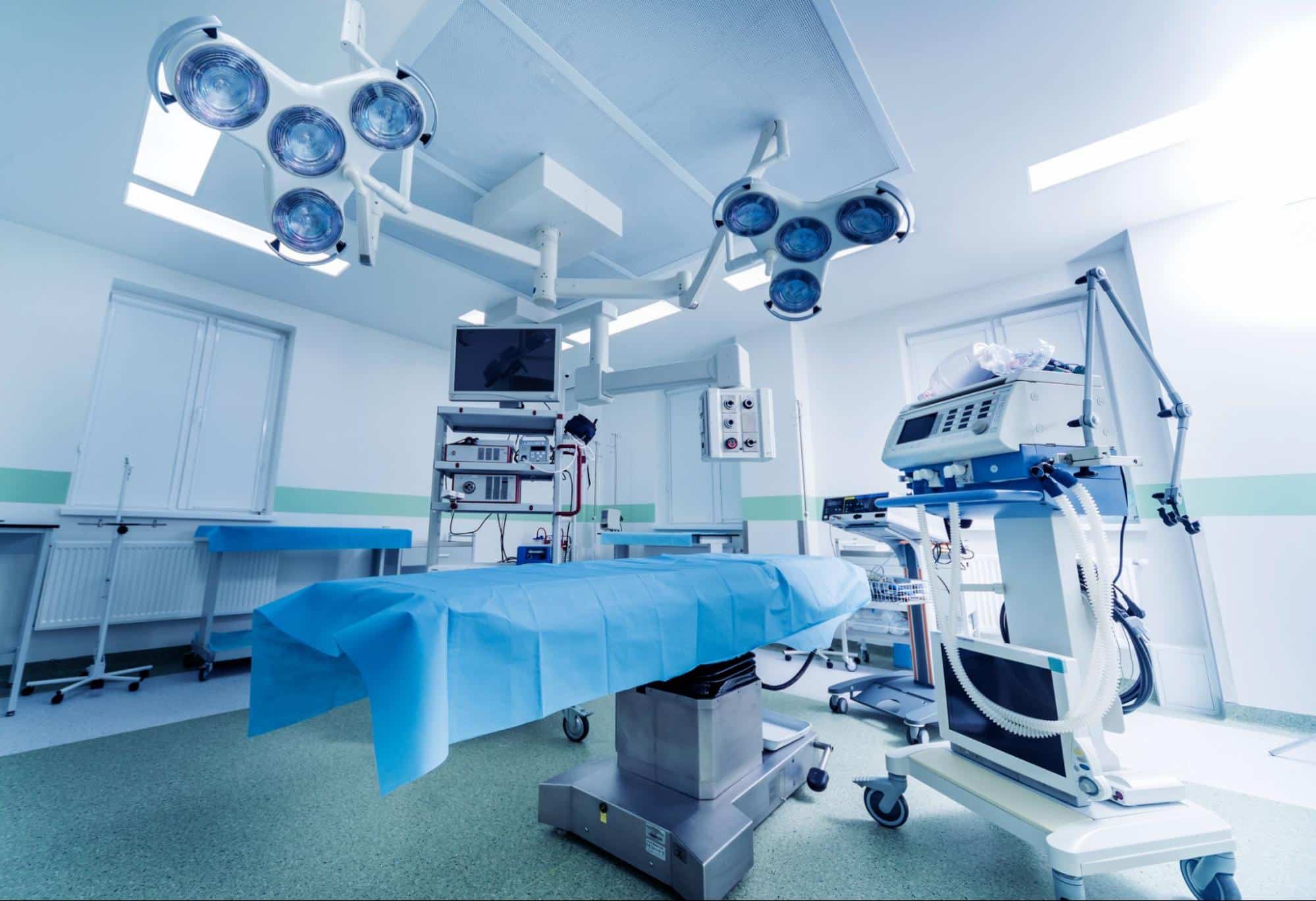
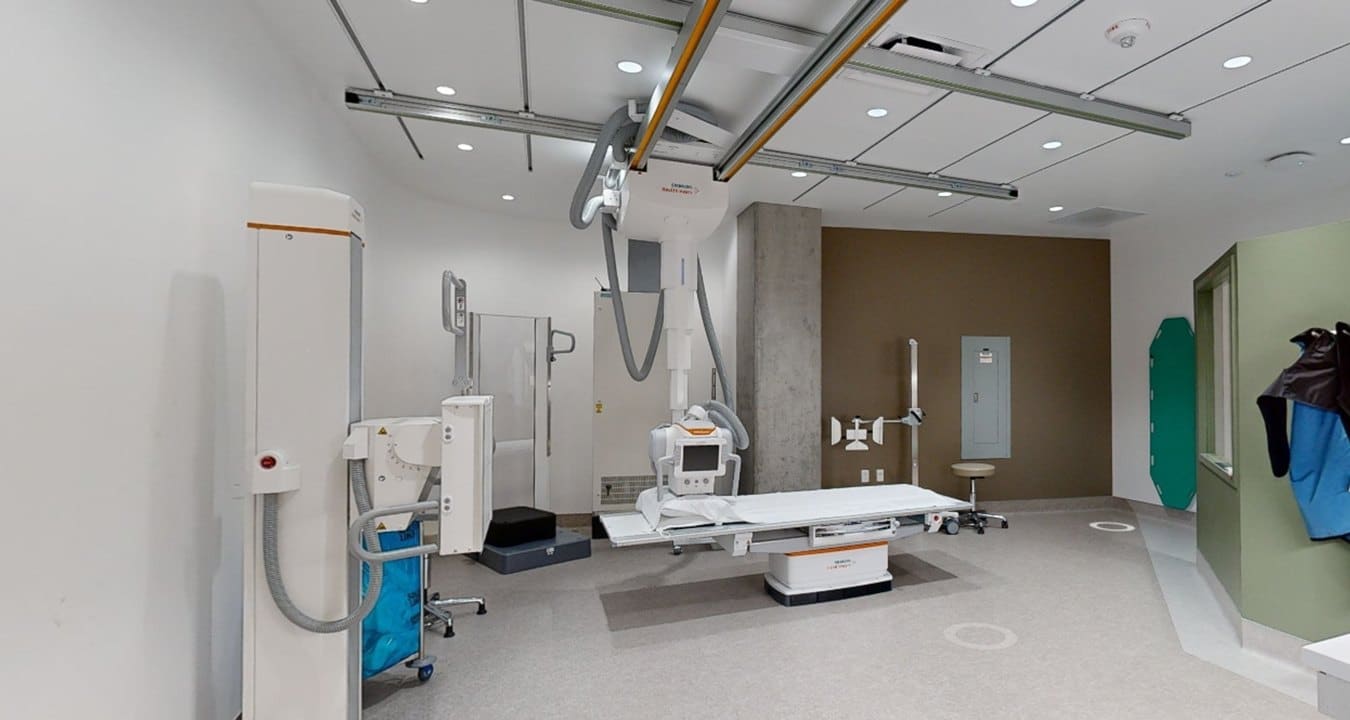
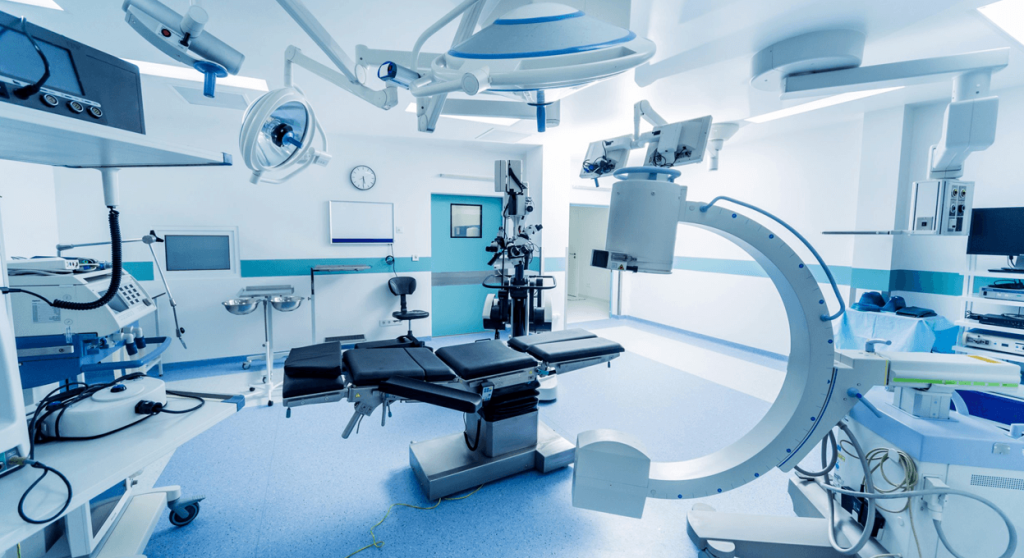
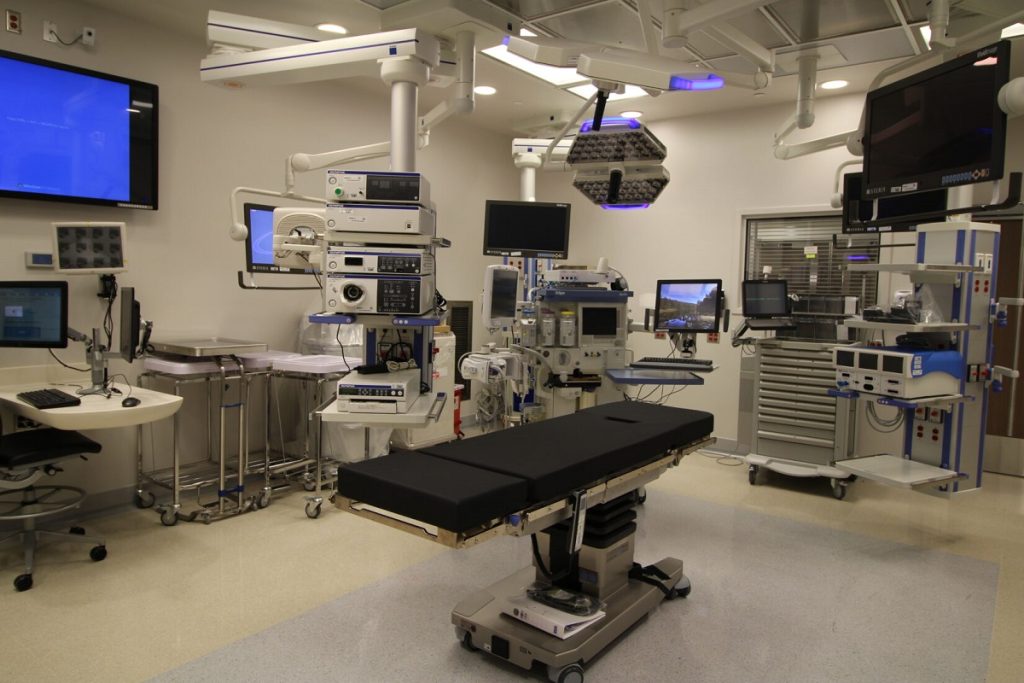
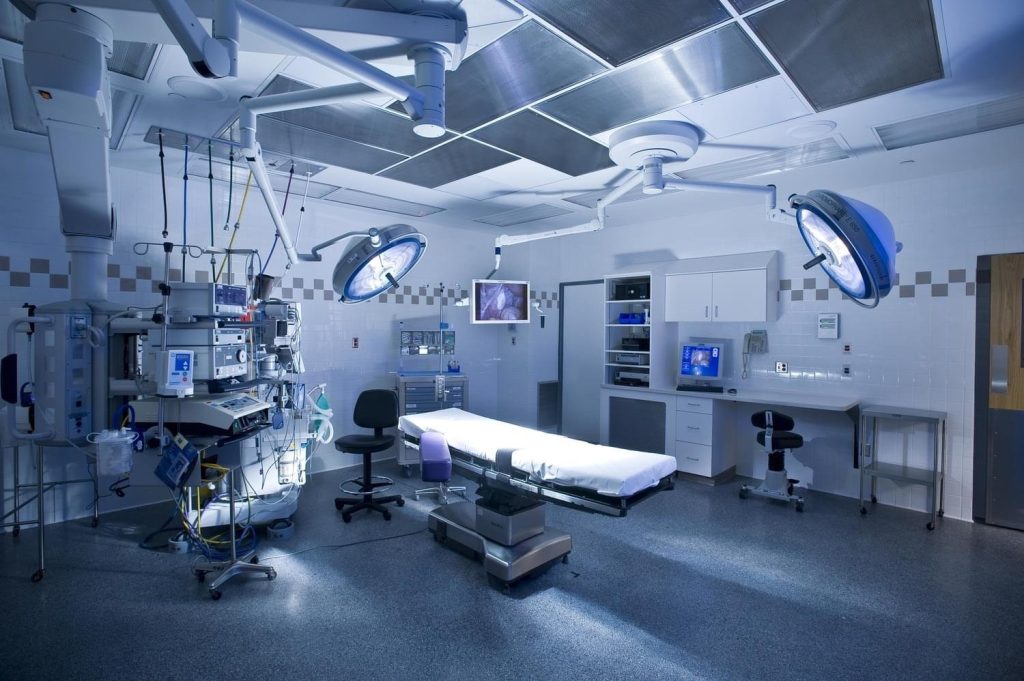
Designing a Highly Efficient Operating Room properly is a critical factor in enabling hospitals to have efficient operating rooms that can adapt to ongoing innovations in healthcare and better safeguard patient health. Given the significant role that operating rooms play in saving patients’ lives, attention must be paid to the environment where surgeries are performed, regardless of their type.
Considering the current social and economic situation in the healthcare sector, hospitals must optimize their resources more than ever. Efficiency, performance, and innovation must integrate to reduce healthcare spending without compromising patient-centered care.
Operating Room Zoning
Modern hospital operating rooms are committed to creating distinct and differentiated areas within the surgical zone. The primary goal is to prevent potential contamination and infection of patients, as the major source of postoperative wound infections stems from improper handling of shared spaces between medical staff and patients.
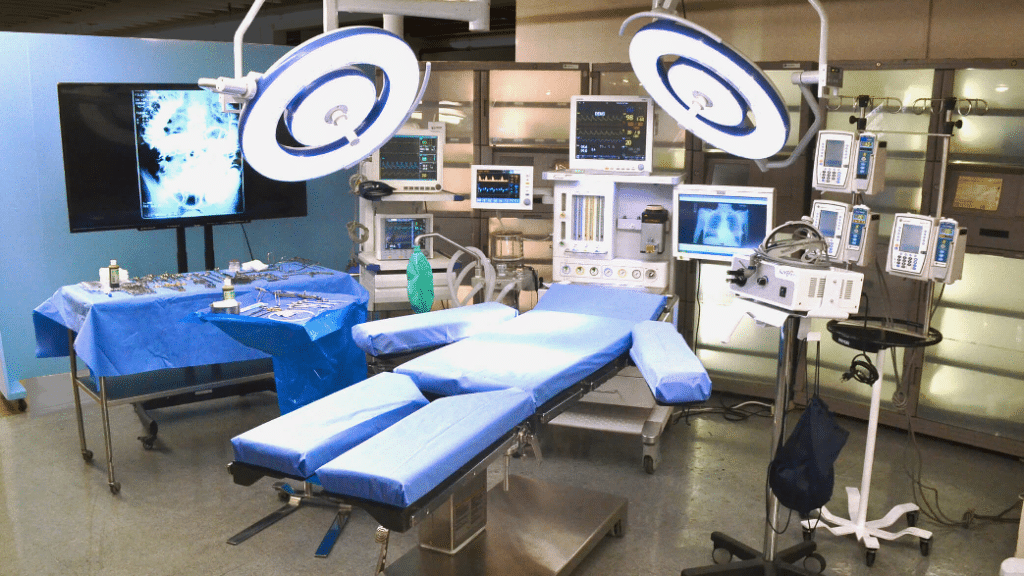
Therefore, dividing the structure of the operating room into three different zones reduces and eliminates sources of contamination:
- Black Zone: This is the initial isolation area upon entering the operating room. Here, the patient is prepared with appropriate surgical attire. It is the area where patients are received, with semi-restricted access, and includes administration and changing rooms.
- Gray Zone: The clean area where individuals present must wear sterile masks and caps. Patient companions and medical staff are allowed in this area. It contains the pharmacy, storage for surgical instruments, and access areas to operating rooms.
- White Zone: An area with maximum restrictions, where the operating room and sterile access corridors are located. In this zone, doors must remain closed at all times.
Operating Room Design
In improving hospital and healthcare center facilities, surgical intervention areas, or operating rooms, are among the most critical areas to consider. One of the key steps to enhance them is innovation in operating room design, taking into account essential design considerations, which we will discuss in this article.
When designing surgical rooms, the location and flow of patients, staff, and materials should be considered as the three main elements during the design stages of the operating room. Additionally, isolating it from the main traffic in the hospital, having direct access to recovery units, communication with pharmacy units, radiology, and emergency entrances are important. The surgical area should also have good lighting focused on the surgical table and provide proper air conditioning.
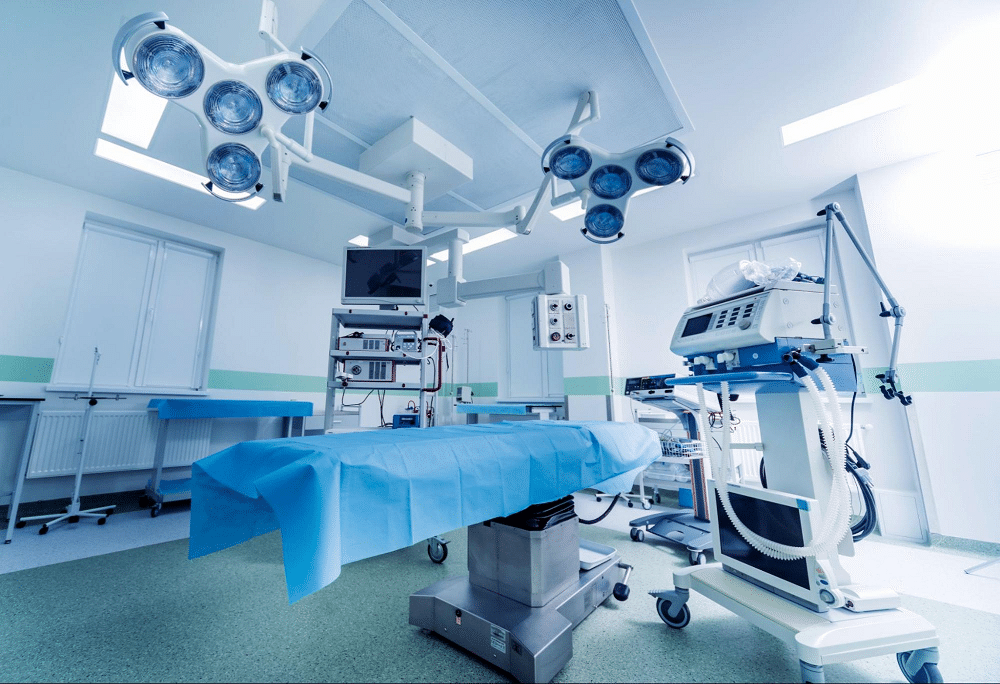
Consideration should be given to providing a sterile protection area, changing rooms for all medical staff, rooms for administrative staff, a cleaning room, and equipment storage.
It should also include several sub-areas such as:
- Preoperative registration or reception area.
- Preparation area.
- Anesthesia room.
- Post-anesthesia care units.
- Facilities for cleaning staff.
Basic Requirements When Designing Operating Rooms
- Double Circulation Design: Operating areas should be designed with a double circulation system to ensure proper workflow protocols.
- Separation of the Clean Area: The clean area in the operating room should be defined and separated from other areas.
- Proper Air System: An appropriate air system is essential, and positive pressure gradients must be maintained.
- Surgical Handwashing Area: A surgical handwashing area with a sensor-operated sink should be provided.
- Size of Surgical Rooms: Operating rooms should have a minimum area of 25 square meters.
- Floor Materials: The floor should be made of semi-conductive materials connected to the ground, with attention to electrical installations and their maintenance.
- Doors: Doors should be tightly sealed or sliding and operate automatically.
- Surface Coverings: Walls, ceilings, and floors should be covered with smooth materials, free from cracks or openings.
- Avoiding Gaps: Gaps such as corners and crevices should be avoided.
- Emergency Communication System: Rooms should have an optimal communication system for emergencies, including telephones, intercoms, buzzers, emergency lights, and a computer area.
- Lighting: Lighting should be appropriate, preferably using LED lights.
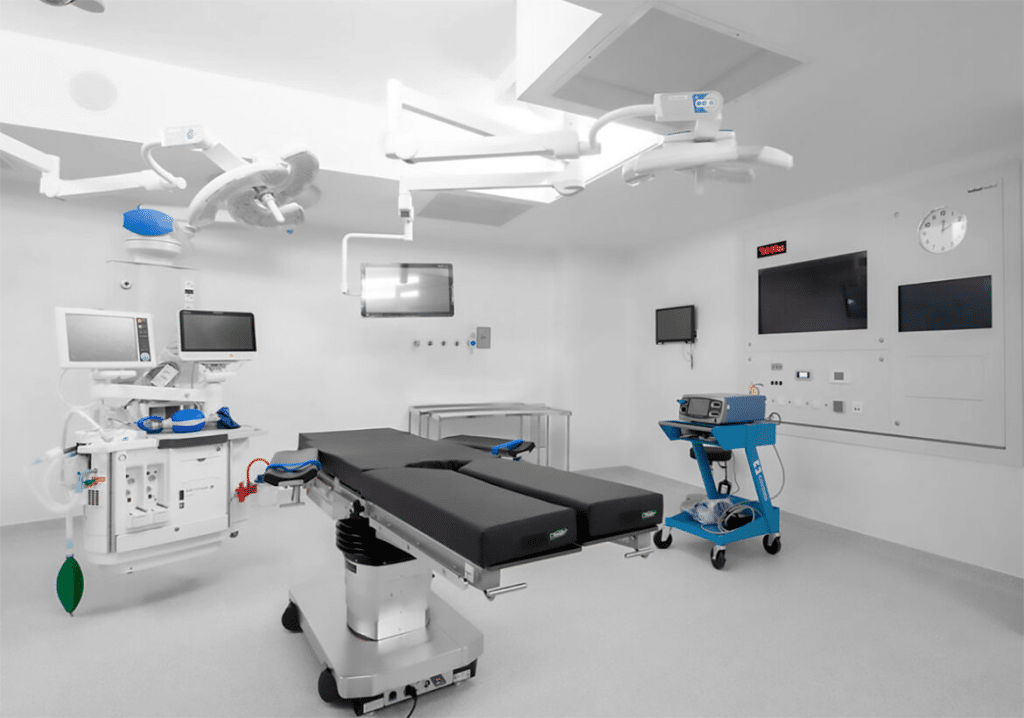
Key Considerations When Designing Operating Rooms
Designing operating rooms is a critical task that combines functionality, safety, and comfort. The environment where surgical procedures are performed must be meticulously planned, as its design plays a significant role in the success of surgical operations. Therefore, it is essential to consider several factors to ensure that these spaces meet the needs of healthcare professionals and provide the best possible outcomes for patients.
1- Attention to Operating Room Layout
The design should facilitate the smooth flow of personnel and equipment, minimizing the risk of contamination during procedures. An effective layout typically includes designated areas for surgical instruments, a sterile zone where the surgical team operates, and clear pathways for easy access to essential medical supplies. Additionally, integrating advanced technology, such as surgical lighting and imaging systems, should be seamless to enhance the room’s functionality.
2- Infection Control Measures
Preventing infections is paramount when designing an operating room, as these environments can be breeding grounds for bacteria and viruses. It’s crucial to implement measures to prevent the spread of infections. One advantage of maintaining a lower temperature in the operating room is that microorganisms grow more slowly at reduced temperatures. Key considerations for infection control include:
- Using non-porous, easy-to-clean materials in the construction of the operating room.
- Designing walls, floors, and ceilings to minimize dust accumulation and facilitate maintenance.
- Carefully planning the ventilation system to ensure proper air circulation and filtration, thereby reducing the risk of airborne contaminants.
3- Adequate Lighting
Sufficient lighting is essential for the surgical team to have clear visibility and perform precise procedures. Utilizing a combination of ambient lighting and task lighting can provide the necessary illumination.
4- Facilitating Movement
Ergonomics cannot be overlooked in operating room design. The layout should promote comfort and ease of movement for the surgical team. Factors such as the height of surfaces, accessibility of equipment, and the positioning of monitors can significantly impact the efficiency and effectiveness of work in the operating room.
5- Integrating Technology into Operating Room Design
Advanced surgical equipment and integrated technology can enhance surgical precision and improve communication among the surgical team. Ensuring that all technological components are seamlessly incorporated into the operating room design can streamline workflow.
In conclusion, designing operating rooms is a multifaceted process that requires careful consideration of various factors, including layout, infection control, lighting, ergonomics, technology integration, and collaboration with healthcare professionals. By focusing on these elements, designers can create operating rooms that support the surgical team in delivering high-quality patient care and achieving successful surgical outcomes.
At HSI, we offer specialized courses to guide and assist healthcare professionals, including effective strategies for designing operating rooms that serve patients and enhance overall medical services.
Source: All the Keys to the Correct Design of an Operating Theatre