Medical equipment is considered the cornerstone of delivering effective and high-quality healthcare within hospitals. It plays a pivotal role in diagnosing diseases, treating patients, and monitoring their conditions. With rapid technological advancements, choosing the right medical equipment has become a complex task that requires a careful study of several factors to ensure the best patient outcomes and improve operational efficiency within the hospital. Making informed decisions regarding the selection of medical equipment directly impacts the quality of healthcare services provided, patient safety, and the economic viability of the medical institution.
With a wide range of options available, those responsible for choosing medical equipment may find themselves facing a significant challenge. The vast diversity in device types, specifications, technologies, and manufacturers necessitates the existence of a comprehensive guide that assists in making the right decisions. This article aims to serve as that guide by discussing the fundamental criteria to consider when selecting medical equipment for your hospital, with a focus on patient needs, safety, and ensuring accuracy and reliability.
Choosing Medical Equipment
Essential Criteria to Consider When Choosing Medical Equipment
The process of choosing the right medical equipment requires a careful evaluation of several essential criteria to ensure that the health needs of patients are met and the hospital’s objectives are achieved.
Patient Needs and Safety
The first and most important factor to consider when choosing medical equipment is the specific needs of patients and their safety. The hospital must accurately determine the demographic profile of the patients it serves, including their average ages, common health conditions, and the medical specialties provided. For instance, if the hospital serves a large number of children, it is crucial to select medical equipment specifically designed to meet their needs, taking into account their small sizes and unique physiological requirements. Similarly, the medical furniture should be comfortable and practical to accommodate patients of different ages and categories.
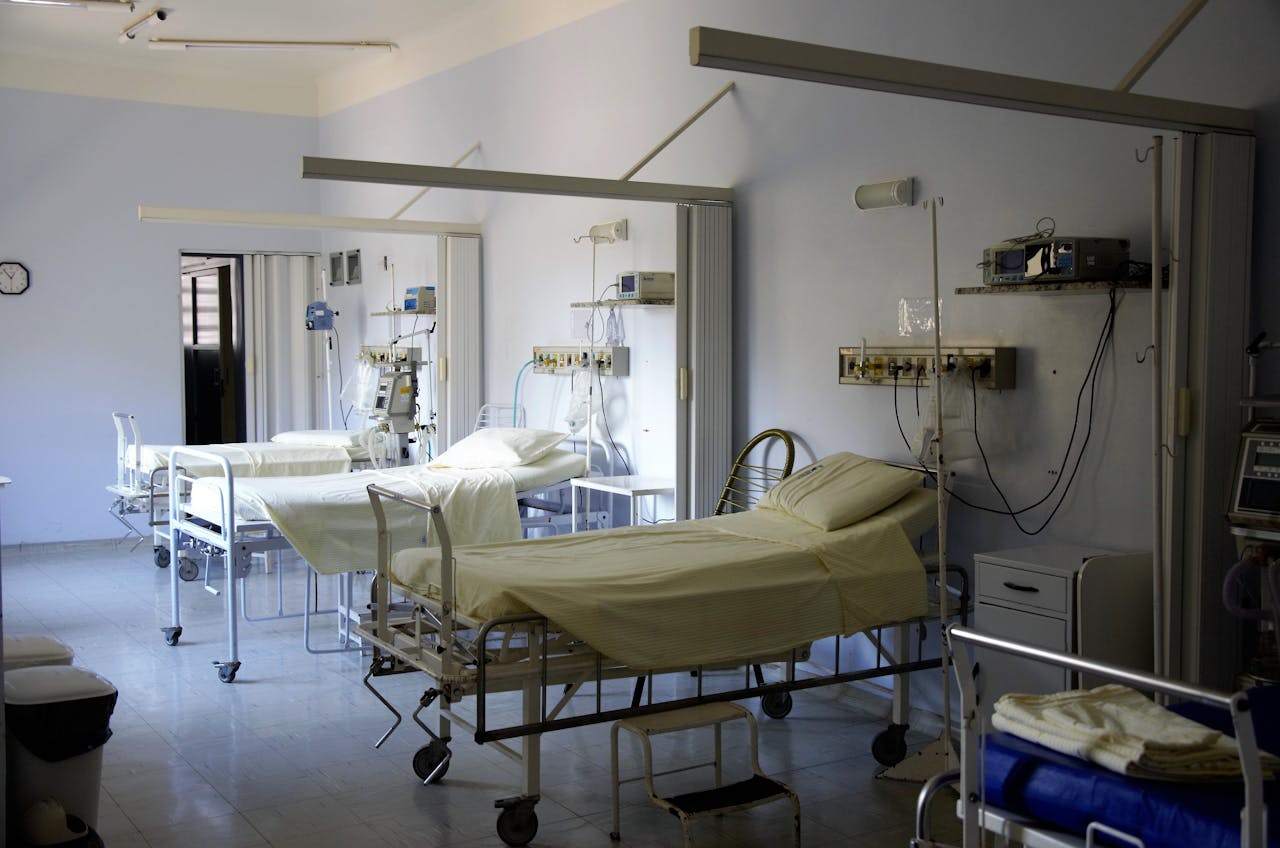
Ensuring patient safety is of utmost importance. Medical equipment should be chosen with built-in safety features, such as alarm systems that alert the medical staff in case of any malfunction or abnormal readings. The equipment should also include automatic shut-off mechanisms to reduce potential risks and infection control procedures to prevent the spread of diseases. For example, when selecting medical equipment such as vital signs monitors, features such as continuous monitoring, alerts for abnormal readings, and secure data transmission to prevent unauthorized access must be considered.
Another critical aspect is compatibility with existing healthcare systems to ensure smooth integration and efficient data management. It is essential to ensure that the new equipment can be easily integrated with the electronic health record (EHR) system and other medical devices used within the hospital. This integration helps streamline workflows, improve data accuracy, and enhance overall clinical efficiency.
Accuracy and Reliability
Accuracy and reliability are key characteristics when choosing medical equipment. Inaccurate or unreliable devices can lead to misdiagnosis and ineffective treatment, thereby endangering patient health. To ensure accuracy, it is necessary to select medical equipment that has undergone rigorous testing and obtained the necessary regulatory approvals. Look for quality certifications such as ISO 13485, which pertains to quality management systems in the medical device industry and ensures that manufacturers adhere to global safety and quality standards.
It is also important to research the reputation of the manufacturer and evaluate its performance in real-world environments. Obtaining feedback from other healthcare professionals who have used the equipment can provide valuable insights into its performance under clinical conditions. Additionally, the availability of support and maintenance services should be taken into account to ensure that any issues can be promptly resolved, minimizing downtime.
Economic Viability and Long-Term Value
While the initial cost of medical equipment is an important factor, it is equally crucial to assess the long-term value and economic viability of the selection. A cost-benefit analysis should be conducted to determine whether the benefits of the equipment outweigh its expenses in the long run. Factors such as durability, warranty coverage, and the potential for future upgrades or modifications should be considered.
Investing in high-quality equipment that offers long-term value can lead to cost savings and improved patient outcomes over time. For example, choosing medical equipment with advanced features and connectivity capabilities can enhance efficiency and data management, resulting in better clinical decision-making and a reduction in manual paperwork. Additionally, the availability of spare parts, as well as maintenance and repair costs, should be considered. Often, choosing medical equipment from reputable manufacturers ensures a reliable supply of spare parts and access to a network of authorized service centers, which minimizes downtime and extends the lifespan of the equipment.
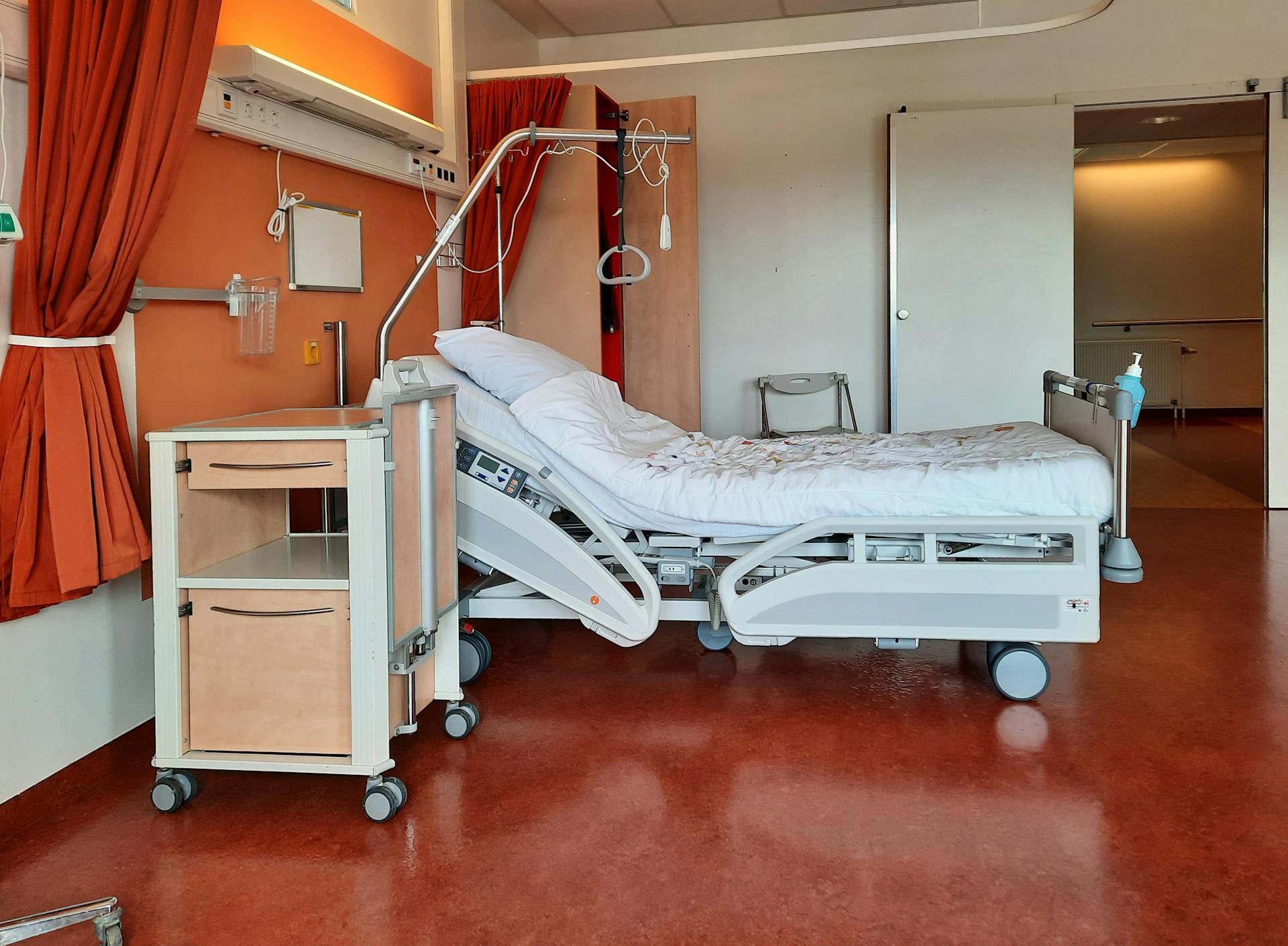
Ensuring Quality and Safety in Choosing Medical Equipment
To guarantee that the selected medical equipment meets the highest standards of quality and safety, hospitals must follow several key steps.
Verifying Quality Certifications and Industry Standards:
Hospitals should meticulously check quality certifications and industry standards when choosing medical equipment. The ISO 13485 certification is one of the most important in this field, as it indicates that the manufacturer has a quality management system that meets the requirements for medical devices. Additionally, it is essential to ensure that the equipment has obtained the necessary regulatory approvals from both local and international authorities, such as the U.S. Food and Drug Administration (FDA) or the CE mark in Europe.
Conducting a Comprehensive Risk Assessment for the Equipment:
The process of choosing medical equipment should include a thorough risk assessment of the potential hazards associated with using the equipment. It is important to identify and evaluate the risks that patients and healthcare providers may face and to implement measures to mitigate these risks. For example, ensuring that the equipment is user-friendly can reduce the likelihood of user errors, and selecting devices made of biocompatible materials can minimize the risk of adverse reactions in patients. Furthermore, appropriate protocols for cleaning and sterilizing the equipment should be established to prevent the spread of infections.
Impact on Hospital Efficiency and Patient Outcomes
The proper selection of medical equipment has a significant impact on the efficiency of hospital operations and patient outcomes.
Accurate and Timely Diagnosis of Diseases:
Modern and advanced medical equipment contributes to the precise and prompt diagnosis of diseases. Advanced imaging devices such as Magnetic Resonance Imaging (MRI), Computed Tomography (CT) scans, and Electrocardiogram (ECG) machines provide detailed images and accurate information that help physicians detect diseases at early stages and precisely determine their characteristics. Early diagnosis can lead to more effective treatment and increase the chances of full recovery.

Improved Treatment Outcomes:
The impact of choosing the right medical equipment extends to improving the treatment outcomes of diseases. Advanced medical devices, such as ventilators, blood pumps, artificial heart devices, and minimally invasive surgical instruments, provide effective tools for delivering appropriate treatment for a variety of conditions. These technologies help accelerate the recovery process, reduce the risk of complications, and enhance the overall quality of life for patients.
Reducing the Risk of Injuries and Complications:
Selecting the appropriate medical equipment can significantly reduce the risk of injuries and complications among patients. Modern patient monitoring systems offer continuous surveillance of vital signs and provide timely alerts in case of any abnormal changes, allowing the medical staff to intervene swiftly. Moreover, the use of minimally invasive surgical tools reduces the size of incisions, shortens recovery periods, and minimizes the risk of infections and other complications associated with traditional surgery.
Enhancing Operational Efficiency in Hospitals:
The adoption of modern medical equipment leads to improved operational efficiency within hospitals. Advanced devices can streamline workflows, enhance data management, and reduce the length of hospital stays. For instance, remote patient monitoring systems can decrease the need for frequent in-person visits to the hospital or clinic, thereby reducing healthcare costs. Additionally, the implementation of automated systems minimizes human error and increases the speed and accuracy of clinical processes.
Choosing the right medical equipment for your hospital is a strategic decision that profoundly affects the quality of healthcare, patient outcomes, and operational efficiency. It requires a comprehensive and well-thought-out approach that considers patient needs, safety, accuracy, reliability, training, technical support, and a detailed analysis of economic viability and long-term value.
Collaboration among doctors, technicians, and administrators is essential during the equipment selection process to ensure that the needs of all stakeholders are met. The selection of medical equipment should be viewed as an ongoing process that necessitates regular evaluation and updates to keep pace with technological advancements and changing patient needs. By making informed decisions, hospitals can ensure that they are equipped with the best medical equipment to provide high-quality and effective healthcare to their patients.
If you wish to receive comprehensive courses in the field of biomedical engineering to develop yourself and enhance your skills, HSI provides you with the necessary tools to ensure a bright future as a biomedical engineer. All you need to do is check out our services and contact us for more information.