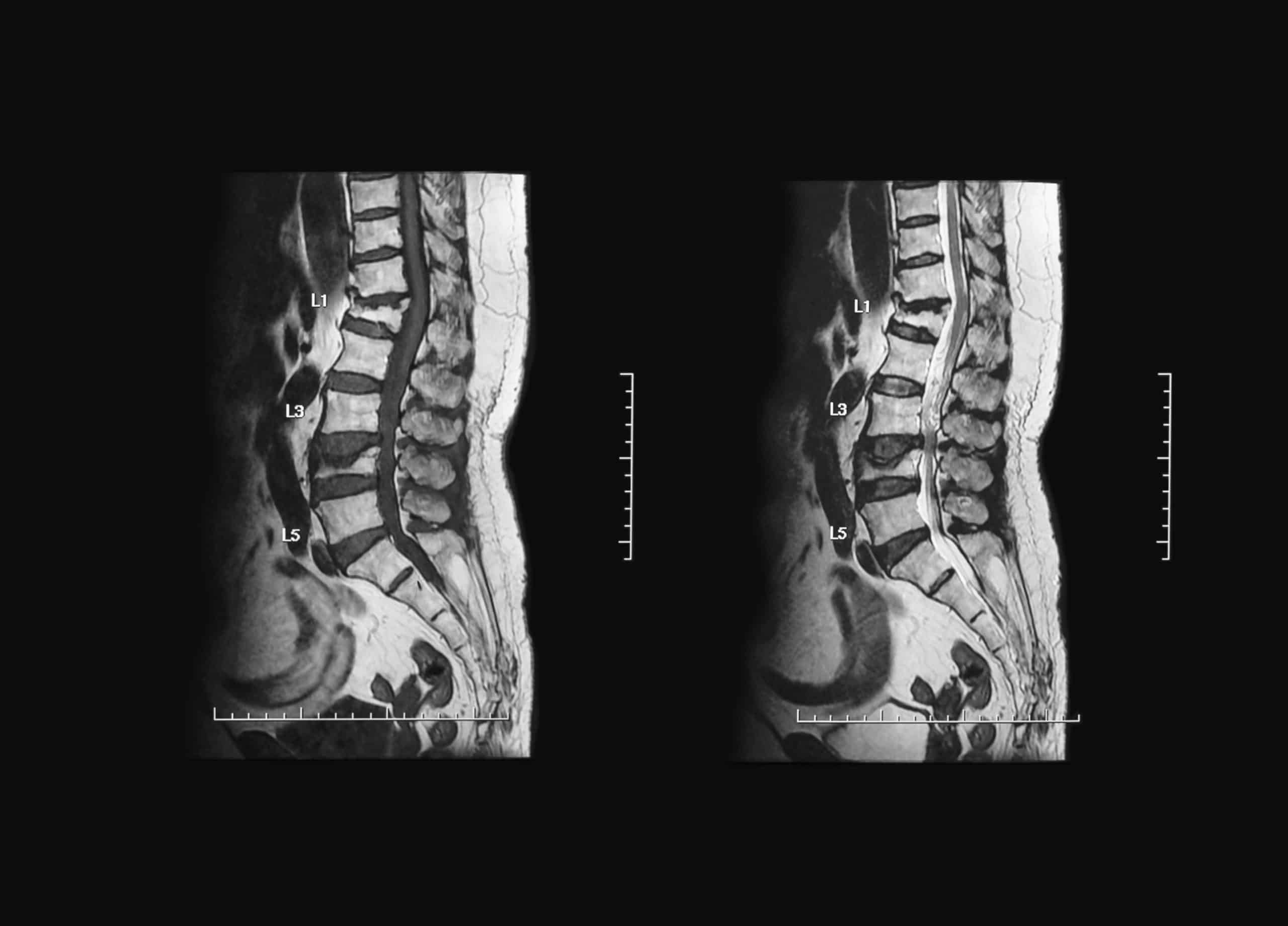
AI’s Role in Early Disease Detection via Medical Imaging
The use of AI in medical imaging represents a major breakthrough in integrating technology into healthcare. This integration is not just a technological advancement, but a qualitative leap in enhancing diagnostic and treatment plans. AI is leveraged in the early detection of diseases through advanced imaging techniques. In this article, we will discuss this role and how it contributes to improving healthcare.
The Importance of AI in Early Disease Detection
We are not exaggerating when we talk about the importance of AI in healthcare and medical imaging. It goes beyond merely improving image quality and processing speed. AI capabilities in medical imaging have evolved from basic diagnostics to aiding in early disease detection. It’s no longer just about faster and clearer images, but also about saving lives through early intervention and providing personalized treatment options.
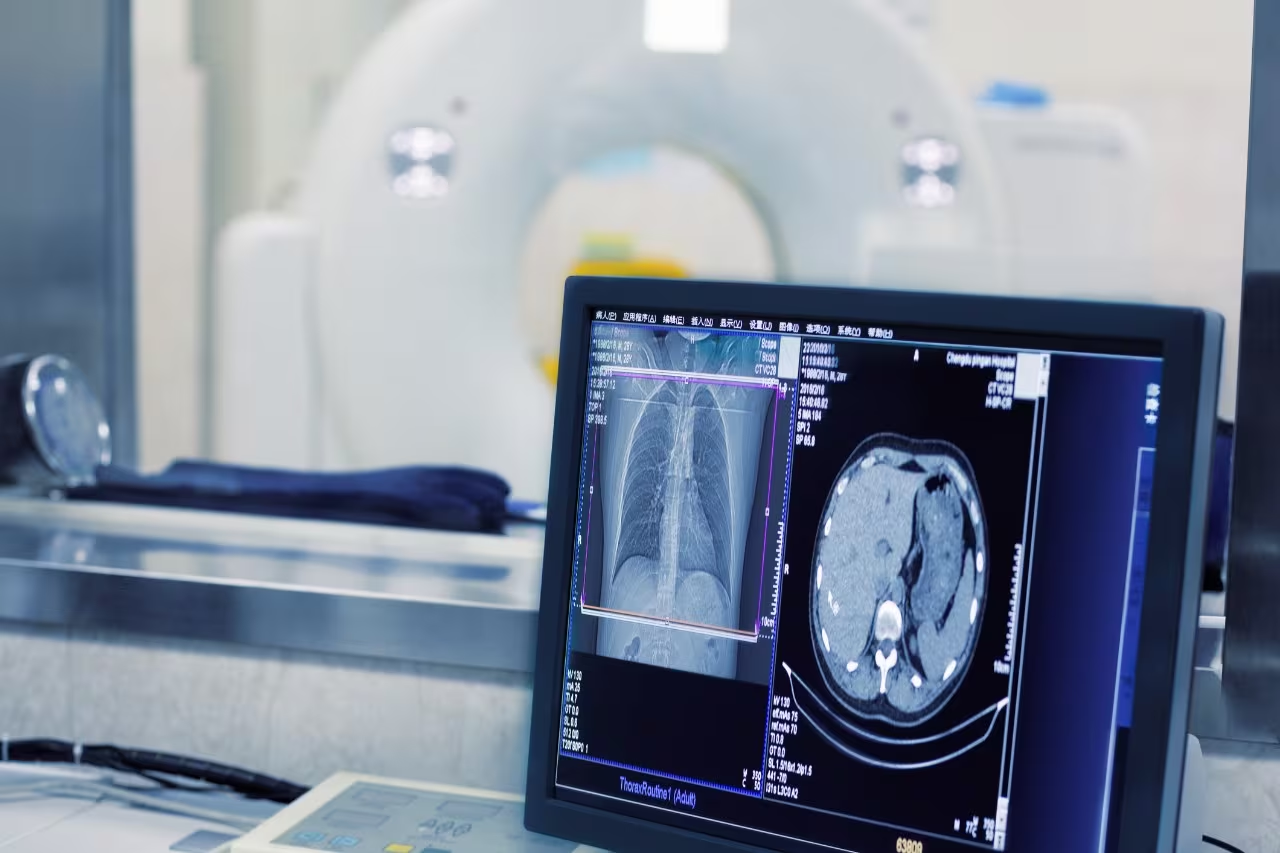
These advancements have had a significant impact on healthcare, especially in fields like oncology and neurology, where timely and accurate diagnosis is critical. More specifically, these innovations have significantly increased the number of patients undergoing screenings, enhancing not only patient outcomes and safety but also productivity and cost-effectiveness.
AI Capabilities in Medical Imaging
AI technologies have a multifaceted impact on medical imaging. They improve diagnostic accuracy, reduce human error, and enable early disease detection, ultimately raising the standard of patient care. AI can be utilized in various ways to enhance medical imaging.
The full potential of AI can be realized through the effective use of machine learning and deep learning algorithms, which are now playing a pivotal role in advancing imaging technologies.
AI Improvements in Medical Imaging
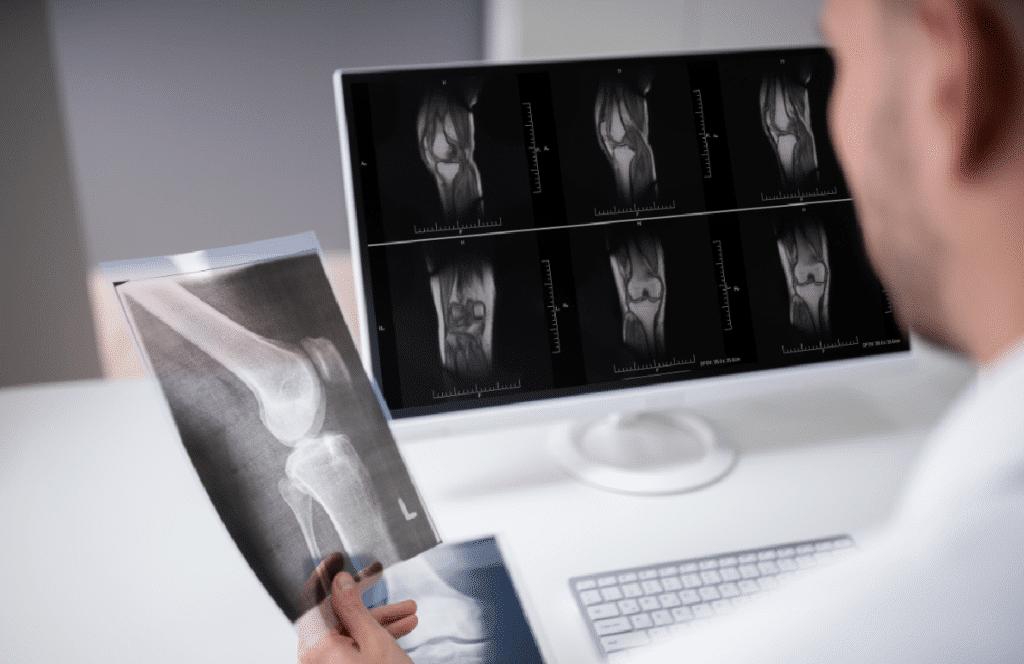
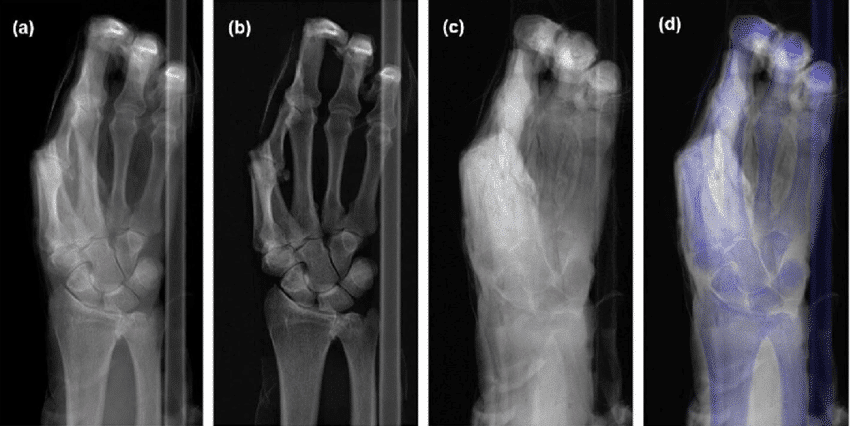
- One of the most notable advancements is image quality enhancement. AI algorithms can analyze massive volumes of imaging data, learning to detect subtle patterns and anomalies that may be invisible to the human eye. The increased clarity and resolution of these images have paved the way for more accurate diagnoses, such as the ability to detect fractures.
- Image processing speed is another area where AI makes a significant difference in early disease detection. In the past, analyzing medical images was time-consuming, which affected the timing of diagnoses and treatment.
- Thanks to its ability to quickly process and analyze large datasets, AI significantly reduces the time needed to analyze medical images. As a result, AI systems can now interpret and generate complex images much faster than traditional methods, speeding up the diagnostic process.
- By integrating deep learning algorithms, AI can identify patterns associated with specific diseases, making it a powerful tool for early detection and diagnosis. Through advanced image analysis, AI can detect abnormalities such as tumors in their early stages, greatly enhancing the patient experience.
- AI also plays a major role in personalized medicine and preventive healthcare. By analyzing medical imaging data alongside a patient’s medical history, AI can provide personalized diagnostic insights, paving the way for more tailored treatment plans.
Key Applications of AI in Medical Imaging
Current AI applications in medical imaging are significantly impacting fields such as radiology, oncology, and neurology. By harnessing AI, medical professionals in these areas can improve the accuracy and efficiency of numerous diagnoses and treat medical conditions more successfully.
These three fields demonstrate how AI applications in medical imaging are not only enhancing current diagnostic and treatment methods but also opening new horizons in personalized medicine. From improving diagnostic accuracy in radiology to aiding in the early detection of cancerous cells and neurological diseases, AI is proving its value in the healthcare sector.
Below are the key fields that benefit from AI in the early detection of diseases.
1. Radiology
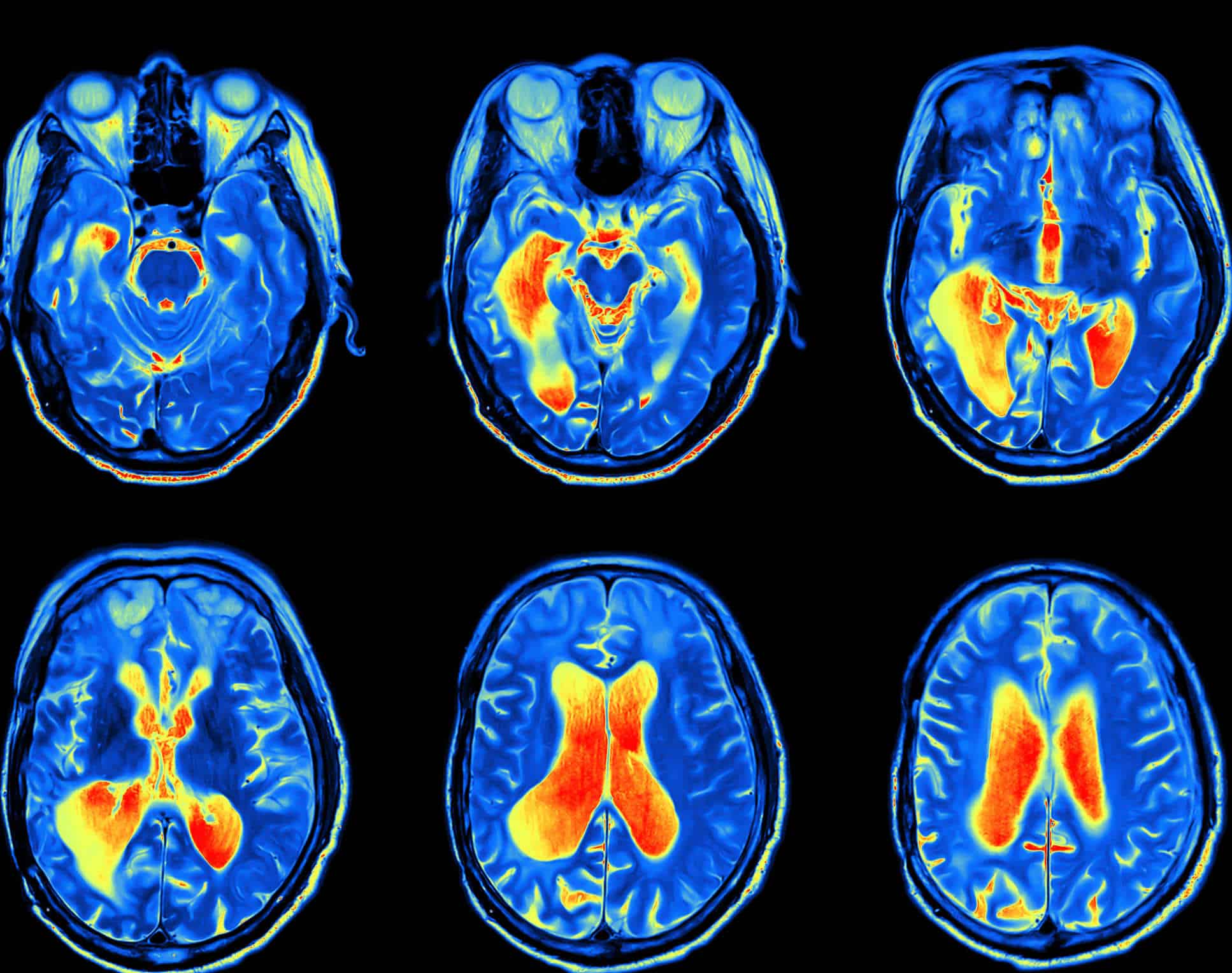
In the field of radiology, for example, artificial intelligence is primarily used to identify abnormalities in imaging scans. AI algorithms applied to computed tomography (CT) and magnetic resonance imaging (MRI) can quickly detect and segment areas of interest in scans of the lungs, liver, and brain.
2. Cancer Tumor Detection
Particular attention should be given to AI’s role in tumor imaging. It assists in detecting and monitoring cancerous tumors, improving the accuracy of cancer screenings. For instance, deep learning AI techniques have been used to analyze mammograms and accurately distinguish between malignant and benign tumors.
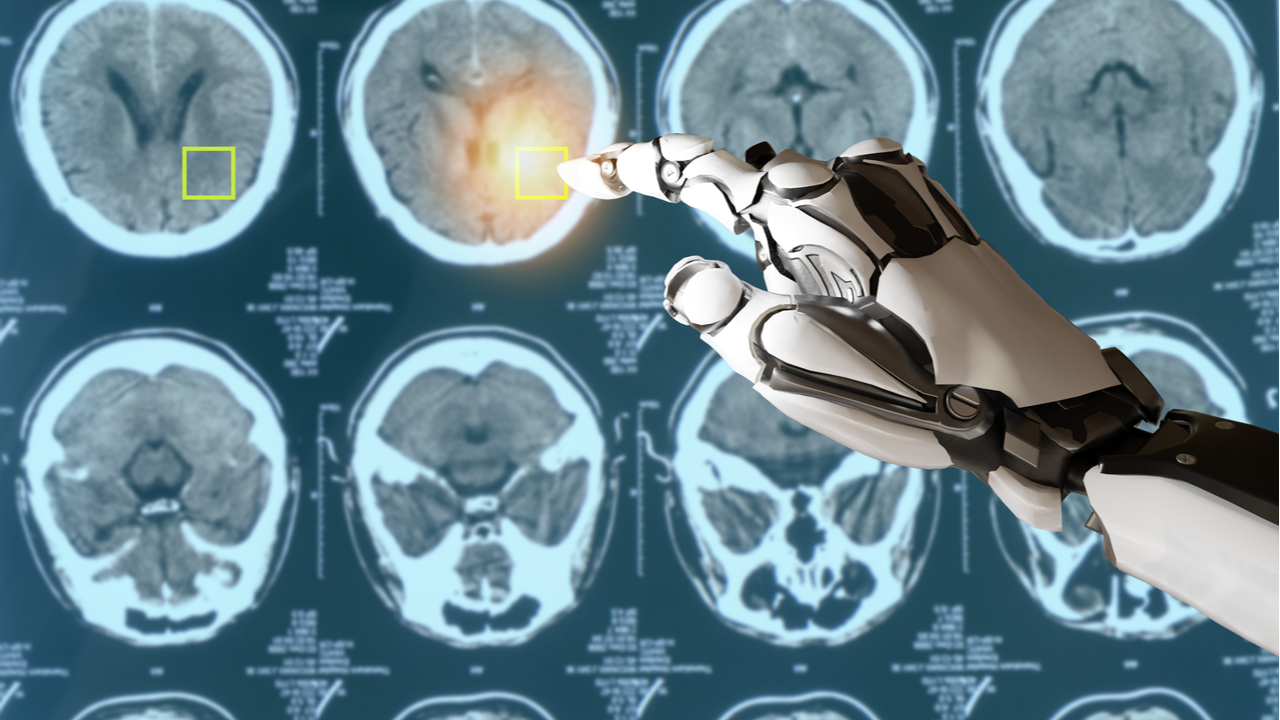
3. Neurology
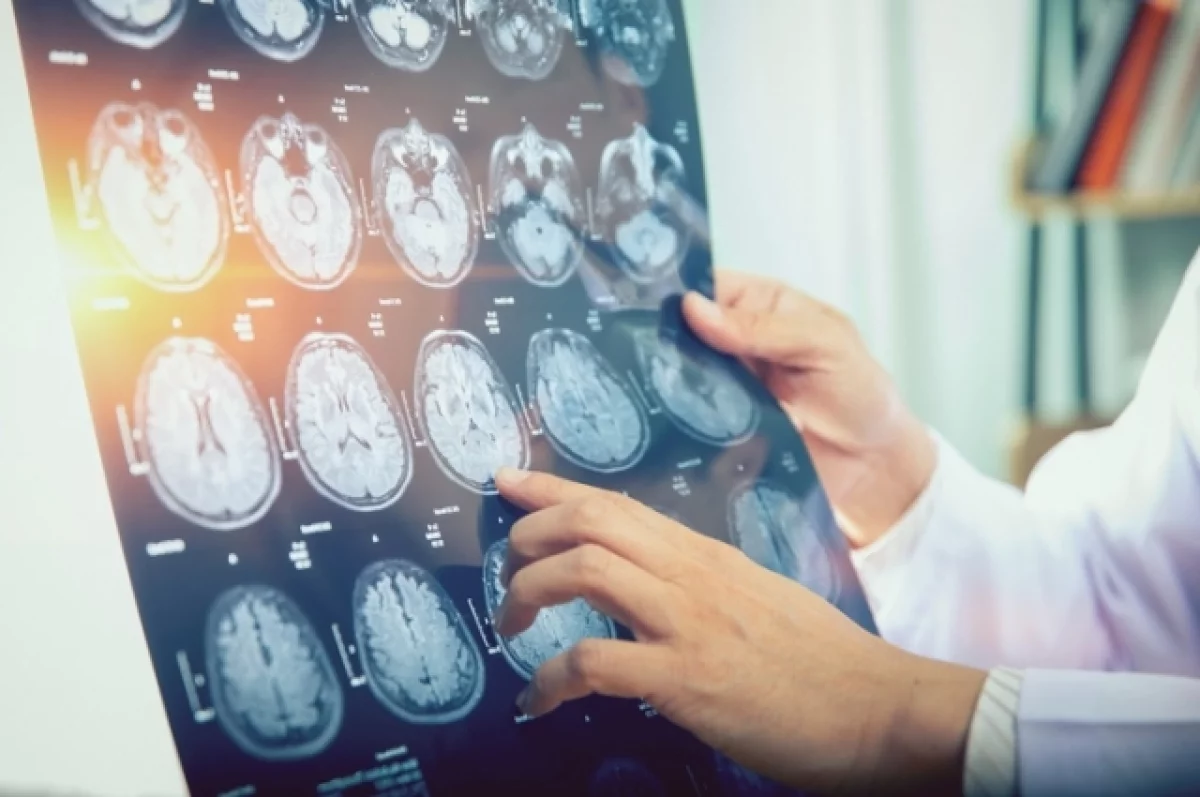
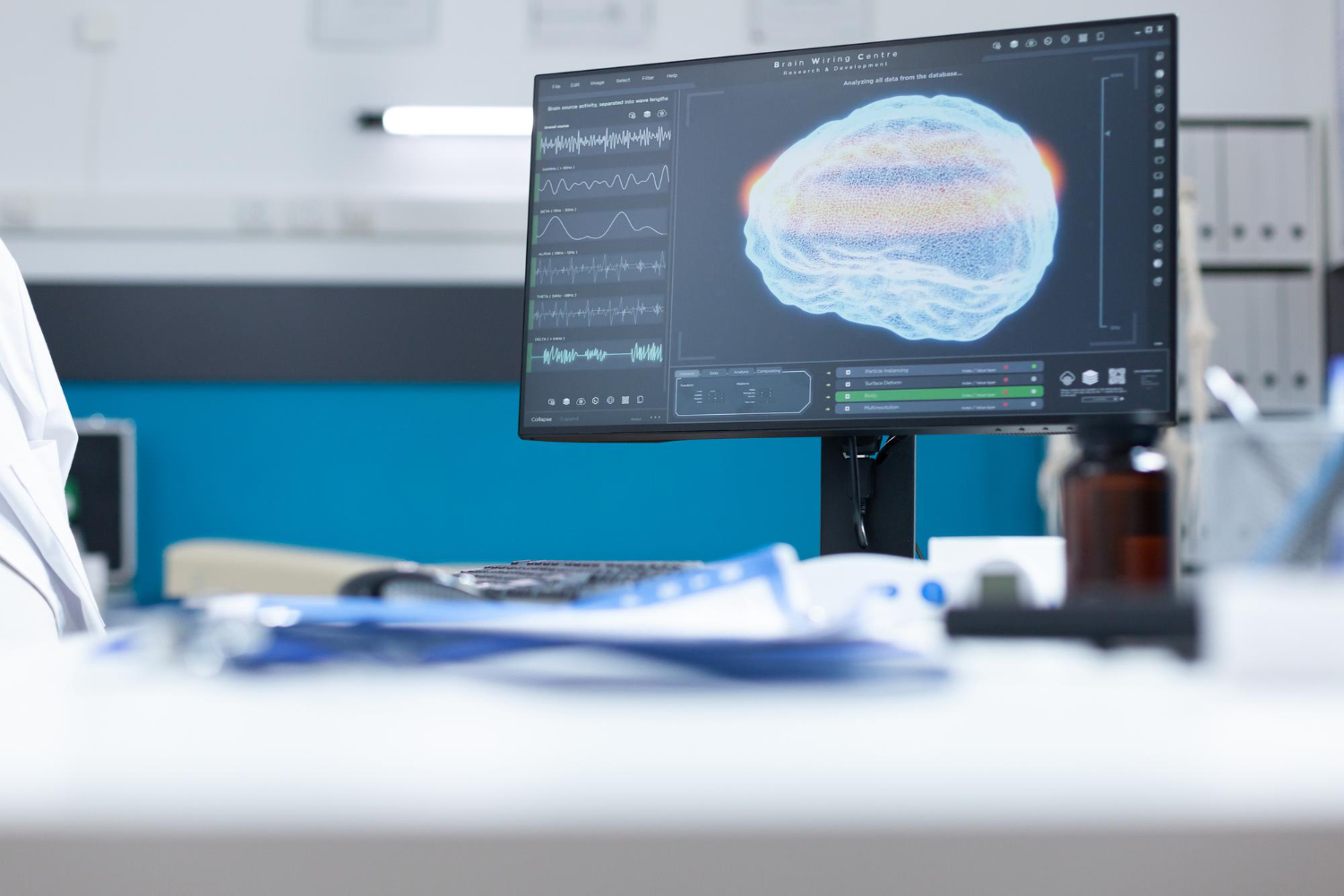
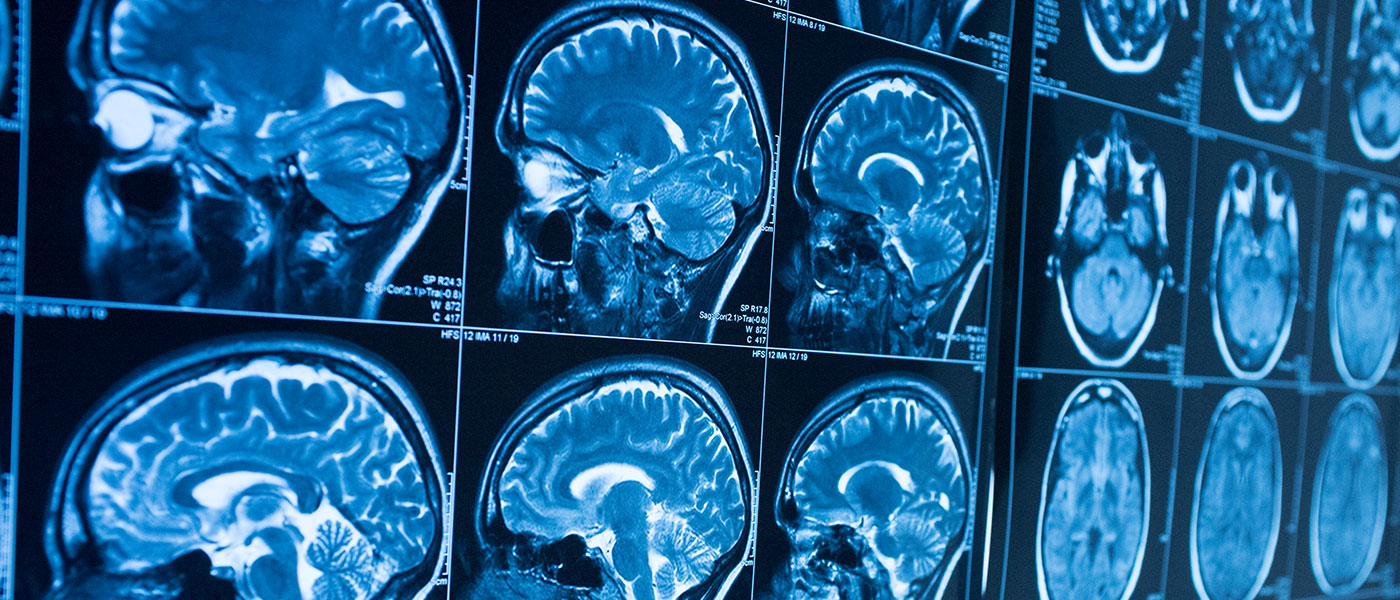
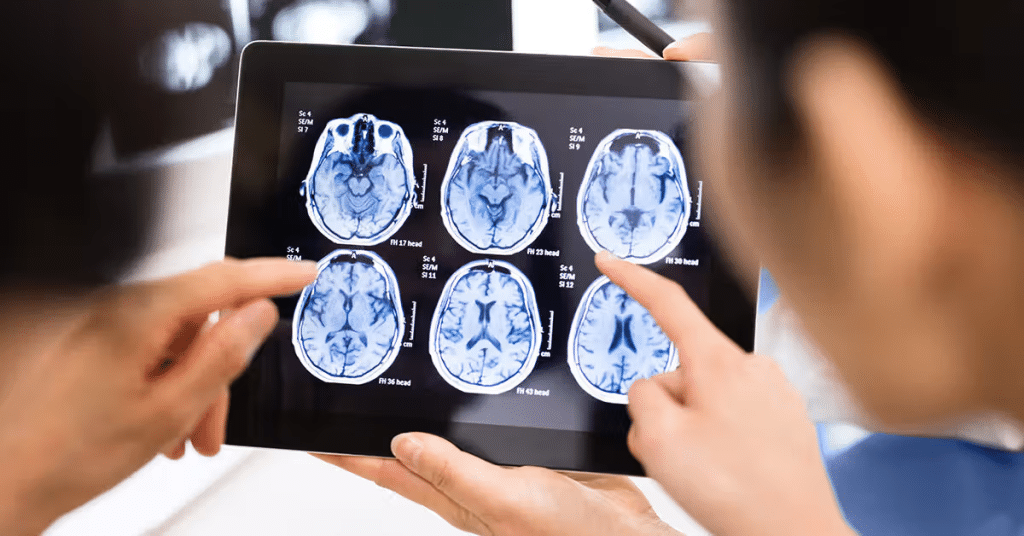
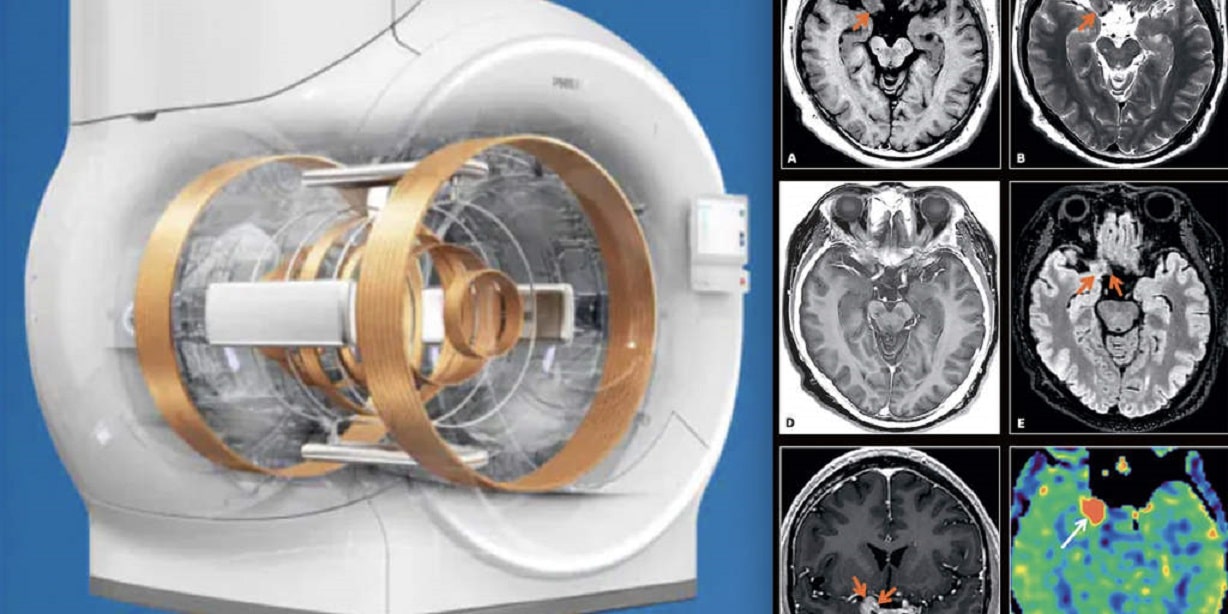
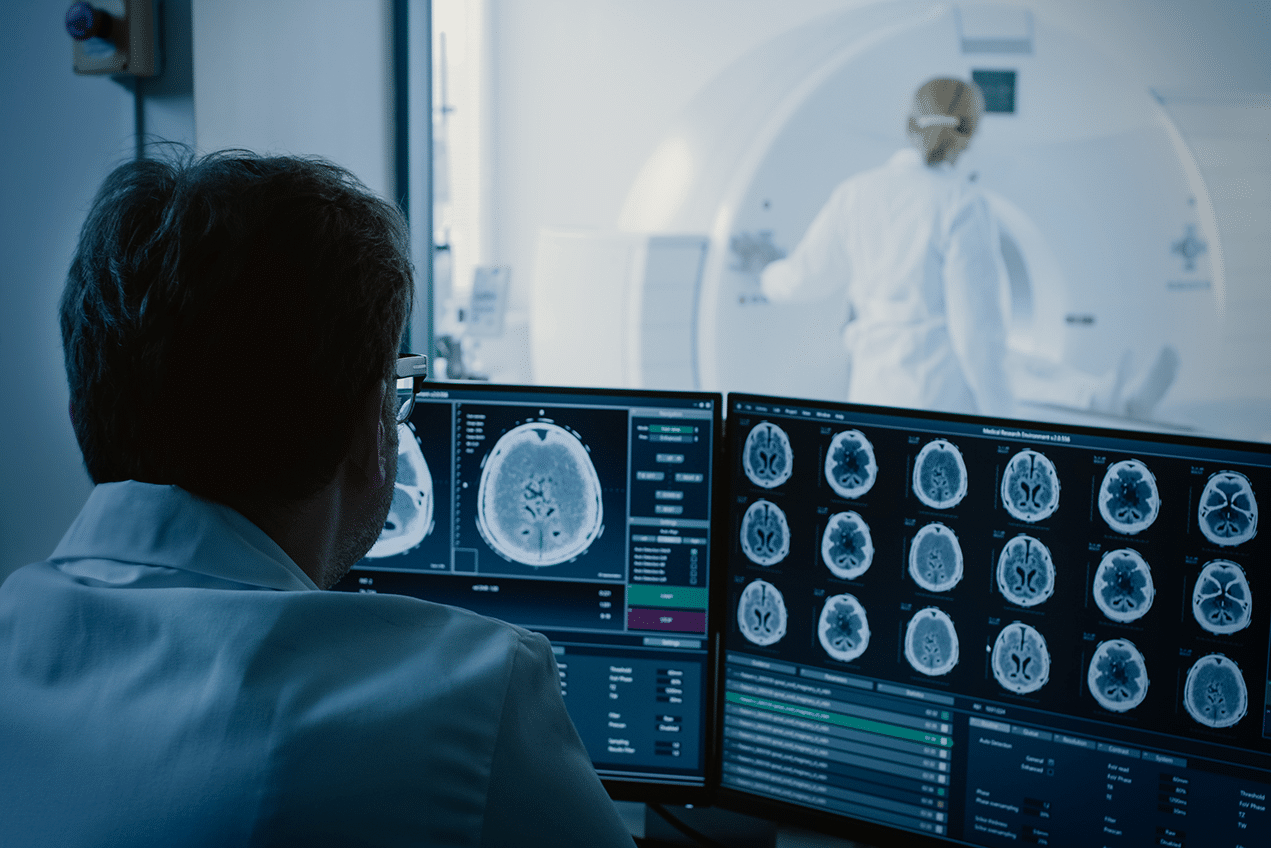
In neurology, AI enhances the analysis of brain images for conditions such as stroke, Alzheimer’s disease, and brain tumors. AI algorithms can detect subtle changes in brain tissue, allowing for early intervention and treatment. A notable example is the use of AI in diffusion-weighted imaging, a type of MRI, to quickly identify stroke-affected areas in the brain.
AI’s Impact on Diagnostic Accuracy
The integration of AI into medical imaging analysis has significantly improved diagnostic accuracy. It reduces human error and enhances early disease detection. This shift toward AI-enhanced diagnostic and imaging methods is reshaping the landscape of medical imaging technology and precision medicine. Below are the key impacts:
1. Improved Diagnosis of Various Medical Conditions
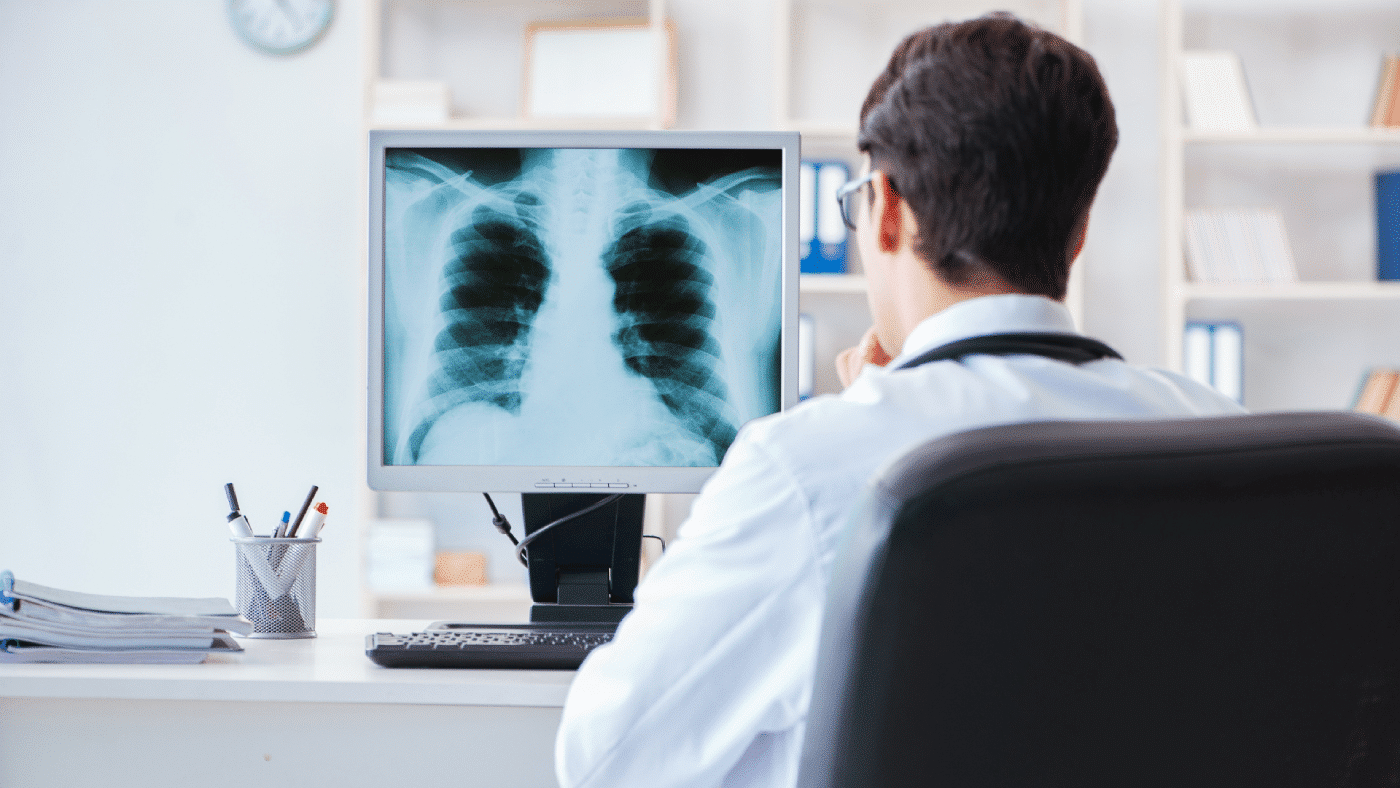
Thanks to its ability to learn from large datasets, AI algorithms have shown remarkable improvement in identifying and diagnosing medical conditions. For example, AI can match—or even surpass—the accuracy of human radiologists in detecting diseases like pneumonia in chest X-rays. This level of precision is especially critical in cases where early detection greatly influences treatment outcomes.
2. Reduction of Human Error
The second major advantage of AI in medical imaging is its consistency, which significantly reduces human error. Unlike human radiologists who may be affected by fatigue or subjective judgment, AI systems provide consistent analyses. AI support can reduce diagnostic errors in mammograms for breast cancer, thereby improving diagnostic accuracy.
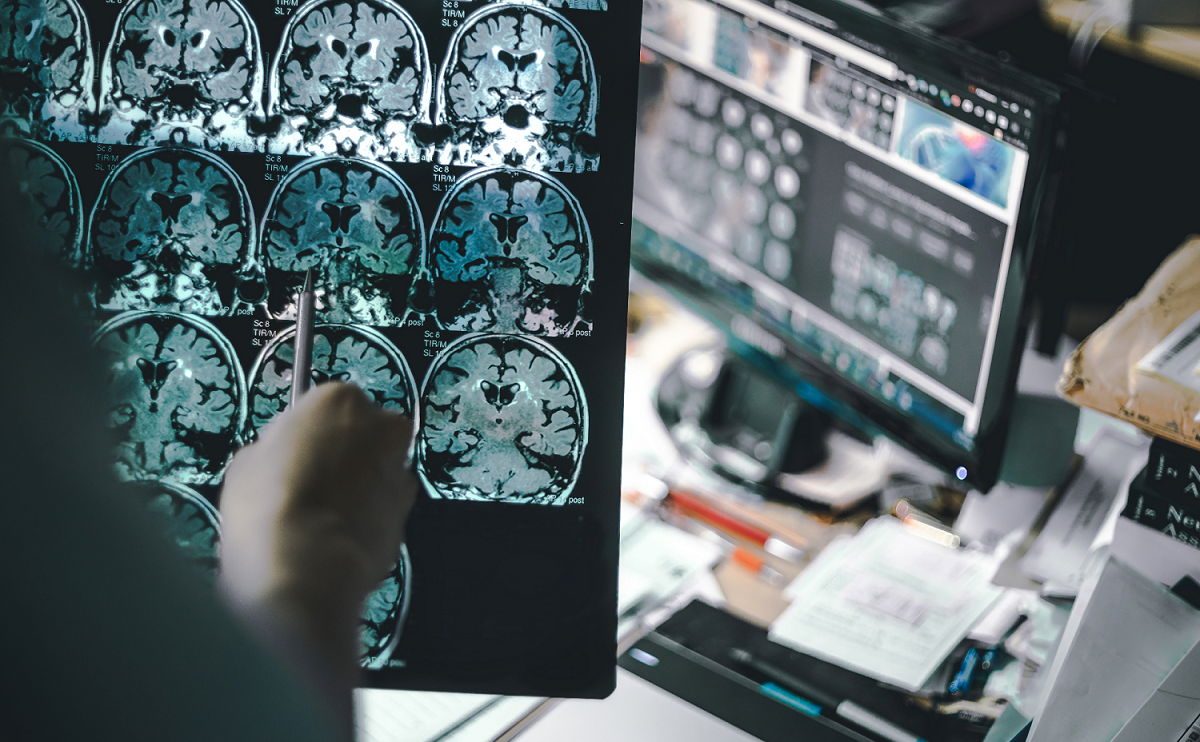
3. Early Disease Detection
Early disease detection is crucial for effective treatment, and AI is playing a vital role in this area. For example, AI has been instrumental in the early detection of diabetic retinopathy—a condition that can lead to blindness if left untreated. By analyzing retinal images, AI can detect this condition with high accuracy, often before any physical symptoms appear in the patient.
Challenges and Ethical Considerations
Despite the tremendous potential of artificial intelligence in the healthcare sector and medical imaging technologies, it still faces a number of challenges and concerns that slow down its widespread adoption. These challenges include:
1. Data Privacy
The first challenge affecting AI is the concern over data privacy. AI systems require access to large datasets of patient images, which raises significant concerns about confidentiality. Ensuring the security and privacy of this sensitive data is absolutely critical. Healthcare institutions must comply with strict data protection regulations, as safeguarding this information is essential.
2. High Costs
The cost of integrating AI into existing standard imaging technologies presents a major barrier to its adoption. Acquiring AI software, along with the necessary hardware upgrades, can be extremely expensive for many healthcare institutions—especially public ones.
3. Training Medical Staff
For AI to be successfully used in medical imaging, it also requires specialized training for healthcare professionals. Radiologists and technicians must be educated on how to interpret AI results and incorporate them into clinical decision-making processes.
4. Technical Challenges
Technical issues—such as data integration and algorithmic bias—pose significant challenges. Integrating AI into current health IT systems can be complex and demands seamless compatibility. To address this, AI systems must be trained on diverse and comprehensive datasets and undergo rigorous validation processes to ensure accuracy and fairness.
It is essential to ensure the transparency of AI-supported systems in decision-making processes and to clearly define accountability for the outcomes of those decisions. Regulatory frameworks must be established to guarantee the safe and effective use of AI in the medical field. These frameworks should address key issues such as:
- Validating algorithm reliability.
- Official certification and approval.
- Managing potential biases within the systems.
In conclusion, integrating AI into medical imaging is not merely a technical advancement, but a promising paradigm shift that redefines diagnosis and treatment planning. The positive impact of AI integration in imaging systems extends beyond patients, medical practitioners, and healthcare providers—it benefits anyone seeking a more efficient and error-free healthcare system.