment placement and spatial requirements.
- Easy access to emergency equipment and supplies is critical for providing intensive care and ensuring patient safety in critical situations. Quick response times are essential for patient care, making accessibility to emergency equipment and supplies a top priority. These resources must be well-organized and easily accessible throughout patient rooms and other facility areas.
- Soundproof rooms reduce noise and provide patients with a quiet, restful environment. These rooms should also be equipped with necessary medical equipment.
- Effective monitoring and care in healthcare rooms require clear visibility and communication between patients and staff. Design plays a crucial role in ensuring optimal health outcomes.
In conclusion, ICU rooms are among the most critical units in hospitals, offering life-saving care for patients in critical conditions. This requires meticulous design to meet patient needs, support medical teams, and ensure safety. At HSI, we offer specialized courses to assist professionals in designing ICUs that cater to patients’ needs while supporting doctors and nurses in their work. In this article, we have outlined some essential considerations to help achieve the best design outcomes.