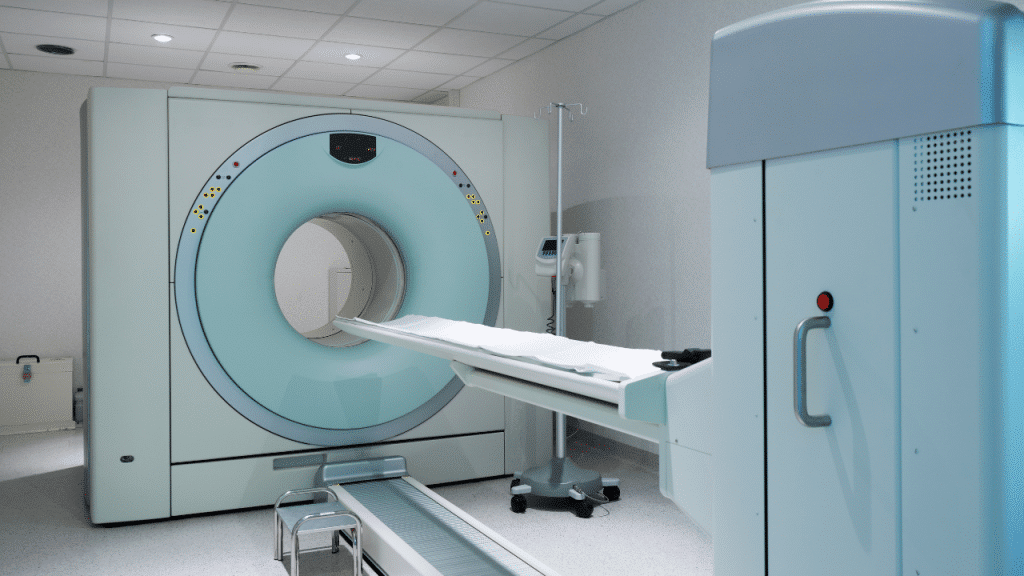
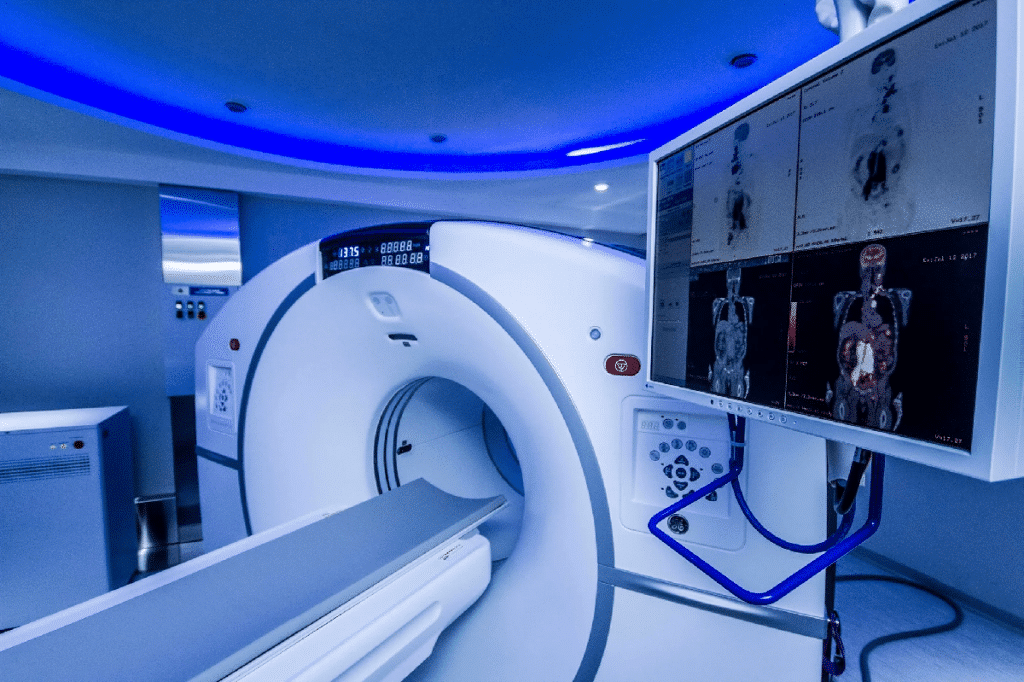
Artificial intelligence is defined as a branch of computer science aimed at designing systems and programs capable of simulating human cognitive abilities such as thinking, learning, and decision-making. One of its most prominent techniques in the medical field is known as machine learning in radiology, which relies on advanced algorithms to analyze big data and medical images. The applications of machine learning in radiology vary and include technologies such as deep learning and traditional machine learning, as well as the use of natural language processing (NLP) techniques that contribute to the preparation of medical reports and the analysis of electronic records. In this article, we will explore the applications of machine learning in medical imaging technologies.
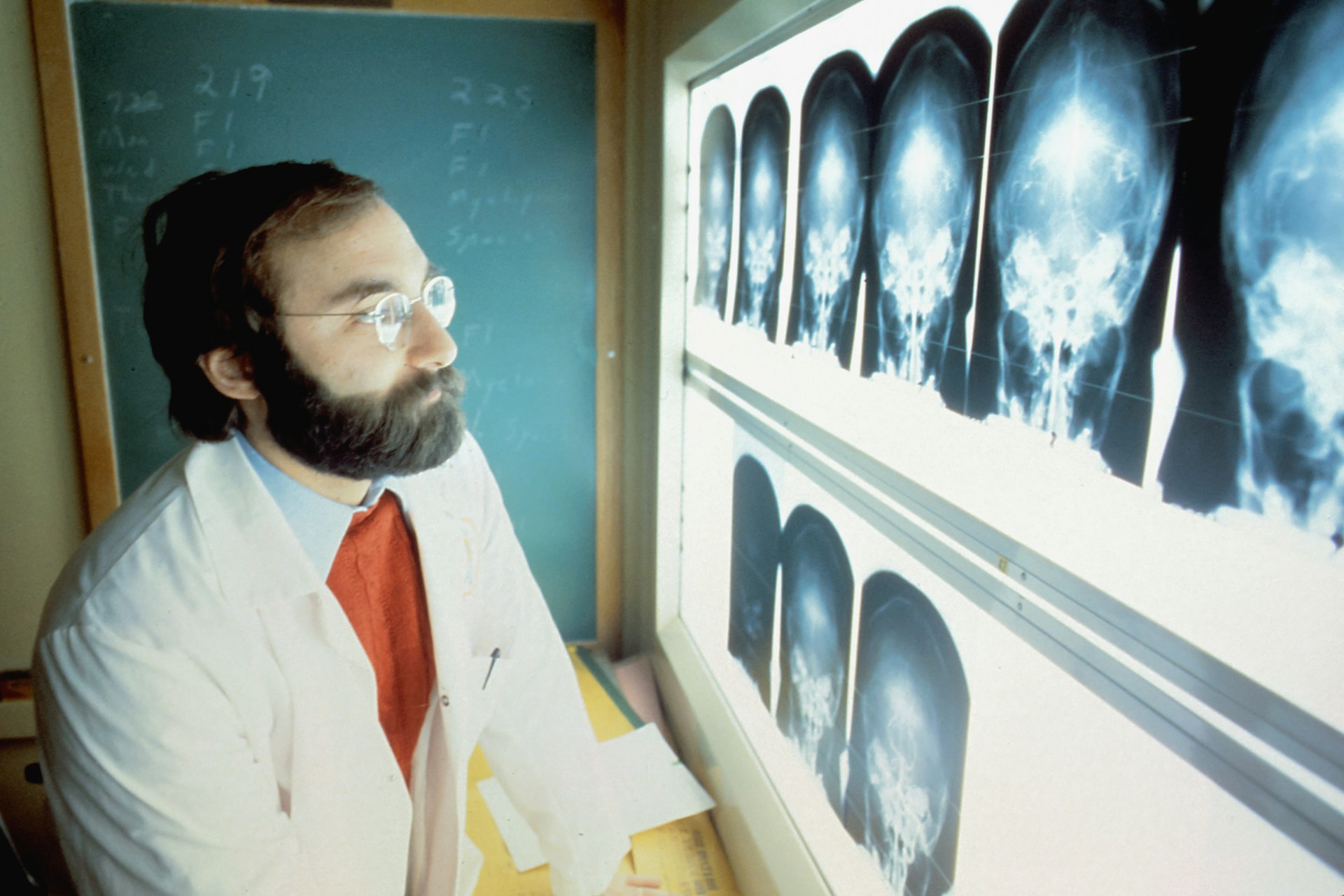
The journey of applying artificial intelligence in radiology began decades ago with the advent of computer-aided detection systems, initially used in fields like breast imaging for tumor diagnosis. With increasing computational power and advancements in data technologies, machine learning techniques in radiology have come to play a pivotal role in significantly improving diagnostic accuracy and reducing medical errors. This development helps save time for radiology specialists by allowing intelligent systems to handle routine tasks, thereby enabling doctors to focus on complex cases.
Applications of Machine Learning in Radiology
Machine learning in radiology has brought about radical transformations in many radiology specialties. Below are the most prominent applications along with case studies that illustrate its effective impact.
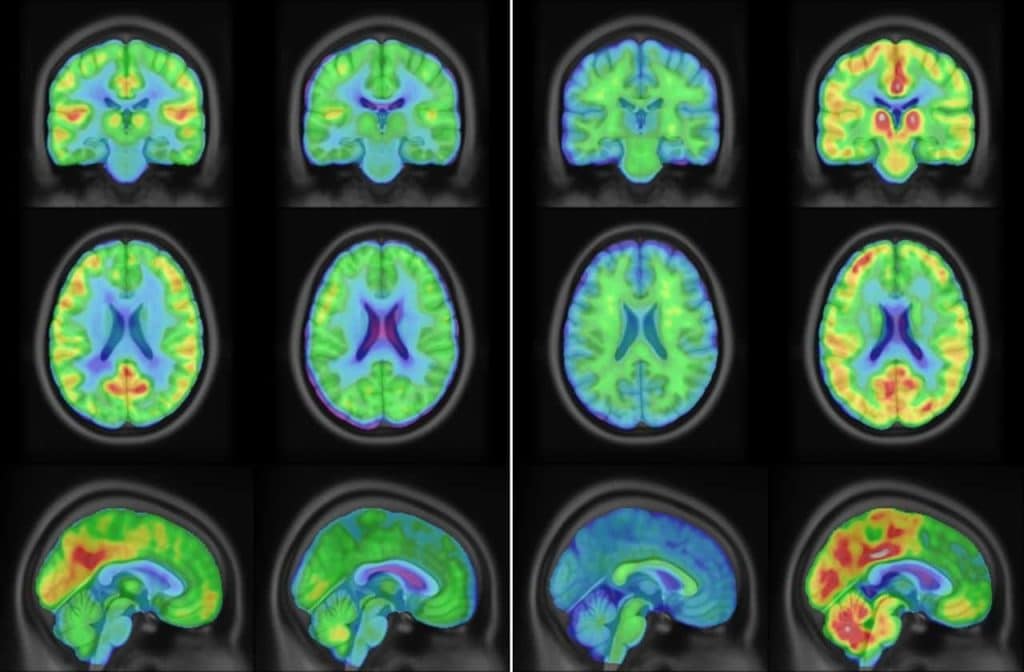
1. Neuroimaging
In the field of neuroimaging, machine learning is used to detect brain tumors and assess neurodegenerative diseases such as Alzheimer’s and Parkinson’s disease. Systems rely on deep learning algorithms to analyze magnetic resonance imaging (MRI) and computed tomography (CT) scans, discerning subtle differences between normal tissues and affected areas. For example, some studies have demonstrated that machine learning algorithms in radiology can distinguish between low-grade and high-grade tumors with greater accuracy than traditional methods, thereby contributing to improved treatment options and surgical planning.
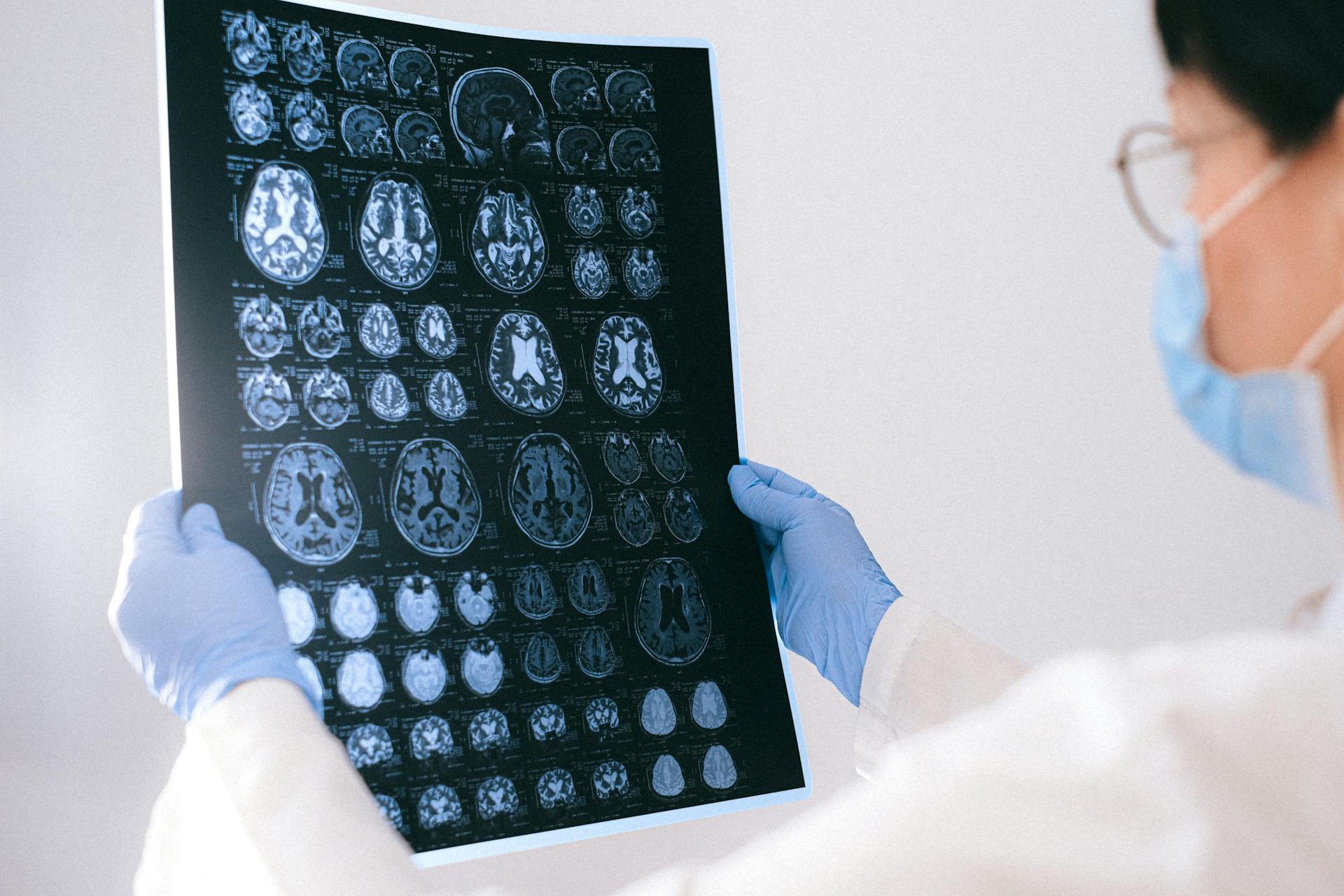
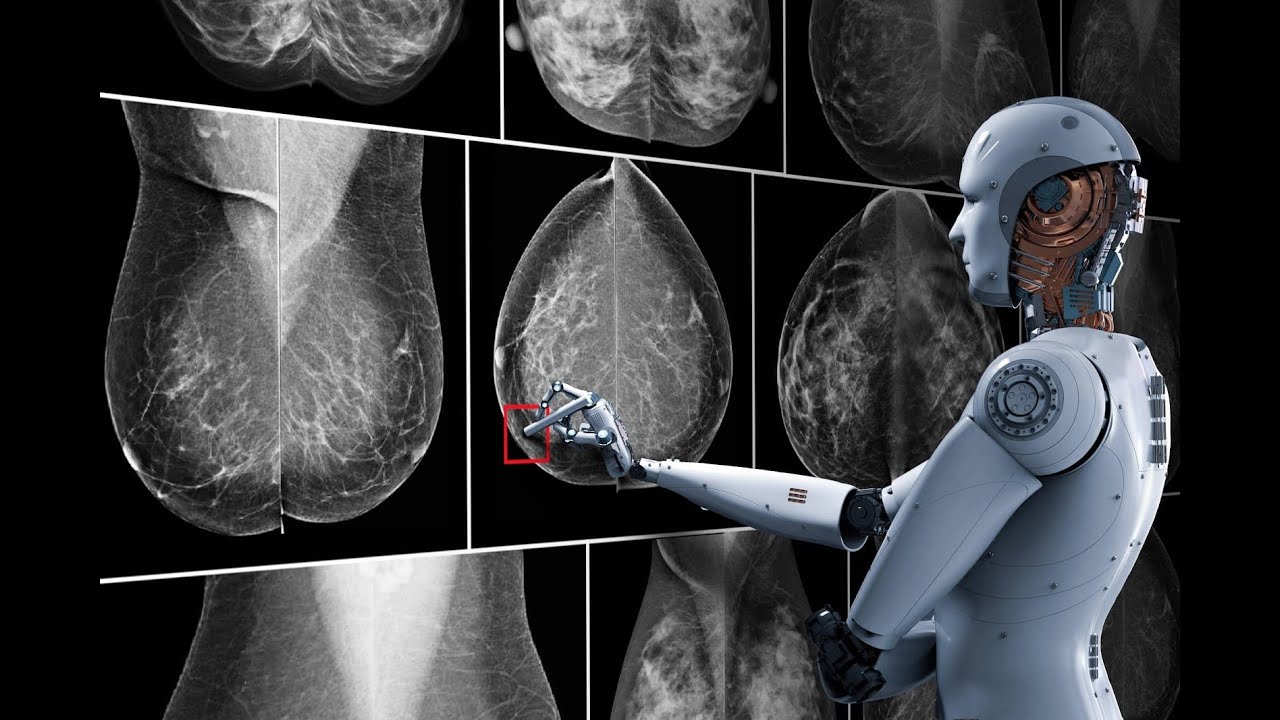
2. Mammogram Imaging
The diagnosis of breast cancer is one of the most prominent areas benefiting from machine learning in radiology. Deep learning techniques have contributed to the development of medical image analysis systems that examine mammogram images and identify tumors at early stages. Case studies indicate that these systems can achieve high accuracy rates in detecting tumors that might be overlooked during manual examinations, thus reducing diagnostic errors and improving patient survival rates.
3. Chest Imaging
Machine learning in radiology plays an important role in analyzing X-ray and chest images to diagnose conditions such as pneumonia, tuberculosis, and pulmonary fibrosis. Deep learning techniques are employed to analyze these images with extreme precision, enabling the system to differentiate between healthy tissues and those affected by disease. Moreover, these techniques are applied in emergency settings to quickly identify critical conditions like pneumothorax and fluid accumulations, thereby aiding in prompt, life-saving interventions.
4. Cardiac Imaging
Evaluating heart and vascular diseases is a vital area that has greatly benefited from machine learning in radiology. Artificial intelligence techniques are used to analyze chest CT scans and cardiac MRI to detect arterial blockages and assess heart function. Machine learning-supported models can analyze multidimensional data and integrate it with results from other tests to provide comprehensive and accurate diagnoses, thus contributing to improved treatment plans and reduced surgical risks.
5. Abdominal Imaging
In abdominal imaging, machine learning techniques are used to diagnose diseases of the liver, pancreas, and kidneys. Systems analyze CT images to detect masses or tumors and evaluate their characteristics, helping to differentiate between benign and malignant tumors. Studies show that these techniques can reduce diagnosis time and increase accuracy, allowing doctors to intervene early and provide appropriate treatment.
6. Musculoskeletal Imaging
Applications in musculoskeletal imaging include diagnosing fractures, assessing joint and bone diseases, and identifying cases of arthritis. Algorithms analyze X-ray and MRI scans to accurately detect abnormalities in the skeletal structure. This enhanced analysis improves diagnostic accuracy and offers customized treatment recommendations, ultimately contributing to an improved quality of life for patients.
7. Nuclear Medicine Imaging
In nuclear medicine, machine learning in radiology has improved the quality of images obtained through techniques such as PET and SPECT. AI-based denoising and filtering techniques are used to reduce noise and enhance image precision, which contributes to the early detection of tumors and cardiac and neurological diseases. Additionally, these techniques help reduce the required radiation doses without compromising diagnostic quality.
8. Interventional Radiology
Machine learning is applied in interventional procedures to enhance the accuracy of surgical interventions and reduce risks. Algorithms provide immediate support during surgery by analyzing images and precisely identifying target tissues, which aids in planning procedures and improving patient outcomes. Intelligent systems are also used to monitor interventions and offer real-time recommendations to physicians during operations.
Enhancing Patient Care Through Machine Learning in Radiology
The benefits of machine learning in radiology extend beyond diagnosis to include significant improvements in patient care:
- Support for Medical Decision-Making: Intelligent systems help analyze clinical data and medical images to provide precise treatment recommendations, reducing medical errors and bolstering physicians’ confidence in their diagnoses.
- Improved Workflow: Machine learning techniques help organize appointment schedules and prioritize examinations, thereby enhancing the efficiency of medical departments and reducing waiting times.
- Reduced Radiation Exposure: By employing image enhancement techniques, the need for repeat examinations is minimized and radiation doses for patients are reduced without affecting diagnostic quality.
- Early Diagnosis and Personalized Treatment: Intelligent systems enable the early detection of tumors and chronic diseases, allowing for personalized treatment plans tailored to each patient’s health condition.
Challenges and Future Prospects
Despite the significant achievements of machine learning in radiology, several challenges remain:
1- Data Quality and Diversity
Training machine learning algorithms requires large and varied datasets. However, issues of privacy and data confidentiality pose major obstacles to data collection. Techniques like federated learning may offer promising solutions to progress without compromising patient privacy.
2- Integration and Interoperability
Machine learning systems must operate seamlessly with existing medical systems such as Radiology Information Systems (RIS) and Picture Archiving and Communication Systems (PACS). Achieving interoperability and integration with diverse software systems represents a significant challenge.
3- Transparency and Explainability
A major challenge is the “black box” phenomenon, where it can be difficult to understand how algorithms make decisions. Developing explainable AI systems is essential to build trust between physicians and intelligent systems and ensure their safe and effective use in clinical environments.
4- Quality Assurance and Regulatory Approval
Machine learning systems must undergo rigorous testing to ensure their accuracy and safety before clinical use. Regulatory bodies like the FDA require strict standards to confirm that these systems are both safe and effective. Continuous research, development, and collaboration between developers and medical institutions are vital to achieving this.
5- Ethical and Privacy Concerns
Issues regarding data privacy and the handling of sensitive information pose significant ethical challenges. Medical institutions must adhere to the highest standards of data protection and ensure that the use of machine learning does not introduce biases that negatively impact certain patient groups. Clear policies for data management and the handling of diagnostic results are essential to maintain fairness and transparency throughout the diagnostic process.
Case Studies and Practical Applications
Multiple studies have demonstrated the tangible benefits of machine learning in radiology in real clinical settings. For example, the use of deep learning to analyze mammogram images has improved early detection of breast tumors and reduced mortality. In emergency settings, intelligent systems have expedited the diagnosis of pneumonia and pneumothorax via X-ray image analysis, enabling prompt intervention. Additionally, machine learning techniques have precisely analyzed cardiac MRI scans to identify heart failure and devise personalized treatment plans, while in abdominal imaging, intelligent models have differentiated between benign and malignant liver tumors, facilitating targeted treatments and reducing the need for complex surgeries.
Machine learning in radiology represents a qualitative leap in medical diagnostics, offering advanced analytical tools that enable early disease detection and enhanced patient care. Its applications span all radiology specialties—from neuroimaging to nuclear and interventional radiology—improving diagnostic accuracy and reducing medical errors. Despite challenges related to data diversity, interoperability, and transparency, ongoing research and development remain key to overcoming obstacles and achieving optimal integration between intelligent systems and clinical diagnosis.
The success of machine learning in radiology depends not only on technological advancements but also on close collaboration among physicians, researchers, developers, and policymakers. Such cooperation is essential for developing safe, transparent, and effective systems that ensure high-quality healthcare and improved patient outcomes.
As advancements continue, experts expect the future of machine learning in radiology to witness further innovations that will revolutionize the methods of diagnosing and treating diseases. This underscores the necessity of investing in education, training, and the development of digital infrastructure within medical institutions. These efforts will not only improve diagnosis and treatment but also open new horizons for scientific research and clinical applications, ultimately enhancing healthcare quality worldwide.
The HSI Center welcomes medical engineers passionate about exploring the world of medical imaging and its advanced technologies by offering unique training courses. Through these courses, participants will delve deep into both theoretical and practical knowledge, acquiring the skills needed to actively contribute to progress in this rapidly evolving field. Join us on this inspiring educational journey and become part of the future of medical imaging.